## Clinical Context The patient has clinical features of Cushing syndrome (central obesity, purple striae, proximal weakness, hypertension, amenorrhea) with elevated morning cortisol (28 µg/dL) and failure of suppression on LDDST (18 µg/dL). The LDDST is abnormal, confirming cortisol excess, but the diagnosis of Cushing syndrome itself must be established before proceeding to subtype differentiation. ## Diagnostic Algorithm for Cushing Syndrome **Key Point:** Diagnosis of Cushing syndrome requires confirmation with at least TWO abnormal screening tests before proceeding to localization studies. A single abnormal LDDST is insufficient; additional confirmatory tests are mandatory. **High-Yield:** The three confirmatory tests for Cushing syndrome are: 1. 24-hour urinary free cortisol (UFC) — elevated (>50 µg/24 hr) 2. Late-night salivary cortisol — elevated (>7.5 µg/dL at midnight) 3. LDDST — cortisol >5 µg/dL after 1 mg dexamethasone At least TWO abnormal tests are needed to diagnose Cushing syndrome [cite:Harrison 21e Ch 375]. ## Why This Is the Next Step **Clinical Pearl:** Although LDDST is abnormal here, confirming the diagnosis with a second independent test (24-hour UFC or late-night salivary cortisol) is the standard diagnostic pathway. This prevents false positives from pseudo-Cushing states (depression, obesity, alcoholism, critical illness) and ensures the diagnosis before expensive and invasive localization studies. ## Pathway After Confirmation Once Cushing syndrome is confirmed, the next step is ACTH measurement: - **ACTH <10 pg/mL** → ACTH-independent (adrenal source) → Adrenal CT/MRI - **ACTH ≥10 pg/mL** → ACTH-dependent → HDDST and pituitary MRI **Mnemonic:** **CONFIRM before LOCATE** — Always confirm Cushing syndrome with two tests before ordering localization imaging. 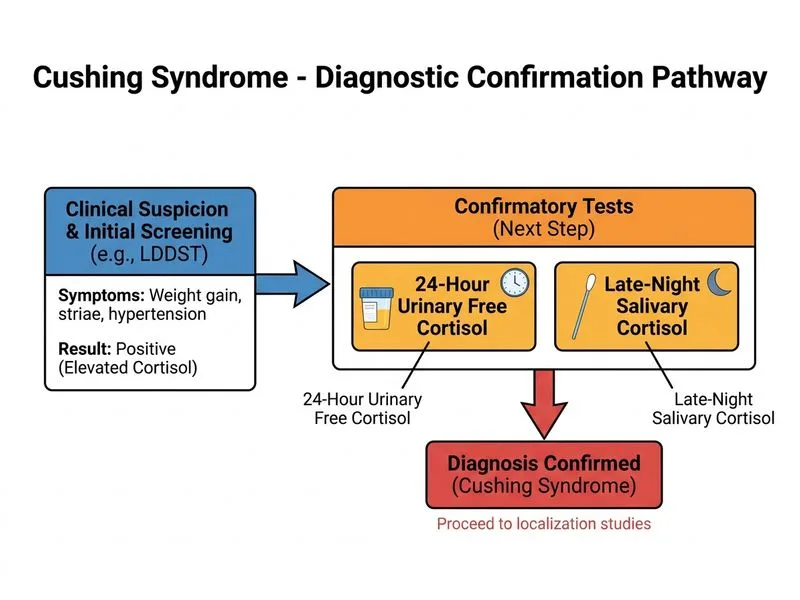
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.