## Diagnosis: Persistent Gestational Trophoblastic Neoplasia (GTN) with Pulmonary Metastases ### Clinical Context: GTN Cascade Persistent GTN (also called postmolar GTN) is the **malignant evolution of trophoblastic tissue following molar pregnancy** that fails to regress despite evacuation. This patient's history of molar pregnancy 6 months ago with **lack of β-hCG surveillance** is the critical risk factor. **Key Point:** GTN can arise from: 1. **Postmolar GTN** (most common, 50% of cases) — after complete or partial mole 2. **Nonmolar GTN** — after normal pregnancy, abortion, or ectopic pregnancy 3. **Choriocarcinoma** — highly malignant form ### Why This Is Persistent GTN | Feature | Finding | Significance | |---------|---------|---------------| | **Prior molar pregnancy** | 6 months ago | Establishes trophoblastic origin | | **Persistent β-hCG** | 8,500 mIU/mL (detectable) | Indicates active trophoblastic disease; should be undetectable 6 months post-evacuation | | **Uterine mass with abnormal vascularity** | Heterogeneous fundal mass | Represents invasive/metastatic trophoblastic tissue | | **Pulmonary nodules** | Multiple, bilateral | Metastatic disease (lungs are most common site for GTN metastases) | | **Hemoptysis** | Present | Due to pulmonary nodule erosion into airways | **High-Yield:** The **combination of prior molar pregnancy + persistent/rising β-hCG + metastatic disease** is diagnostic of GTN. This is a medical oncologic emergency requiring immediate chemotherapy (typically methotrexate or combination regimens based on FIGO risk scoring). ### FIGO Risk Scoring for GTN This patient would be classified as **HIGH-RISK GTN** based on: - Interval >4 months from antecedent event (6 months) - Pulmonary metastases - β-hCG >1,000 mIU/mL High-risk patients require multi-agent chemotherapy (EMA-CO: Etoposide, Methotrexate, Actinomycin D, Cyclophosphamide, Vincristine). ### Pathophysiology of Metastatic GTN ```mermaid flowchart TD A[Molar pregnancy evacuation]:::outcome --> B[Trophoblastic tissue remains in uterus]:::outcome B --> C{β-hCG surveillance?}:::decision C -->|Yes, monitored| D[Regression to undetectable]:::action C -->|No, unmonitored| E[Persistent/rising β-hCG]:::urgent E --> F[Invasive mole or choriocarcinoma]:::urgent F --> G[Local myometrial invasion]:::urgent G --> H[Hematogenous spread to lungs, brain, liver]:::urgent H --> I[Metastatic GTN]:::urgent I --> J[Hemoptysis, neurologic symptoms, hepatic dysfunction]:::urgent ``` **Clinical Pearl:** The **absence of β-hCG follow-up** is the critical missed opportunity. All patients with molar pregnancy must have: - Weekly β-hCG until undetectable - Monthly β-hCG for 6–12 months - Chest X-ray before and after evacuation - Pelvic ultrasound during follow-up ### Differential Diagnosis | Diagnosis | β-hCG | Uterine Mass | Prior Mole | Pulmonary Findings | |-----------|-------|--------------|-----------|-------------------| | **Persistent GTN** | Persistent/rising | Yes (invasive) | Yes | Metastatic nodules | | **Recurrent molar pregnancy** | Would be very high if present | Molar pattern | Yes (prior) | None | | **Leiomyosarcoma** | Negative | Yes | No | Metastases possible but β-hCG negative | | **TB** | Negative | No | No | Cavitary/infiltrative pattern | ### Management 1. **Immediate chemotherapy** (EMA-CO for high-risk disease) 2. **Serial β-hCG monitoring** during and after treatment 3. **Imaging surveillance** (chest X-ray, CT abdomen/pelvis, brain MRI if CNS symptoms) 4. **Contraception** during treatment (teratogenic agents) 5. **Avoid pregnancy** for 12 months post-treatment 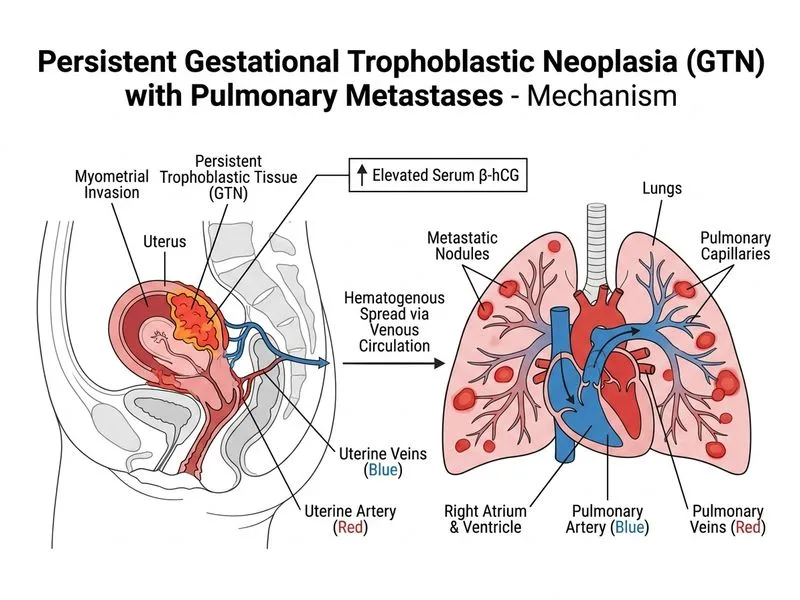
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.