## ESBL Mechanism and Resistance Pattern **Key Point:** Extended-spectrum beta-lactamases (ESBLs) are mutant derivatives of TEM-1, TEM-2, and SHV-1 beta-lactamases that have acquired the ability to hydrolyze third-generation cephalosporins (ceftriaxone, cefotaxime) and monobactams (aztreonam), but retain susceptibility to carbapenems and beta-lactamase inhibitors. ## Clinical Context This patient's resistance pattern is classic for ESBL-producing Enterobacteriaceae: - **Resistant to:** 3rd-generation cephalosporins, monobactams - **Susceptible to:** Carbapenems (meropenem, imipenem), aminoglycosides, fluoroquinolones (though this isolate may have acquired resistance through prior exposure) - **Confirmatory test:** Positive ESBL confirmation disk diffusion (cephalosporin ± clavulanic acid) ## Mechanism of ESBL Resistance ```mermaid flowchart TD A[ESBL-producing organism]:::outcome --> B[TEM or SHV mutant beta-lactamase]:::action B --> C[Hydrolysis of 3rd-gen cephalosporins]:::action C --> D[Resistance to ceftriaxone, cefotaxime]:::outcome B --> E[Hydrolysis of monobactams]:::action E --> F[Resistance to aztreonam]:::outcome B --> G[Cannot hydrolyze carbapenems]:::action G --> H[Susceptibility maintained]:::outcome ``` **High-Yield:** ESBLs are inhibited by clavulanic acid and beta-lactamase inhibitors, but carbapenems are NOT substrates for ESBL hydrolysis due to their unique beta-lactam ring structure and stability. ## Why Carbapenems Work Carbapenems have a different bicyclic structure and are highly resistant to hydrolysis by ESBLs. They remain the drug of choice for serious ESBL-producing gram-negative infections [cite:Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases Ch 211]. **Clinical Pearl:** Prior fluoroquinolone exposure is a major risk factor for ESBL acquisition in UTIs, as seen in this patient's history of recurrent infections treated with fluoroquinolones. 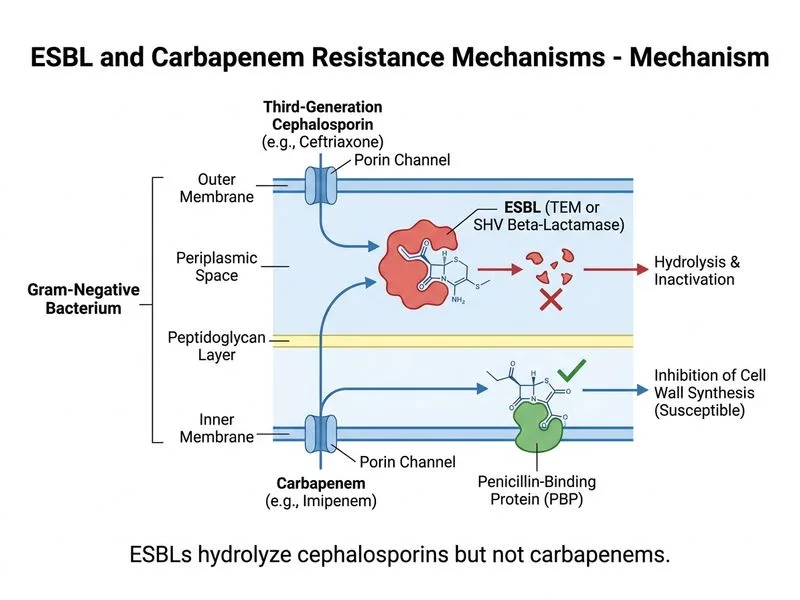
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.