## Clinical Context This patient has **carbapenem-resistant Enterobacteriaceae (CRE)** producing a metallo-β-lactamase (NDM-1). This is a pan-resistant organism with extremely limited treatment options. The presence of bla-NDM-1 confirms true carbapenem resistance, not ESBL. ## Carbapenem Resistance Mechanisms: ESBL vs. MBL | Feature | ESBL | Metallo-β-lactamase (NDM-1, VIM, IMP) | |---------|------|----------------------------------------| | Substrate | 3rd/4th gen cephalosporins, aztreonam | **Carbapenems + cephalosporins** | | Carbapenem susceptibility | **Susceptible** | **Resistant** | | Mechanism | Serine active site | **Zinc-dependent metalloenzyme** | | Inhibitor | Clavulanic acid, tazobactam | **Not inhibited by β-lactamase inhibitors** | | Treatment | Carbapenems (1st line) | Colistin, tigecycline, fosfomycin | **Key Point:** Metallo-β-lactamases (MBLs) are zinc-dependent enzymes that hydrolyze carbapenems. Unlike ESBLs, they are NOT inhibited by conventional β-lactamase inhibitors (clavulanic acid, tazobactam, sulbactam). NDM-1 is the most common MBL globally, first identified in New Delhi. ## Why Colistin Is the Next Step **High-Yield:** Colistin (polymyxin E) is a last-resort antibiotic for CRE/NDM-1 infections because: 1. It remains active against most MBL-producing organisms 2. It acts via membrane disruption (not β-lactam hydrolysis), bypassing resistance mechanisms 3. It is bactericidal at high concentrations 4. Alternatives (tigecycline, fosfomycin) have lower bactericidal activity and higher failure rates in sepsis **Clinical Pearl:** Colistin dosing in renal impairment requires adjustment. With serum creatinine 1.8 mg/dL (estimated CrCl ~30–40 mL/min), the patient needs dose reduction. Standard loading dose is 9 million units IV, then maintenance 4.5 million units IV 8-hourly (or 3 million units 12-hourly if CrCl <10 mL/min). Renal function monitoring is essential. ## Management Algorithm for CRE/NDM-1 ```mermaid flowchart TD A[CRE/NDM-1 infection confirmed]:::outcome A --> B{Clinical severity?}:::decision B -->|Sepsis/Bacteremia| C[Colistin IV ± tigecycline]:::action B -->|Uncomplicated UTI| D[Fosfomycin or tigecycline]:::action C --> E[Blood cultures before therapy]:::action E --> F[Source control: remove catheter if possible]:::action F --> G[Monitor renal function closely]:::action G --> H[Clinical response at 48-72 hours]:::outcome ``` **Warning:** Do NOT use carbapenems in confirmed MBL-producing organisms—they will fail. Ertapenem is also a carbapenem and will not work. ## Why Repeat Blood Cultures? **Key Point:** Repeat blood cultures after antibiotic initiation help confirm source control and guide duration of therapy. In catheter-associated infections, catheter removal is mandatory for cure. [cite:Harrison 21e Ch 297; Mandell, Douglas & Bennett 9e Ch 220] 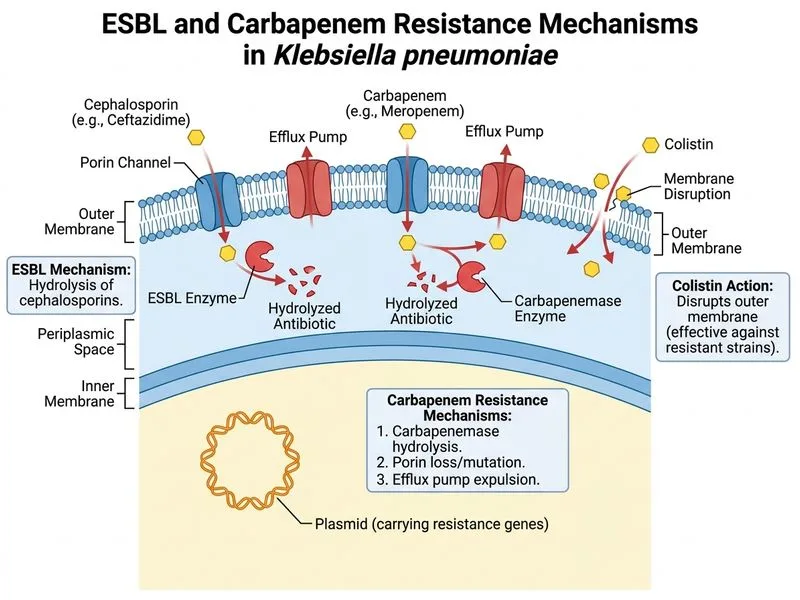
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.