## Difficult Airway Algorithm — Failed Intubation Management **Key Point:** When direct laryngoscopy fails in an anesthetized, paralyzed patient, the algorithm mandates a structured escalation: call for help, then attempt alternative techniques (video laryngoscopy, flexible scope, bougie) BEFORE resorting to surgical airway. **High-Yield:** The difficult airway algorithm distinguishes between: - **Failed intubation** (cannot pass tube despite good visualization) - **Failed oxygenation** (cannot maintain SpO₂ ≥ 90% despite rescue maneuvers) In this case, the patient has Grade III view (epiglottis only), which is a **failed intubation scenario**, not yet a failed oxygenation emergency. The algorithm prioritizes: 1. **Call for help** — senior anesthesia, ENT, surgical airway team 2. **Attempt rescue techniques** — video laryngoscope (often succeeds where direct laryngoscopy fails), bougie, flexible scope 3. **Surgical airway only if** — oxygenation fails despite all rescue attempts **Clinical Pearl:** Video laryngoscopy has a significantly higher success rate than direct laryngoscopy in difficult airways because it bypasses the need for oral-pharyngeal axis alignment. It should be the first rescue technique in an anesthetized patient with failed DL. **Mnemonic: CICO** — Can't Intubate, Can't Oxygenate. Surgical airway is reserved for CICO, not for simple failed intubation. ### Why Video Laryngoscopy Works Here - Patient is already anesthetized and paralyzed (no time for awake fiberoptic) - Bougie alone without visualization is less reliable as a first rescue - Video laryngoscope provides superior visualization angles and often upgrades Grade III to Grade I/II - Preserves oxygenation window while attempting alternative intubation [cite:Difficult Airway Society Guidelines 2015] 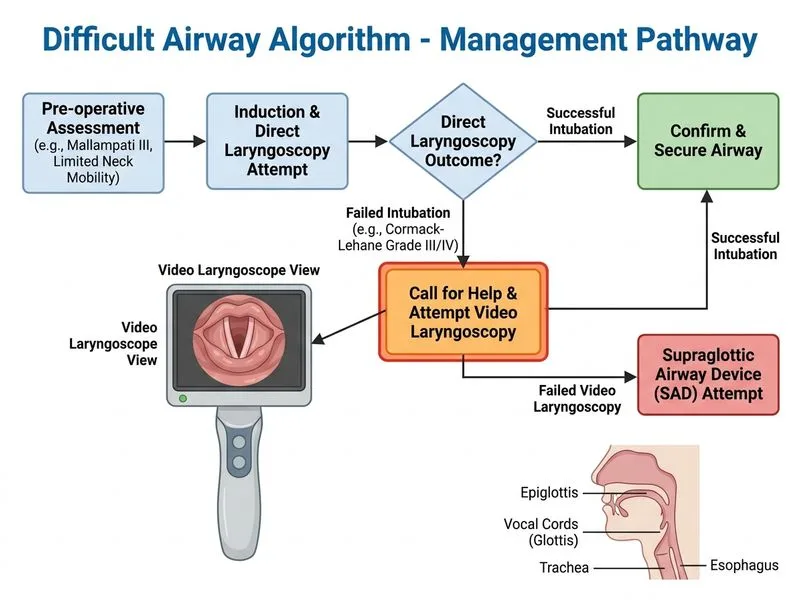
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.