## Diagnosis: Atrial Fibrillation with Controlled Ventricular Response ### ECG Hallmarks of Atrial Fibrillation **Key Point:** Atrial fibrillation (AF) is characterized by the **absence of organized P waves** and **irregular RR intervals** (irregularly irregular rhythm). These two findings are pathognomonic. ### Diagnostic Criteria | Feature | Atrial Fibrillation | Finding in This Case | |---|---|---| | P waves | Absent; replaced by irregular baseline fibrillation waves (f waves) | Absent ✓ | | RR intervals | Completely irregular (no pattern) | Irregularly irregular ✓ | | Ventricular rate | Variable; depends on AV node conduction | 70–100 bpm (controlled) ✓ | | QRS duration | Normal (0.08–0.12 s) unless aberrant conduction | 0.08 s (normal) ✓ | | Atrial rate | 300–600 bpm (not visible on surface ECG) | Not applicable | **High-Yield:** AF is the most common sustained arrhythmia in clinical practice, affecting 1–2% of the general population. Prevalence increases sharply with age and in the presence of structural heart disease, hypertension, and diabetes. ### Ventricular Rate Control Classification **Mnemonic: RVR** = Rapid Ventricular Response - **Controlled AF:** Ventricular rate 60–100 bpm at rest → no acute intervention needed - **Rapid AF (RVR):** Ventricular rate >100 bpm → requires rate control (beta-blocker, calcium channel blocker, or digoxin) - **Slow AF:** Ventricular rate <60 bpm → consider pacemaker if symptomatic This patient has a ventricular rate of 70–100 bpm, which falls within the **controlled range**. ### Pathophysiology Atrial fibrillation results from: 1. **Ectopic foci** in the pulmonary veins firing at rapid rates (300–600 bpm) 2. **Reentry circuits** within the atria 3. **AV node acts as a gatekeeper**, conducting only a fraction of atrial impulses irregularly to the ventricles 4. This produces the characteristic **irregularly irregular ventricular rhythm** **Clinical Pearl:** The AV node has a refractory period that prevents 1:1 conduction of all atrial impulses, thereby protecting the ventricles from excessively rapid rates. Without this, the ventricular rate could exceed 300 bpm and cause hemodynamic collapse. ### Risk Factors in This Patient - **Age 72 years** (non-modifiable) - **Hypertension** (major modifiable risk factor) - **Diabetes mellitus** (increases AF risk 1.4–1.6 fold) ### Management Approach **Key Point:** In AF with controlled ventricular response and no acute hemodynamic compromise: 1. **Rate control** (beta-blocker, diltiazem, or verapamil) — target HR 60–100 bpm at rest 2. **Anticoagulation** — assess CHA₂DS₂-VASc score for stroke risk (this patient likely qualifies for anticoagulation given age + hypertension + diabetes) 3. **Rhythm control** (if indicated) — antiarrhythmic drugs or catheter ablation 4. **Treat underlying conditions** — optimize BP and glycemic control [cite:Harrison 21e Ch 296] 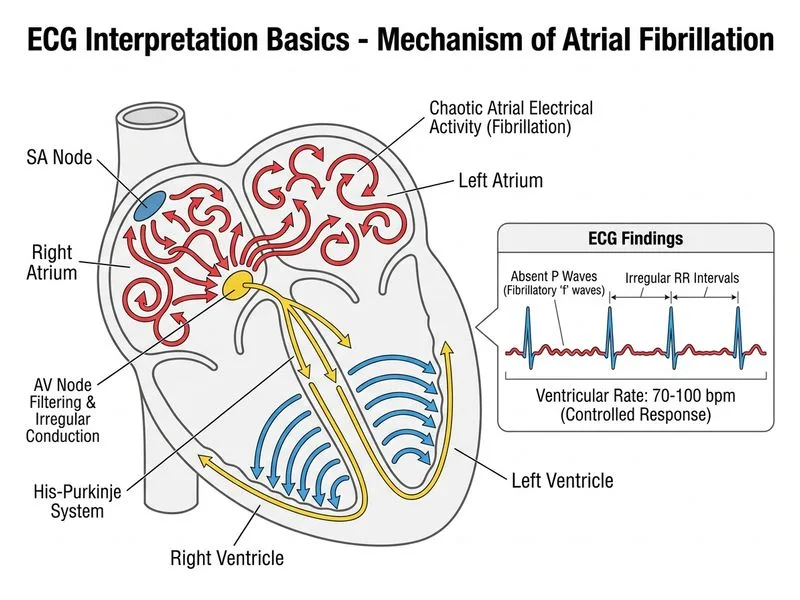
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.