## Diagnosis: Bacterial Corneal Ulcer (Staphylococcal) **Key Point:** Gram-positive cocci in clusters indicate *Staphylococcus aureus*, the most common cause of bacterial keratitis in India. The well-demarcated, round infiltrate with a smooth base is typical of staphylococcal ulcers. **High-Yield:** Bacterial corneal ulcers present with: - Acute onset (hours to 1–2 days) - Well-defined, round or oval infiltrate - Smooth ulcer base - Hypopyon (often 1–3 mm) - Purulent discharge ### Bacterial vs. Fungal Corneal Ulcer Comparison | Feature | Bacterial | Fungal | |---------|-----------|--------| | **Onset** | Acute (hours to 1–2 days) | Insidious (days to weeks) | | **Ulcer border** | Well-demarcated, round/oval | Feathery, serrated, irregular | | **Satellite lesions** | Absent | Present | | **Hypopyon** | 1–3 mm, resolves quickly | Larger, persistent | | **Infiltrate appearance** | Yellow-white, smooth base | Gray-white, granular | | **Pain severity** | Moderate to severe | Mild to moderate | | **Gram stain** | Cocci or rods | Hyphae (KOH mount) | ### Initial Empirical Therapy for Bacterial Keratitis **Fortified antibiotics** are the standard of care for bacterial corneal ulcers: 1. **Fortified Cefazolin 5%** — broad-spectrum coverage against gram-positive and some gram-negative organisms - Prepared by diluting IV cefazolin (500 mg/mL) with normal saline - Excellent corneal penetration 2. **Fortified Gentamicin 1.4%** — covers gram-negative organisms and *Pseudomonas* - Prepared from gentamicin injection (40 mg/mL) - Synergistic with cephalosporins 3. **Frequency:** Hourly (or every 30 minutes in severe cases) for first 48–72 hours, then taper based on clinical response **Clinical Pearl:** Fortified antibiotics achieve much higher corneal concentrations than commercially available topical preparations. They are essential for aggressive bacterial keratitis, especially in high-risk settings (trauma, contact lens wear, immunocompromised). **Mnemonic:** **FCFG** = **F**ortified **C**efazolin + **F**ortified **G**entamicin (for bacterial keratitis) ### Why Fortified Cefazolin + Gentamicin? - **Cefazolin** covers *Staphylococcus aureus* (gram-positive cocci in clusters) - **Gentamicin** provides additional gram-negative coverage and synergy - **Fortified formulations** achieve therapeutic corneal levels (10–20× higher than commercial drops) - **Hourly dosing** prevents bacterial proliferation in the avascular cornea **Warning:** Do NOT use monotherapy with a single antibiotic — resistance may develop rapidly. Always use a combination of fortified agents. [cite:Khurana 7e Ch 5; Sharma & Srinivasan, *Bacterial Keratitis*, 2023] 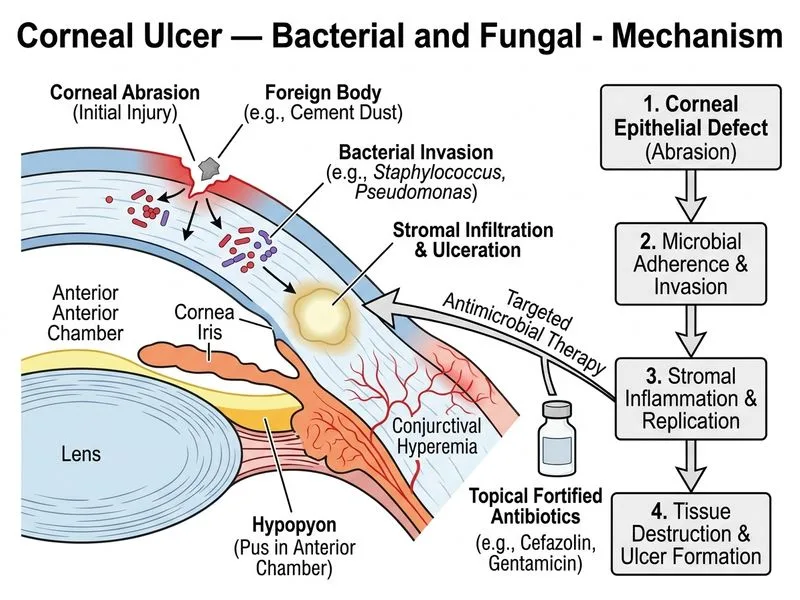
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.