## Clinical Diagnosis The patient has **proliferative diabetic retinopathy (PDR) with vitreous hemorrhage secondary to neovascularization of the disc (NVD)**. ### Why PDR with NVD? **Key Point:** In a long-standing diabetic (18 years) with suboptimal glycemic control presenting with sudden vitreous hemorrhage, PDR is the most likely diagnosis. The vitreous hemorrhage in PDR occurs when fragile new vessels bleed into the vitreous cavity. ### Pathophysiology of Vitreous Hemorrhage in PDR ```mermaid flowchart TD A[Chronic hyperglycemia]:::outcome --> B[Retinal ischemia]:::outcome B --> C[VEGF upregulation]:::outcome C --> D[Neovascularization]:::outcome D --> E{Vessel fragility}:::decision E -->|Vitreous traction| F[Vessel rupture]:::urgent E -->|Spontaneous rupture| G[Vitreous hemorrhage]:::urgent F --> G G --> H[Vision loss]:::outcome ``` ### Clinical Features Supporting PDR | Feature | Significance | |---------|-------------| | Long diabetes duration (18 years) | Risk factor for PDR; typically occurs after 10-15 years of DM | | Suboptimal HbA1c (8.8%) | Poor glycemic control accelerates progression to PDR | | Sudden floaters + blurred vision | Classic presentation of vitreous hemorrhage | | Hand movements vision | Indicates dense hemorrhage obscuring posterior pole | | No retinal detachment on B-scan | Rules out tractional RD; confirms hemorrhage as primary problem | | No trauma history | Excludes traumatic causes | **High-Yield:** PDR is the leading cause of vitreous hemorrhage in diabetic patients. The new vessels are fragile because they lack a normal blood-retinal barrier and are prone to rupture, especially with vitreous traction or Valsalva maneuver. ### Management Approach 1. **Immediate:** Strict bed rest, head elevation, avoid Valsalva (constipation prevention) 2. **Imaging:** Fluorescein angiography (once hemorrhage clears) or OCT-angiography to confirm NVD 3. **Treatment:** Panretinal photocoagulation (PRP) or anti-VEGF injections (bevacizumab, ranibizumab, aflibercept) 4. **Vitrectomy:** If hemorrhage does not clear within 3 months or if tractional RD develops **Clinical Pearl:** Even though the posterior pole is obscured, the diagnosis of PDR is highly likely given the clinical context. Confirmation with imaging (FA or OCT-A) should follow once hemorrhage clears or after vitrectomy. [cite:Yanoff & Duker 6e Ch 6] 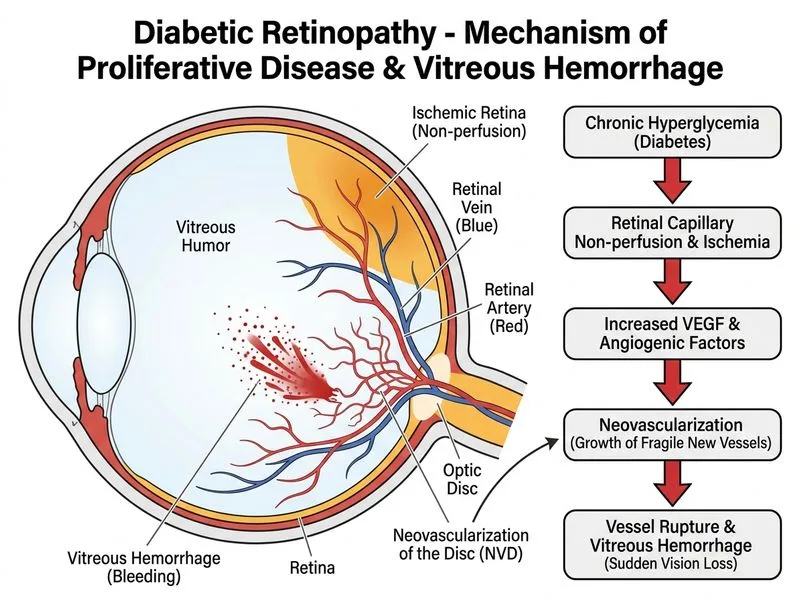
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.