## Patent Ductus Arteriosus (PDA) and Hemodynamic Consequences ### Anatomy of the Ductus Arteriosus The ductus arteriosus is a muscular vessel that connects the **pulmonary artery to the descending aorta** in fetal life. It normally closes functionally within 24–48 hours after birth due to: - Increased oxygen tension (triggers smooth muscle contraction) - Decreased prostaglandin E~2~ (PGE~2~) levels - Mechanical stress from increased blood pressure **Key Point:** In a patent ductus arteriosus (PDA), blood shunts **left-to-right** from the aorta (high pressure) to the pulmonary artery (low pressure), not right-to-left. ### Hemodynamic Effects of Left-to-Right PDA Shunt #### 1. **Increased Aortic Flow** - The aorta must supply both systemic circulation AND the shunted blood returning via the pulmonary circulation - This increases **stroke volume** and **cardiac output** - Results in **elevated systolic pressure** #### 2. **Reduced Diastolic Pressure** - Blood is diverted away from the aorta during diastole (into the low-resistance pulmonary bed) - This causes **diastolic "run-off"** — a drop in aortic diastolic pressure - Results in **reduced diastolic pressure** #### 3. **Wide Pulse Pressure** $$\text{Pulse Pressure} = \text{Systolic} - \text{Diastolic} = 95 - 40 = 55 \text{ mmHg}$$ Normal neonatal pulse pressure is ~30–40 mmHg; this neonate's 55 mmHg is markedly widened. **High-Yield:** Bounding pulses (water-hammer pulse) + wide pulse pressure = classic sign of PDA with left-to-right shunt. ### Clinical Features of PDA | Feature | Mechanism | |---------|----------| | Continuous 'machinery' murmur | Turbulent flow throughout systole and diastole (shunt is continuous) | | Bounding pulses | Increased stroke volume and pulse pressure | | Wide pulse pressure | Systolic elevation + diastolic run-off | | Pulmonary plethora on CXR | Increased pulmonary blood flow from left-to-right shunt | | Mild cyanosis improving with O₂ | Mixing at pulmonary level; not pure right-to-left shunt | | Hyperactive precordium | Increased cardiac output | **Clinical Pearl:** The cyanosis in PDA is mild and improves with oxygen because the shunt is predominantly left-to-right (not right-to-left). Deoxygenated blood is not being bypassed to the systemic circulation in large amounts. ### Why This Is Not a Right-to-Left Shunt In a **right-to-left shunt** (e.g., tetralogy of Fallot, severe PPHN): - Deoxygenated blood bypasses the lungs - Cyanosis is **severe and does NOT improve with oxygen** - Pulse pressure would be **narrow**, not wide - No bounding pulses This neonate's mild cyanosis that improves with O₂ and bounding pulses confirm a **left-to-right shunt**. ### Mermaid: Hemodynamic Flow in PDA ```mermaid flowchart TD A[Aorta<br/>High Pressure] -->|Systole + Diastole| B[PDA Shunt] B --> C[Pulmonary Artery<br/>Low Pressure] C --> D[Lungs] D --> E[Pulmonary Veins] E --> F[Left Atrium] F --> G[Left Ventricle] G --> A A -->|Systemic<br/>Circulation| H[Systemic Organs] H --> I[Systemic Veins] I --> J[Right Atrium] J --> K[Right Ventricle] K --> C style A fill:#ffcccc style C fill:#ccccff style B fill:#ffff99 ``` **Key Point:** The shunt is **left-to-right** (aorta → pulmonary artery). Blood flows from high pressure to low pressure. This causes aortic run-off in diastole, widening the pulse pressure. 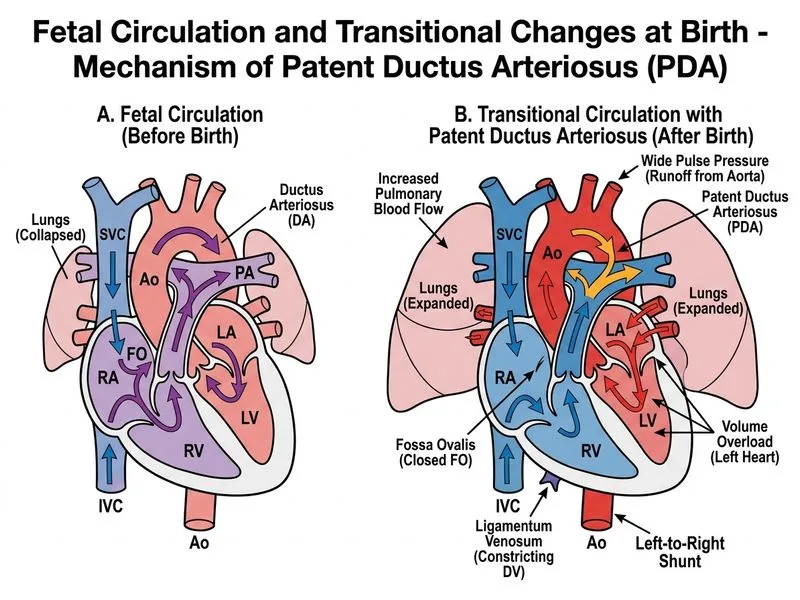
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.