## Diagnosis: Fungal Corneal Ulcer **Key Point:** The clinical presentation of a feathery ulcer with satellite lesions, hypopyon, and branching septate hyphae on KOH mount is pathognomonic for fungal keratitis, specifically a filamentous fungus (likely *Aspergillus* or *Fusarium*). **High-Yield:** Fungal corneal ulcers in India are endemic, particularly in agricultural populations with plant-related trauma. The classic triad is: 1. Feathery or serrated ulcer borders 2. Satellite lesions surrounding the main ulcer 3. Hypopyon (often more prominent than in bacterial ulcers) ### Management of Fungal Keratitis | Aspect | Fungal Ulcer | Bacterial Ulcer | |--------|--------------|----------------| | **First-line topical agent** | Natamycin 5% (polyene macrolide) | Fluoroquinolones (moxifloxacin, ciprofloxacin) | | **Frequency** | Hourly (or more frequently) | Hourly | | **Systemic adjunct** | Fluconazole 400 mg BD or itraconazole | Oral antibiotics (doxycycline, ciprofloxacin) | | **Topical steroids** | Contraindicated (promotes fungal spread) | Cautiously used after bacterial infection controlled | | **Prognosis** | Guarded; higher risk of scarring | Better with early treatment | **Clinical Pearl:** Natamycin is the preferred topical antifungal because it has excellent corneal penetration and is fungistatic (not fungicidal, but sufficient for topical use). Systemic fluconazole or itraconazole is essential for deep stromal or endothelial involvement. **Warning:** Topical corticosteroids are absolutely contraindicated in fungal keratitis — they suppress local immunity and promote fungal proliferation, leading to rapid progression and perforation. ### Why Natamycin + Fluconazole? 1. **Natamycin 5%** — gold standard topical antifungal for filamentous fungi (does not penetrate well systemically, so must be used topically) 2. **Systemic fluconazole** — achieves therapeutic levels in aqueous humor and vitreous; covers both *Candida* and *Aspergillus* species 3. **Hourly frequency** — fungal ulcers progress rapidly and require aggressive topical therapy **Mnemonic:** **NAF** = **N**atamycin + **A**ntifungal (systemic) + **F**ungal keratitis [cite:Khurana 7e Ch 5] 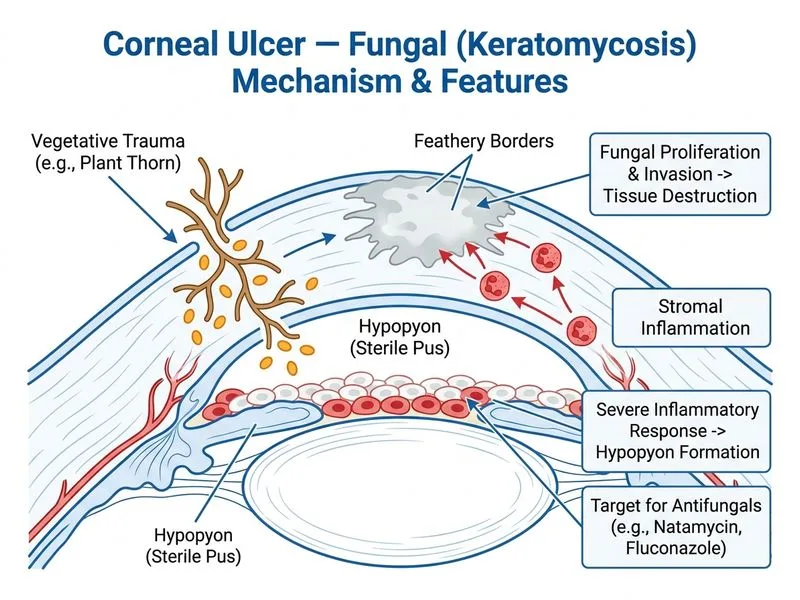
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.