## Pathophysiology of DIC in Malignancy ### The Coagulation Cascade in DIC ```mermaid flowchart TD A[Malignant cells release Tissue Factor]:::outcome --> B[TF binds Factor VII]:::action B --> C[Extrinsic pathway activation]:::action C --> D[Thrombin generation]:::outcome D --> E[Fibrinogen → Fibrin]:::action E --> F[Microthrombi formation]:::outcome F --> G[Platelet consumption]:::outcome F --> H[Factor consumption]:::outcome G --> I[Thrombocytopenia]:::outcome H --> I D --> J[Plasmin activation]:::action J --> K[Fibrin degradation]:::outcome K --> L[Elevated D-dimer & FDP]:::outcome ``` ### Mechanism in This Patient **Key Point:** DIC in malignancy is primarily driven by **tissue factor (TF) expression on cancer cells** and **cancer-derived microparticles**. 1. **Tissue Factor Release** - Adenocarcinoma cells (especially pancreatic, lung, gastric) express high levels of TF on their surface - TF is a transmembrane glycoprotein that directly activates Factor VII → Factor VIIa - This bypasses the intrinsic pathway and directly triggers the extrinsic cascade 2. **Extrinsic Pathway Activation** - TF + Factor VIIa → Factor X activation → Factor Xa - Factor Xa + Factor Va → prothrombin activation → **thrombin generation** - Thrombin converts fibrinogen → fibrin → microthrombi in small vessels 3. **Consumption Phase** - Platelets are trapped in fibrin strands → thrombocytopenia (35,000/μL) - Clotting factors (II, V, VII, X, fibrinogen) are consumed → prolonged PT/aPTT, low fibrinogen - Fibrin is degraded by plasmin → elevated D-dimer and FDP 4. **Secondary Fibrinolysis** - Thrombin activates plasminogen → plasmin - Plasmin degrades fibrin → fibrin degradation products (FDP) - FDP inhibit platelet aggregation and thrombin generation → bleeding paradox ### Laboratory Interpretation | Test | Finding | Mechanism | |------|---------|----------| | **PT** | ↑ (22 sec) | Factor VII, X, II, V consumed | | **aPTT** | ↑ (58 sec) | Factor VIII, IX, XI, XII, II, V consumed | | **Fibrinogen** | ↓ (110 mg/dL) | Converted to fibrin; degraded by plasmin | | **D-dimer** | ↑↑↑ (>10 μg/mL) | **Most sensitive marker** — fibrin degradation | | **Platelets** | ↓ (35,000) | Consumption in microthrombi | | **Schistocytes** | Present | RBC fragmentation from fibrin strands | | **LDH** | ↑ (680 U/L) | Hemolysis from mechanical damage | **Clinical Pearl:** Schistocytes on blood smear indicate **mechanical hemolysis** from fibrin strands — a hallmark of DIC. This distinguishes DIC from immune thrombocytopenia or drug-induced thrombocytopenia. ### Why Malignancies Cause DIC **High-Yield:** Solid tumors most commonly associated with DIC: 1. **Adenocarcinomas** (pancreatic, lung, gastric, colon) — highest risk 2. **Acute promyelocytic leukemia (APL)** — 80–90% of cases 3. **Acute monocytic leukemia** — tissue factor-rich blasts 4. **Prostate cancer** — tissue factor expression ### Bleeding Paradox in DIC Despite **activation** of coagulation (which should cause thrombosis), patients bleed because: - Platelets and factors are **consumed faster than produced** - Fibrin degradation products **inhibit platelet function and thrombin generation** - Plasmin **degrades fibrinogen and factors V and VIII** - Net result: **consumption coagulopathy** (hypocoagulable state) → bleeding **Mnemonic: TISSUE FACTOR in Malignancy** - **T**issue factor expression on cancer cells - **I**ntrinsic pathway bypassed - **S**equential consumption of platelets and factors - **S**econdary fibrinolysis activated - **U**ncontrolled thrombin generation - **E**xtrinsic pathway triggered - **F**ibrin microthrombi → hemolysis (schistocytes) - **A**ctivated plasmin → FDP elevation - **C**oagulopathy (consumption) → bleeding - **T**hrombocytopenia + prolonged PT/aPTT + low fibrinogen - **O**ver-activation of coagulation - **R**esult: bleeding paradox 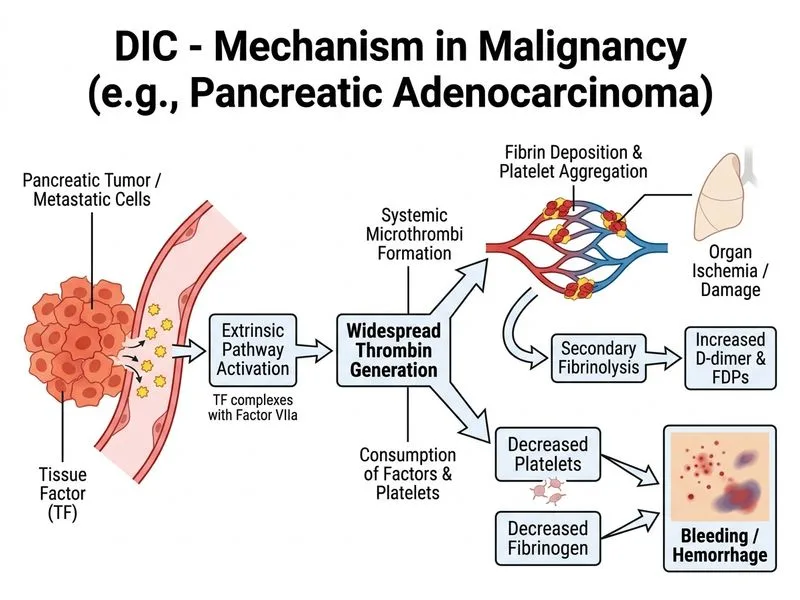
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.