## Antecedent Infections in GBS **Key Point:** Campylobacter jejuni is the most frequently identified antecedent infection in GBS globally, including in India, preceding symptom onset by 1–3 weeks in 20–40% of cases. ### Geographic and Epidemiological Patterns | Antecedent Agent | Global Frequency | India/Asia Frequency | Mechanism | |------------------|------------------|----------------------|----------| | **Campylobacter jejuni** | 20–40% | Most common | Molecular mimicry (LPS epitopes) | | **Cytomegalovirus** | 5–10% | Less common | Reactivation in immunocompromised | | **Zika virus** | Emerging (2016+) | Regional outbreaks | Neurotropism, immune activation | | **Mycoplasma pneumoniae** | 5–10% | Variable | Cross-reactive antibodies | | **No identified trigger** | 30–50% | 30–50% | Idiopathic | **High-Yield:** Campylobacter jejuni causes acute gastroenteritis with diarrhea 1–3 weeks before GBS onset. The bacterial lipopolysaccharide (LPS) shares epitopes with gangliosides on peripheral nerve myelin, triggering cross-reactive antibodies (anti-GM1, anti-GQ1b) that attack the nerve sheath — a mechanism called **molecular mimicry**. ### Molecular Mimicry Mechanism 1. Campylobacter infection → intestinal inflammation 2. Bacterial LPS epitopes cross-react with nerve gangliosides 3. Humoral and cellular immune response against myelin 4. Demyelination and axonal injury 5. Ascending paralysis (1–3 weeks post-infection) **Mnemonic:** **C-GBS** = **C**ampylobacter is the **C**ommonest culprit in GBS. **Clinical Pearl:** A history of diarrhea 2–4 weeks before paralysis onset should raise suspicion for GBS with Campylobacter antecedent. Serological testing for anti-Campylobacter antibodies and anti-ganglioside antibodies (anti-GM1, anti-GQ1b) can support the diagnosis. [cite:Harrison 21e Ch 379] 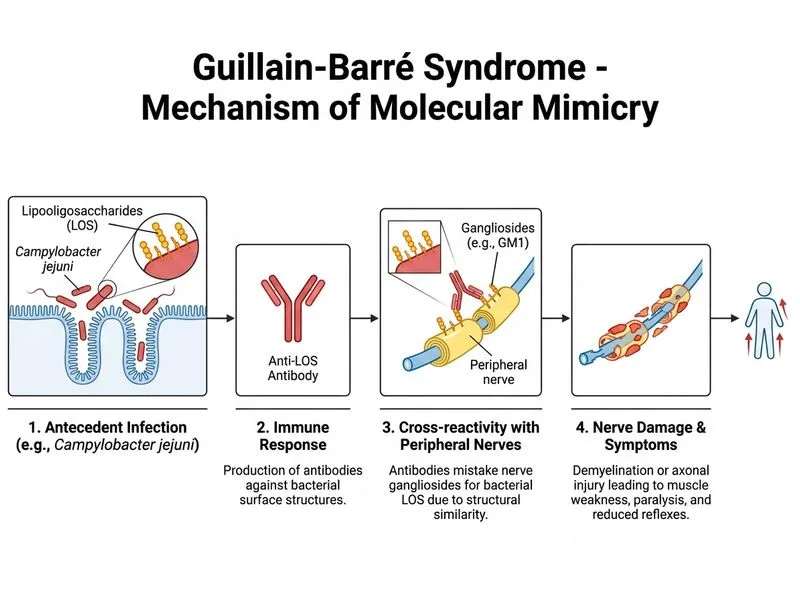
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.