## Distinguishing Primary Adrenal from ACTH-Dependent Cushing Syndrome ### Pathophysiology The key difference between primary adrenal and ACTH-dependent Cushing syndrome lies in the feedback axis: **Key Point:** In primary adrenal Cushing, the adrenal tumor secretes cortisol autonomously, suppressing pituitary ACTH via negative feedback. In ACTH-dependent Cushing, elevated ACTH drives adrenal cortisol production, and the feedback loop is disrupted. ### Plasma ACTH: The Discriminating Feature | Feature | Primary Adrenal Cushing | ACTH-Dependent Cushing (Pituitary/Ectopic) | |---------|-------------------------|---------------------------------------------| | **Plasma ACTH** | **Suppressed (<10 pg/mL)** | **Elevated (>20 pg/mL)** | | **Mechanism** | Autonomous cortisol production suppresses pituitary ACTH | Ectopic or pituitary ACTH drives adrenal secretion | | **Imaging finding** | Adrenal nodule/mass on CT | Pituitary adenoma or ectopic tumor | | **LDDST response** | No suppression | May show partial suppression (pituitary) or no suppression (ectopic) | | **Cortisol source** | Adrenal gland | ACTH-secreting tumor | ### Why Plasma ACTH is the Best Discriminator **High-Yield:** Plasma ACTH is the single most useful test to separate primary adrenal from ACTH-dependent Cushing syndrome. A suppressed ACTH (<10 pg/mL) in the presence of elevated cortisol is pathognomonic for primary adrenal disease. An elevated ACTH (>20 pg/mL) indicates ACTH-dependent Cushing and mandates further testing (HDDST, imaging) to localize the source. **Clinical Pearl:** The patient described has no suppression on LDDST, which is consistent with either primary adrenal or ectopic ACTH Cushing. The next step would be to measure plasma ACTH. If suppressed, primary adrenal disease is confirmed; if elevated, ACTH-dependent Cushing is confirmed, and HDDST would then distinguish pituitary from ectopic. ### Mnemonic **ACTH Axis Tells All (ATA)** — Suppressed ACTH = primary adrenal; elevated ACTH = ACTH-dependent Cushing. ### Why Other Options Are Non-Discriminatory - **Elevated UFC:** Present in all forms of Cushing syndrome; does not distinguish source. - **Proximal myopathy & hypertension:** Common to all Cushing phenotypes; not specific to adrenal vs. ACTH-dependent. - **Elevated midnight salivary cortisol:** Confirms hypercortisolism but is present in both primary adrenal and ACTH-dependent Cushing. [cite:Harrison 21e Ch 387] 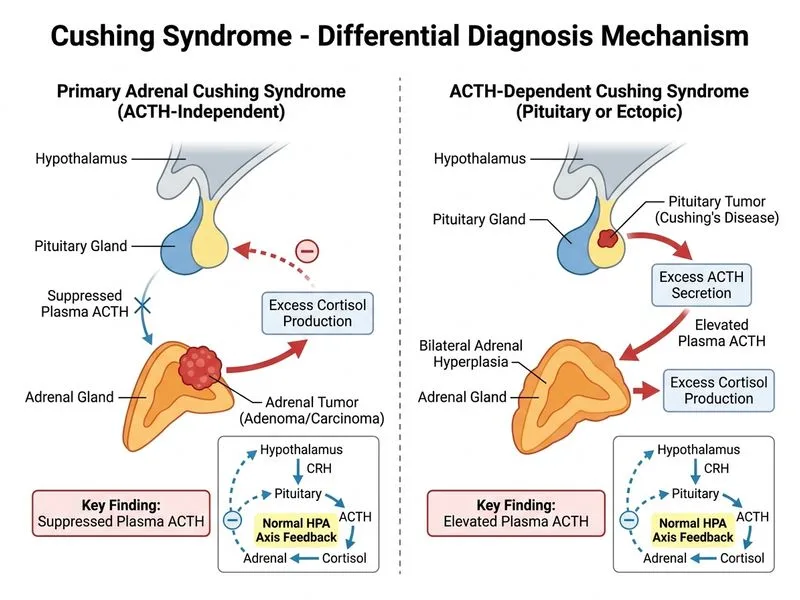
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.