## Diagnosis: Cortisol-Secreting Adrenocortical Adenoma ### Clinical Presentation This patient presents with classic features of Cushing syndrome: central obesity, proximal myopathy, amenorrhea, hypertension, easy bruising, and purple striae. The 6-month duration and gradual onset are typical of an adenoma rather than acute ectopic ACTH syndrome. ### Laboratory Interpretation | Finding | Value | Interpretation | |---------|-------|----------------| | 24-hr UFC | 450 µg/day | Markedly elevated (>10× normal) | | Morning cortisol | 28 µg/dL | Severely elevated | | ACTH | 8 pg/mL | **Suppressed** (normal or low) | | LDDST cortisol | 22 µg/dL | No suppression (<50% reduction) | **Key Point:** The **suppressed ACTH** with elevated cortisol is the diagnostic hallmark of **primary adrenocortical pathology** (adenoma or carcinoma). This distinguishes it from ACTH-dependent Cushing syndrome (pituitary or ectopic). ### Differential Diagnosis Logic ```mermaid flowchart TD A[Cushing Syndrome Confirmed]:::outcome --> B{ACTH Level?}:::decision B -->|Low/Normal| C[ACTH-Independent]:::outcome B -->|Elevated| D[ACTH-Dependent]:::outcome C --> E{Imaging: Unilateral or Bilateral?}:::decision E -->|Unilateral mass| F[Adrenocortical Adenoma]:::action E -->|Bilateral hyperplasia| G[Primary Pigmented Nodular Adrenocortical Disease]:::outcome E -->|Unilateral mass + aggressive features| H[Adrenocortical Carcinoma]:::urgent D --> I{LDDST suppression?}:::decision I -->|Yes| J[Pituitary adenoma]:::outcome I -->|No| K[Ectopic ACTH]:::outcome ``` ### Why This Is Adenoma, Not Carcinoma **High-Yield:** Adrenocortical **adenoma** typically: - Presents with insidious onset over months to years - Produces only cortisol (pure cortisol-secreting) - Has suppressed ACTH - Shows no LDDST suppression (autonomous secretion) - Imaging: small (<4 cm), well-circumscribed, unilateral - Prognosis: excellent after adrenalectomy **Adrenocortical carcinoma** typically: - More aggressive presentation - Often secretes multiple hormones (cortisol + androgens + aldosterone) - Elevated DHEA-S (often >700 µg/dL) - Larger mass (>4 cm), irregular borders, invasion - Elevated 17-hydroxyprogesterone and other precursors This patient's presentation (gradual onset, pure cortisol excess, suppressed ACTH, no mention of virilization or hypokalemia) is consistent with **benign adenoma**. ### Clinical Pearl **Warning:** Do NOT confuse ACTH suppression with pituitary disease. In pituitary Cushing syndrome, ACTH is **elevated** (though lower than in ectopic ACTH). The **suppressed ACTH** here rules out pituitary adenoma immediately. ### Next Step Confirm with abdominal CT or MRI to visualize a unilateral adrenal mass, then proceed to adrenalectomy for definitive cure. 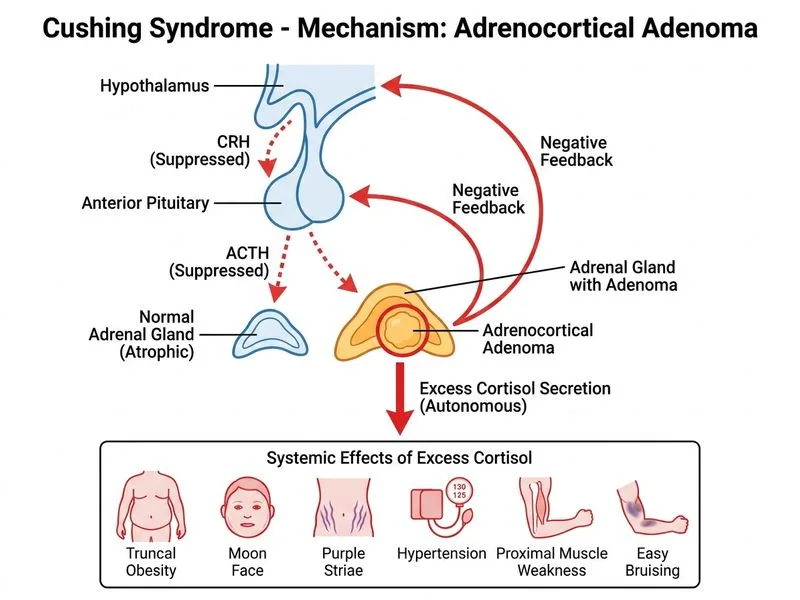
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.