## Diagnosis and Staging of Gestational Trophoblastic Disease **Key Point:** In suspected molar pregnancy or persistent gestational trophoblastic disease (GTD), the combination of imaging and metastatic workup is essential before treatment initiation. ### Role of Chest X-ray and Abdominal CT Chest X-ray is the first-line imaging to detect pulmonary metastases, which occur in 4–8% of complete molar pregnancies and up to 20% of invasive moles. Abdominal/pelvic CT with contrast provides: - Assessment of uterine invasion (invasive mole vs. choriocarcinoma) - Detection of hepatic and abdominal metastases - Baseline staging for risk stratification **High-Yield:** The WHO scoring system for GTD risk stratification requires imaging confirmation of metastatic disease. Chest X-ray is mandatory; CT is added if chest X-ray is abnormal or if clinical suspicion of invasive disease is high. ### Why This Combination? 1. **Ultrasound** (already done) confirms the diagnosis via the characteristic "bunch of grapes" appearance and absence of fetal parts. 2. **β-hCG level** (already measured) guides risk stratification but does not localize disease. 3. **Imaging** (chest X-ray + CT) is required to: - Detect occult metastases - Assess depth of myometrial invasion - Determine FIGO score and treatment intensity **Clinical Pearl:** A markedly elevated β-hCG (>100,000 mIU/mL) increases risk of metastatic disease and warrants aggressive imaging workup before chemotherapy. ### Investigation Algorithm ```mermaid flowchart TD A[Suspected GTD on ultrasound]:::outcome --> B[Measure serum β-hCG]:::action B --> C{β-hCG level & clinical features}:::decision C -->|Low risk| D[Chest X-ray]:::action C -->|High risk or elevated hCG| E[Chest X-ray + CT abdomen/pelvis]:::action D --> F[Assess for metastases]:::outcome E --> F F --> G[Risk stratification & treatment planning]:::action ``` [cite:FIGO GTD Handbook; Park 26e Ch 15] 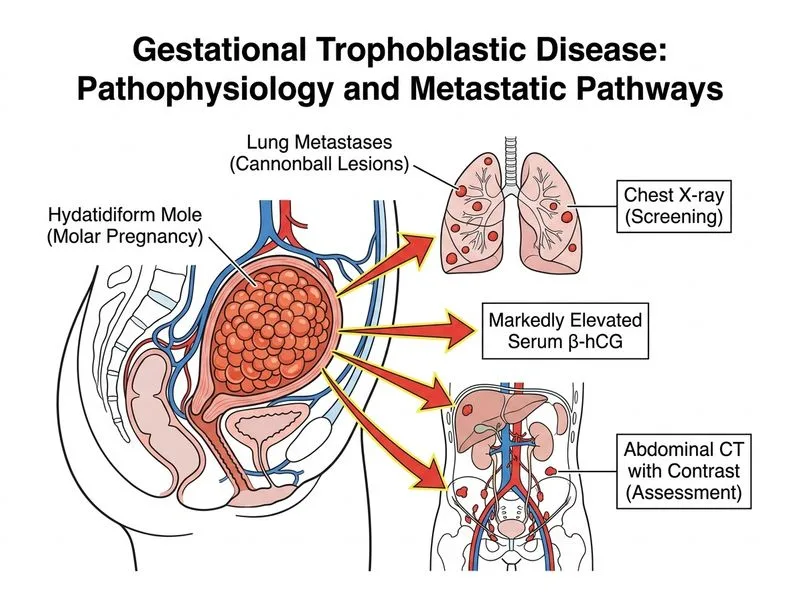
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.