## Clinical Scenario Analysis This patient presents with **healthcare-associated pneumonia (HCAP)** following recent hospitalization and beta-lactam (ceftriaxone) exposure. The resistance pattern is highly specific and points to a well-defined resistance mechanism. ## Resistance Pattern Interpretation **Key Point:** The organism is resistant to ceftriaxone, cefotaxime, ceftazidime, and piperacillin-tazobactam, yet remains **susceptible to carbapenems and colistin**. Clavulanic acid does **NOT** inhibit the beta-lactamase. ### Critical Discriminator Table | Feature | ESBL (classic) | ESBL + reduced OMP permeability | AmpC | KPC/OXA | MBL (IMP/VIM/NDM) | |---------|---------------|-------------------------------|------|---------|-------------------| | **Cephalosporin resistance** | Yes | Yes | Yes | Yes | Yes | | **Pip-tazo resistance** | Variable | Yes | Yes | Yes | Yes | | **Carbapenem susceptibility** | Susceptible | Susceptible | Susceptible | **Resistant** | **Resistant** | | **Clavulanic acid reversal** | Yes | **No** | No | No | No | **High-Yield:** Classic ESBLs are inhibited by clavulanic acid. However, when an ESBL-producing organism **also has reduced outer membrane permeability** (loss of porins such as OmpF/OmpC), clavulanic acid cannot adequately penetrate to inhibit the enzyme — resulting in a phenotype where clavulanic acid does NOT reverse resistance. This explains the non-inhibition by clavulanic acid in this case while carbapenems (which penetrate via different porins and are more stable) remain active. ## Why NOT Metallo-Beta-Lactamase (MBL)? **Critical Fact (Mandell 9e, Murray's Medical Microbiology 9e):** IMP-type, VIM-type, and NDM-type MBLs are zinc-dependent enzymes that hydrolyze **all beta-lactams INCLUDING carbapenems**. They confer carbapenem **resistance**, not susceptibility. An organism producing a clinically significant MBL would be expected to be carbapenem-resistant. Therefore, option D (MBL with carbapenem susceptibility) is factually incorrect — MBLs do not spare carbapenems in clinical practice. ## Why NOT KPC or OXA-type Carbapenemase? Options A and C both imply carbapenem resistance, which contradicts the susceptibility data in the stem. These are ruled out directly. ## Correct Mechanism: ESBL + Reduced Outer Membrane Permeability 1. **ESBL** (e.g., CTX-M, TEM, SHV extended-spectrum variants) hydrolyzes penicillins and extended-spectrum cephalosporins. 2. **Reduced OMP permeability** (porin loss) prevents clavulanic acid from reaching the enzyme in sufficient concentration → clavulanic acid inhibition test is negative. 3. **Piperacillin-tazobactam resistance** occurs because tazobactam (like clavulanic acid) cannot penetrate adequately. 4. **Carbapenems remain active** because they use alternative uptake pathways and are intrinsically more stable against hydrolysis by ESBLs. 5. **Colistin susceptibility** is consistent with a gram-negative rod without colistin resistance mechanisms. **Clinical Pearl:** Loss of outer membrane porins combined with ESBL production is a well-recognized mechanism that mimics carbapenem resistance phenotypically in some assays but retains true carbapenem susceptibility — a key distinction tested in NEET PG/INI-CET. ## Treatment Implications **High-Yield:** For this patient with HCAP due to ESBL + reduced permeability organism: - **First-line:** Carbapenem (meropenem or imipenem-cilastatin) — drug of choice - **Alternative:** Colistin for pan-resistant cases - **Avoid:** All cephalosporins, piperacillin-tazobactam (unreliable even if in vitro susceptibility shown) [cite: Mandell, Douglas & Bennett's Principles and Practice of Infectious Diseases, 9e, Ch 18; Murray's Medical Microbiology, 9e, Ch 15] 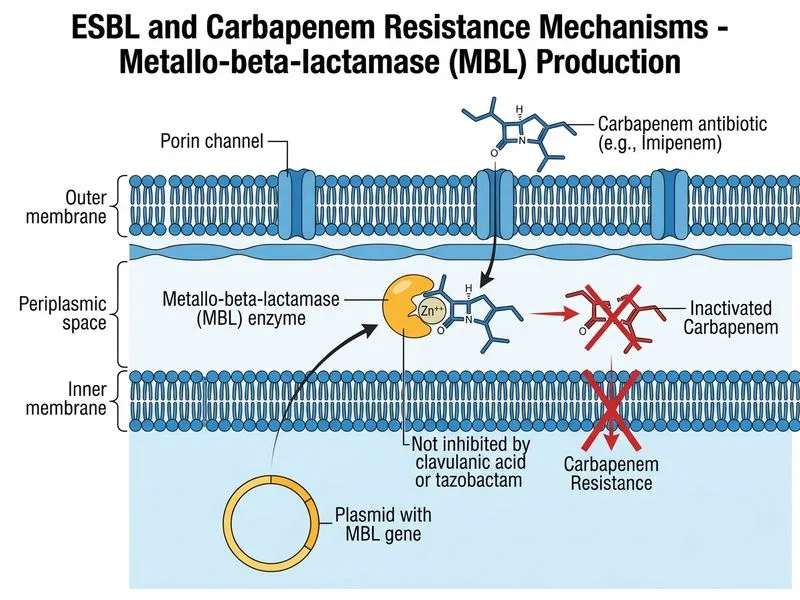
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.