## Clinical Context This case illustrates **acquired carbapenem resistance in an ESBL-producing *Klebsiella pneumoniae*** that was initially susceptible to carbapenems but developed resistance during or shortly after therapy — a phenomenon distinct from primary MBL-mediated resistance and more consistent with **porin loss and efflux pump upregulation**. ## Mechanism: Porin Loss + Efflux Upregulation in *Klebsiella* **Key Point:** In *Klebsiella pneumoniae*, carbapenem resistance frequently arises through a **two-hit mechanism**: loss of outer membrane porins (OmpK35/OmpK36) combined with upregulation of the AcrAB-TolC efflux pump. This is distinct from MBL-mediated resistance and is particularly common in nosocomial strains. ### Why This Mechanism Fits the Clinical Picture 1. **Gradual MIC elevation**: The MIC rose from 0.5 µg/mL (susceptible) to 4 µg/mL (resistant) — consistent with **incremental loss of permeability** rather than enzymatic hydrolysis. 2. **Selective pressure**: Prolonged imipenem exposure selects for mutants with reduced porin expression and increased efflux. 3. **Preserved susceptibility to colistin/tigecycline**: These agents are less dependent on porin-mediated entry and are not substrates for AcrAB, explaining why the organism remains susceptible. 4. **Nosocomial acquisition**: Porin-loss mutants are common in hospital-acquired *Klebsiella* and can emerge during therapy [cite:Mandell, Douglas, and Bennett's Ch 214]. ### Porin Loss Mechanism in *Klebsiella* ```mermaid flowchart TD A[ESBL-producing K. pneumoniae<br/>Imipenem MIC 0.5 µg/mL]:::outcome A --> B[Prolonged imipenem exposure]:::action B --> C{Selective pressure}:::decision C -->|Spontaneous mutation| D[OmpK35/OmpK36 downregulation<br/>or deletion]:::action C -->|Concurrent event| E[AcrAB efflux pump<br/>upregulation]:::action D --> F[Reduced carbapenem entry]:::action E --> F F --> G[Imipenem MIC 4 µg/mL<br/>Carbapenem-resistant]:::outcome G --> H[Colistin/Tigecycline<br/>still active]:::outcome ``` ### Why NOT the Other Options? | Mechanism | Why Incorrect | |-----------|---------------| | **MBL acquisition (NDM-1/VIM)** | Would cause resistance to ALL β-lactams including aztreonam; this patient's aztreonam susceptibility is not mentioned as lost. MBL-mediated resistance typically presents with higher MICs (≥8 µg/mL) and is less common in *Klebsiella* than porin loss. | | **Chromosomal AmpC induction + permeability loss** | AmpC β-lactamases do NOT hydrolyze carbapenems; induction of AmpC would not explain carbapenem resistance. AmpC is more relevant in *Enterobacter*, *Citrobacter*, and *Serratia*. | | **23S rRNA mutation** | Mutations in 23S rRNA confer macrolide resistance (e.g., in *Streptococcus*), not carbapenem resistance. This mechanism is irrelevant to β-lactam resistance. | ## High-Yield: Differential Diagnosis of Carbapenem Resistance Mechanisms | Mechanism | Organism | MIC Pattern | Colistin | Aztreonam | Clinical Clue | |-----------|----------|-------------|----------|-----------|---------------| | **Porin loss + efflux** | *Klebsiella*, *Enterobacter* | Gradual rise (0.5→4) | Susceptible | Susceptible | Emerges during therapy; preserved susceptibility to polymyxins | | **MBL (NDM-1, VIM, IMP)** | *E. coli*, *Klebsiella*, *Pseudomonas* | High (≥8) | Susceptible | **Resistant** | Rapid emergence; aztreonam resistance; EDTA synergy positive | | **OXA carbapenemase** | *Acinetobacter* | Variable | Often resistant | Susceptible | Intrinsic to *Acinetobacter*; colistin often lost | | **KPC serine carbapenemase** | *Klebsiella*, *Enterobacter* | High (≥4) | Susceptible | Susceptible | Plasmid-mediated; inhibited by β-lactamase inhibitors | ## Clinical Pearl **Warning:** Do NOT confuse **porin-loss resistance** (gradual, selective pressure-driven, preserved polymyxin susceptibility) with **MBL-mediated resistance** (rapid, enzymatic, aztreonam-resistant). The former is managed with colistin or tigecycline; the latter requires urgent infection control and source control. ## Management Implications 1. **Switch therapy**: Colistin or tigecycline (organism remains susceptible). 2. **Source control**: Repeat imaging to rule out pneumonia recurrence or new focus. 3. **Infection control**: Contact precautions; screen for other resistant isolates. 4. **Avoid prolonged monotherapy**: Reduces risk of resistance emergence. 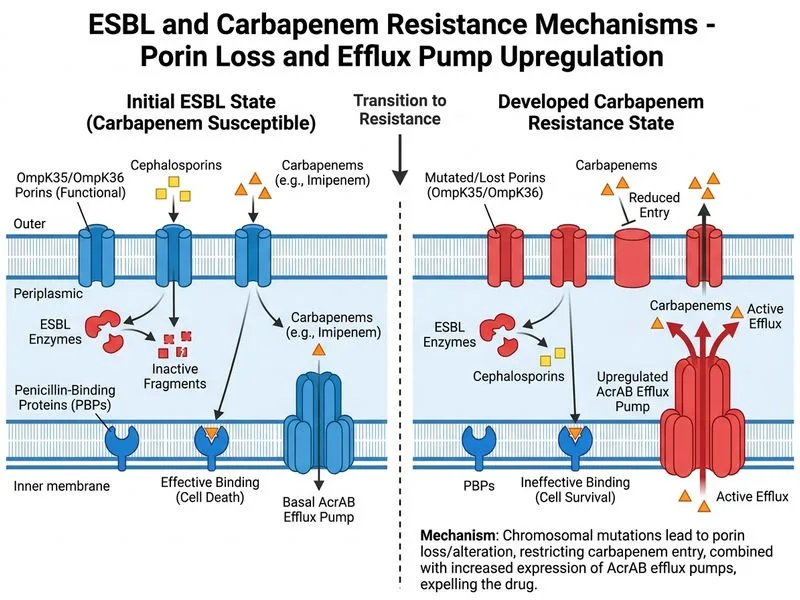
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.