## Diagnosis and Assessment of COPD **Key Point:** Spirometry is the gold standard investigation for diagnosis and severity classification of COPD. It provides objective, reproducible measurement of airflow obstruction. ### Why Spirometry with Bronchodilator Response? **High-Yield:** COPD diagnosis requires: 1. **FEV₁/FVC ratio < 0.70** (post-bronchodilator) — defines persistent airflow obstruction 2. **Bronchodilator response < 12% and < 200 mL** — distinguishes COPD from asthma 3. **FEV₁ classification** determines severity (GOLD criteria): - GOLD 1 (Mild): FEV₁ ≥ 80% predicted - GOLD 2 (Moderate): FEV₁ 50–79% predicted - GOLD 3 (Severe): FEV₁ 30–49% predicted - GOLD 4 (Very Severe): FEV₁ < 30% predicted **Clinical Pearl:** The **post-bronchodilator** measurement is mandatory because it confirms the obstruction is not fully reversible (unlike asthma) and provides the most accurate baseline for monitoring. **Mnemonic: COPD Diagnosis = FEV₁/FVC < 0.70 + Clinical Context** ### Role of Other Investigations | Investigation | Role in COPD | Limitation | |---|---|---| | HRCT | Identifies emphysema pattern, rules out alternative diagnoses | Not needed for routine diagnosis; adds cost and radiation | | ABG | Assesses gas exchange, detects hypoxemia/hypercapnia | Used for severity assessment and exacerbation management, not diagnosis | | DLCO | Reduced in emphysema, normal/high in chronic bronchitis | Prognostic marker, not diagnostic; helps phenotype | **Warning:** Do not confuse diagnostic spirometry with severity assessment — both use FEV₁, but diagnosis requires the FEV₁/FVC ratio and bronchodilator response. [cite:Harrison 21e Ch 254] 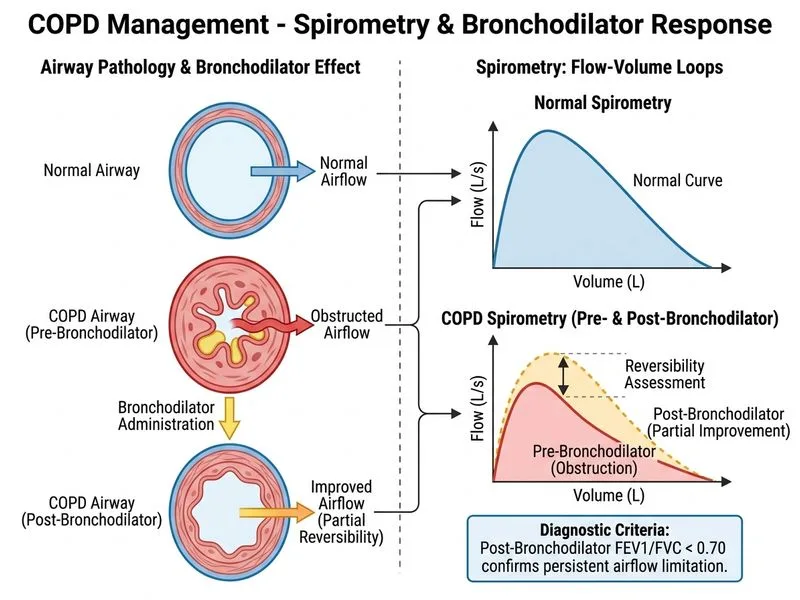
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.