## Clinical Diagnosis: Persistent GTN **Key Point:** The β-hCG plateau (not declining to undetectable) after evacuation of molar pregnancy defines **persistent gestational trophoblastic neoplasia (GTN)**. This is a malignant condition requiring chemotherapy. ## β-hCG Kinetics and Diagnosis | Finding | Interpretation | |---------|----------------| | β-hCG declines to undetectable by 8–12 weeks post-evacuation | Complete remission; no GTN | | β-hCG plateau or rises after initial decline | **Persistent GTN** | | β-hCG never declines adequately | Persistent GTN | | Detectable β-hCG >6 months post-evacuation | Persistent GTN | **High-Yield:** In this case, β-hCG declined initially (Week 1 → Week 3) but then plateaued (Week 5 = 22,000; Week 8 = 19,000). This plateau pattern is diagnostic of persistent GTN, not retained molar tissue (which would show continued high β-hCG without decline). ## Differential Diagnosis: Invasive Mole vs. Persistent GTN ```mermaid flowchart TD A[Persistent GTN After Molar Evacuation]:::outcome --> B{Uterine Invasion on Imaging?}:::decision B -->|Yes, Confined to Uterus| C[Invasive Mole]:::outcome B -->|No Invasion, or Extrauterine Disease| D[Choriocarcinoma/Other GTN]:::outcome C --> E[Chemotherapy First-Line]:::action D --> F[Chemotherapy First-Line]:::action E --> G[Hysterectomy if Chemotherapy Fails]:::action F --> G ``` **Clinical Pearl:** The distinction between invasive mole and choriocarcinoma is histological, not clinical. Both are treated with chemotherapy first. Hysterectomy is reserved for chemotherapy-resistant disease or life-threatening haemorrhage. ## Why This Is Persistent GTN, Not Retained Molar Tissue **Key Point:** Retained molar tissue typically presents with: - Continued high β-hCG (>50,000 mIU/mL) without decline - Uterine bleeding within 2–3 weeks of evacuation - Large intrauterine mass - Management: repeat evacuation In this patient, β-hCG **declined initially** (120,000 → 45,000 → 18,000), then **plateaued**. This pattern indicates trophoblastic tissue has invaded the myometrium or metastasized—not simple retained molar tissue. ## Management of Persistent GTN **High-Yield:** All persistent GTN requires chemotherapy, regardless of whether it is invasive mole or choriocarcinoma. First-line regimens: 1. **Low-risk GTN** (β-hCG <40,000, no metastases, <4 months since evacuation): - Methotrexate 1 mg/kg IM weekly + folinic acid rescue - OR 5-FU 15 mg/kg IV weekly - Single-agent cure rate >90% 2. **High-risk GTN** (β-hCG >40,000 or metastases or >4 months since evacuation): - EMA-CO (etoposide, methotrexate, actinomycin D, cyclophosphamide, vincristine) - Cure rate >85–90% **This patient is low-risk** (β-hCG ~20,000, no metastases, 8 weeks post-evacuation). Methotrexate monotherapy is appropriate. ## Why Hysterectomy Is Not First-Line **Warning:** Hysterectomy should NOT be performed as primary treatment because: - Chemotherapy cures >90% of persistent GTN - Hysterectomy does not eliminate metastatic disease - Patient may wish to preserve fertility - Hysterectomy is reserved for chemotherapy failure or life-threatening bleeding 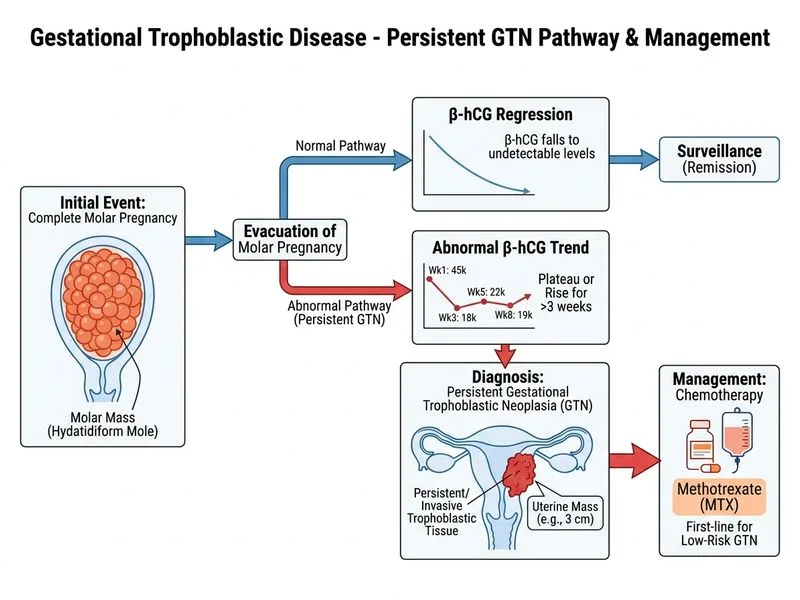
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.