## Clinical Assessment This patient presents with an **acute exacerbation of COPD** characterized by: - Increased dyspnea and sputum production (cardinal features) - Low-grade fever and systemic symptoms - Hypoxemia (SpO₂ 88%) - No radiological consolidation (excludes pneumonia as primary diagnosis) ## Management of COPD Exacerbation **Key Point:** Acute exacerbations of COPD require a dual approach—antimicrobial therapy for presumed bacterial infection and systemic corticosteroids to reduce airway inflammation and improve outcomes. ### Rationale for Oral Corticosteroids + Antibiotics Evidence-based guidelines recommend: | Intervention | Indication | Evidence | |---|---|---| | Systemic corticosteroids | All moderate-to-severe exacerbations | Reduces hospital stay, improves FEV₁ recovery | | Antibiotics | Exacerbation with purulent sputum ± fever | Targets bacterial colonization (H. influenzae, S. pneumoniae, M. catarrhalis) | | Oxygen therapy | SpO₂ < 90% | Target SpO₂ 88–92% to avoid CO₂ retention | **High-Yield:** Oral corticosteroids (prednisone 40–50 mg daily × 5 days) are non-inferior to IV steroids in outpatient/mild-to-moderate exacerbations and are preferred for ease of administration. **Clinical Pearl:** The presence of purulent sputum is a strong indicator of bacterial infection and justifies antibiotic use, even without infiltrate on CXR. ## Why NIV Is Not First-Line Here Non-invasive ventilation is reserved for: - Severe exacerbations with respiratory acidosis (pH < 7.35, PaCO₂ > 45 mmHg) - Failure of medical therapy - Impending respiratory failure This patient has mild-to-moderate hypoxemia without evidence of CO₂ retention and should be managed medically first. [cite:Harrison 21e Ch 297] 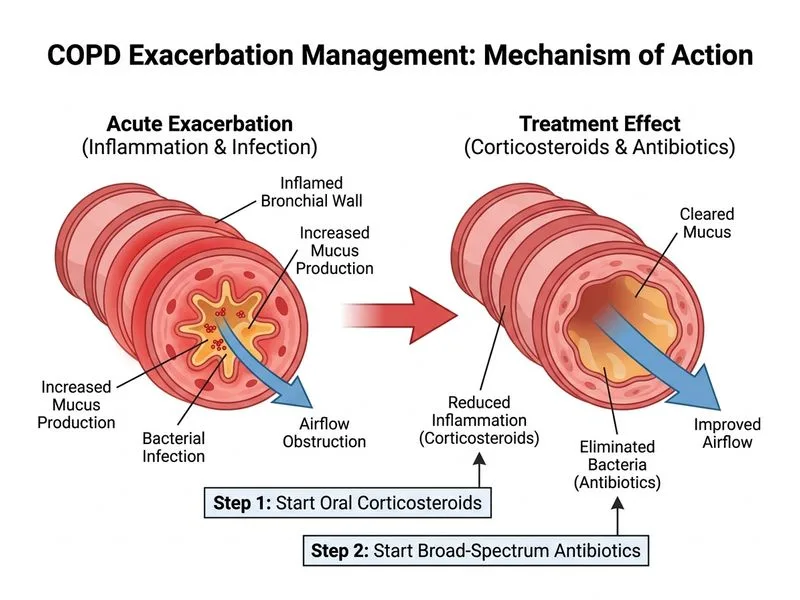
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.