## Clinical Diagnosis: Ewing Sarcoma ### Key Diagnostic Features **Key Point:** Ewing sarcoma is the second most common primary malignant bone tumor in children and adolescents, with peak incidence in the second decade of life (10–20 years). ### Classic Presentation | Feature | Ewing Sarcoma | Osteosarcoma | Osteomyelitis | |---------|---------------|--------------|---------------| | **Age** | 10–20 years | 10–20 years (around growth plate) | Any age | | **Location** | Diaphysis/diametaphysis | Metaphysis | Variable | | **Pain** | Progressive, often nocturnal | Acute onset | Acute with systemic signs | | **Constitutional symptoms** | Fever, malaise common | Rare | Prominent (high fever) | | **Radiographic pattern** | Mixed lytic/sclerotic, sunburst, onion-skin periostitis | Sunburst, Codman triangle | Ill-defined lytic lesion | | **Soft tissue mass** | Present | Present | Minimal | | **ESR/CRP** | Elevated (not diagnostic) | Mildly elevated | Very high | ### Why This Case Points to Ewing Sarcoma 1. **Age and location:** 14-year-old with diaphyseal (mid-shaft femur) involvement — classic for Ewing sarcoma; osteosarcoma favors metaphysis. 2. **Radiographic pattern:** Mixed lytic/sclerotic with sunburst periosteal reaction and onion-skin appearance is pathognomonic for Ewing sarcoma. 3. **Systemic features:** Low-grade fever and malaise are typical constitutional symptoms of Ewing sarcoma, not osteosarcoma. 4. **MRI findings:** Marrow involvement and soft tissue extension are hallmark features. **Clinical Pearl:** Ewing sarcoma often masquerades as infection (fever, elevated inflammatory markers, pain, swelling) — this is a common diagnostic trap. However, the diaphyseal location and imaging pattern distinguish it from osteomyelitis. ### Pathology & Genetics **High-Yield:** Ewing sarcoma is characterized by the **t(11;22)(q24;q12) translocation**, resulting in the **EWSR1-FLI1 fusion gene** — this is the molecular hallmark and is present in ~90% of cases. The tumor is composed of small, round, blue cells with high mitotic activity. **Mnemonic: EWING** — **E**ndothelial (small round cells), **W**hite (pale cytoplasm), **I**nvasive (diaphyseal), **N**ecrosis (common), **G**enetic translocation t(11;22). ### Diagnostic Workup 1. **Plain radiographs:** Sunburst periostitis, onion-skin pattern, mixed lytic/sclerotic lesion in diaphysis. 2. **MRI:** Best for assessing marrow and soft tissue involvement; essential for surgical planning. 3. **CT chest:** Mandatory to exclude pulmonary metastases (present in ~20% at diagnosis). 4. **Biopsy:** Confirms diagnosis; small round cells with high nuclear-to-cytoplasmic ratio. 5. **Molecular testing:** EWSR1-FLI1 fusion (RT-PCR or FISH) — prognostic and therapeutic significance. ### Management & Prognosis - **Neoadjuvant chemotherapy** (vincristine, doxorubicin, cyclophosphamide ± ifosfamide) followed by **surgery** (wide local excision or amputation) and **adjuvant chemotherapy**. - **5-year survival:** ~70% with localized disease; <30% with metastatic disease. - Presence of metastases, large tumor size, and poor chemotherapy response are adverse prognostic factors. **Warning:** Do not confuse Ewing sarcoma with osteosarcoma — osteosarcoma typically arises in the metaphysis, has a more acute presentation, and lacks the systemic symptoms seen here. 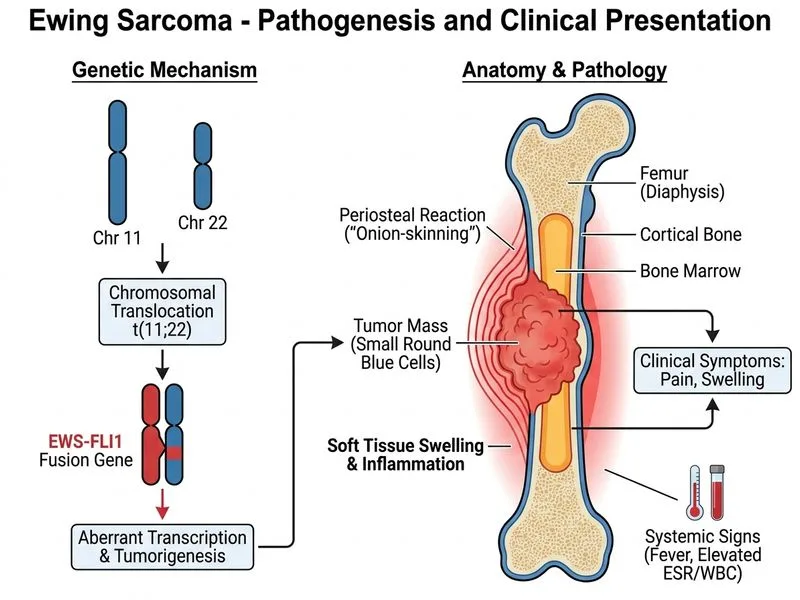
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.