## Clinical Diagnosis: Proliferative Diabetic Retinopathy (PDR) with Vitreous Hemorrhage ### Key Clinical Features Present | Feature | Significance | |---------|-------------| | Extensive hemorrhages (dot, blot, flame) | Indicates severe microvascular disease | | Cotton-wool spots | Nerve fiber layer infarcts; sign of severe ischemia | | Venous beading | Venous dilation and tortuosity; marker of severe ischemia | | Retinal whitening (hard exudates/edema) | Lipid leakage and tissue edema | | Hyperemic optic disc | Neovascularization of disc (NVD) | | Sudden floaters + vision loss | Vitreous hemorrhage obscuring view | **High-Yield:** The combination of **venous beading + cotton-wool spots + extensive hemorrhages = severe NPDR progressing to PDR**. The hyperemic disc indicates **neovascularization of the disc (NVD)**, which is PDR by definition. ## Pathophysiology of Vitreous Hemorrhage in PDR ```mermaid flowchart TD A[Severe retinal ischemia]:::outcome --> B[Upregulation of VEGF]:::outcome B --> C[Neovascularization of disc & elsewhere]:::outcome C --> D[Fragile new vessels]:::outcome D --> E{Mechanical traction or vitreous contraction?}:::decision E -->|Yes| F[Vessel rupture]:::urgent F --> G[Vitreous hemorrhage]:::urgent G --> H[Vision loss, floaters, media opacity]:::outcome H --> I[Urgent vitrectomy needed]:::action ``` ## Why Vitrectomy is Urgent **Key Point:** Vitreous hemorrhage in PDR is a **vision-threatening emergency**. Unlike NPDR, where hemorrhages may reabsorb spontaneously, vitreous hemorrhage in PDR carries high risk of: 1. **Tractional retinal detachment (TRD)** — new vessels pull the retina 2. **Permanent vision loss** if not cleared promptly 3. **Neovascular glaucoma** if ischemia worsens **Clinical Pearl:** The presence of NVD (hyperemic optic disc) + vitreous hemorrhage = **PDR with vitreous hemorrhage**, which mandates **urgent vitrectomy** (within days to weeks, not months). Waiting for spontaneous clearing risks TRD and irreversible blindness. ## Management Hierarchy for PDR ```mermaid flowchart TD A[PDR confirmed]:::outcome --> B{Vitreous hemorrhage?}:::decision B -->|Yes| C[Urgent vitrectomy]:::urgent B -->|No| D{NVD or NVE?}:::decision D -->|Yes| E[Panretinal photocoagulation]:::action D -->|No| F[Close monitoring]:::action C --> G[Vitrectomy + PRP/laser intraoperatively]:::action ``` ## Why Other Options Are Wrong **Option A (Severe NPDR; PRP after OCT):** This is **PDR, not NPDR**. The presence of NVD (hyperemic disc) defines PDR. While PRP is part of PDR management, vitreous hemorrhage takes precedence—you cannot perform effective PRP through blood-filled vitreous. Vitrectomy must come first. **Option C (CRVO; anticoagulation/steroids):** CRVO presents with **retinal hemorrhages in all quadrants + cotton-wool spots + venous dilation**, which can mimic severe DR. However, CRVO is typically **unilateral and acute**, with **cherry-red spot at macula** (not mentioned), and **no neovascularization of disc**. The hyperemic disc and long diabetes history point to PDR, not CRVO. **Option D (ARN; IV acyclovir):** Acute retinal necrosis presents with **granular retinal opacification, hemorrhage, and rapid progression**, but is typically **associated with pain, anterior uveitis, and viral prodrome** (not mentioned). ARN is rare in diabetics and would not explain the long-standing diabetic changes (cotton-wool spots, venous beading). ## Immediate Management Steps 1. **Urgent vitrectomy** (within 1–2 weeks) to clear hemorrhage and prevent TRD 2. **Intraoperative PRP or endolaser** to ablate ischemic retina and reduce VEGF 3. **Tight glycemic and blood pressure control** perioperatively 4. **Anti-VEGF injections** (bevacizumab, ranibizumab) may be given preoperatively to regress new vessels and reduce bleeding risk [cite:Parson's Diseases of the Eye 22e Ch 11; ETDRS Report No. 2] 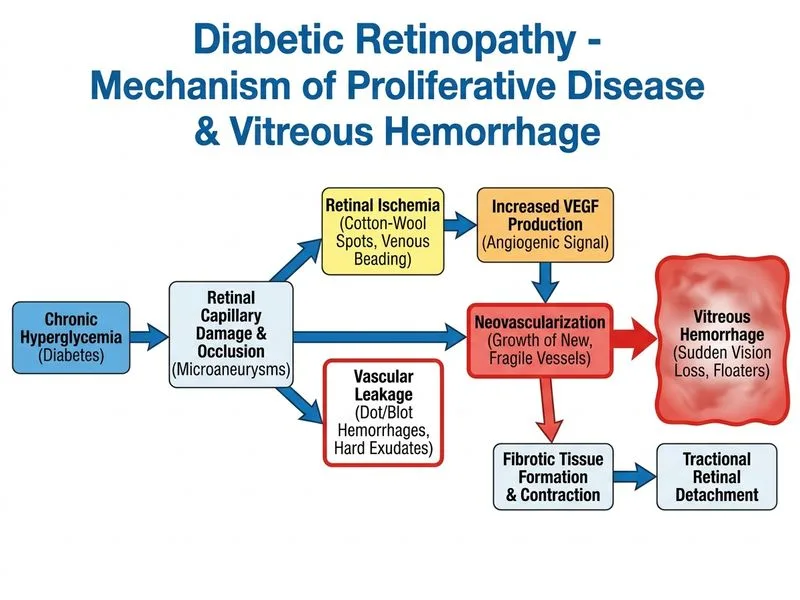
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.