## Diagnosis: Guillain-Barré Syndrome (GBS) ### Clinical Presentation **Key Point:** Ascending paralysis starting distally in the lower limbs and progressing proximally over days to weeks is the hallmark of GBS. - Progressive weakness involving lower limbs first, then upper limbs and bulbar muscles - Antecedent infection (diarrhea 2 weeks prior) — common trigger - Rapid onset and progression (5 days in this case) - Preserved sensation and cognition ### Diagnostic Criteria Met | Feature | Finding | Significance | |---------|---------|---------------| | **Motor weakness** | Ascending, bilateral, symmetric | Classic GBS pattern | | **Areflexia/hyporeflexia** | Diminished DTRs | Hallmark neurological sign | | **CSF findings** | High protein, normal cells | Albuminocytologic dissociation | | **NCS abnormalities** | Conduction blocks, prolonged latencies | Demyelinating variant (AIDP) | | **Antecedent illness** | Diarrhea 2 weeks prior | Campylobacter jejuni common trigger | **High-Yield:** The combination of **ascending paralysis + areflexia + albuminocytologic dissociation + demyelinating NCS changes** is pathognomonic for GBS. ### Pathophysiology ```mermaid flowchart TD A[Antecedent infection<br/>Campylobacter jejuni<br/>Viral illness]:::outcome --> B[Molecular mimicry<br/>Cross-reactive antibodies]:::outcome B --> C[Antibody-mediated attack<br/>on myelin sheath]:::outcome C --> D[Demyelination of<br/>peripheral nerves]:::outcome D --> E[Conduction blocks<br/>Slowed conduction]:::outcome E --> F[Progressive ascending<br/>paralysis]:::outcome F --> G[Peak disability at<br/>2-4 weeks]:::outcome ``` ### Variants of GBS | Variant | NCS Pattern | Frequency | Geography | |---------|------------|-----------|----------| | **AIDP** (Acute Inflammatory Demyelinating Polyneuropathy) | Demyelinating (conduction blocks, prolonged latencies) | 80% (Western countries) | Common worldwide | | **AMAN** (Acute Motor Axonal Neuropathy) | Axonal (normal latencies, reduced amplitudes) | 30–50% | More common in Asia | | **AMSAN** (Acute Motor-Sensory Axonal Neuropathy) | Axonal with sensory involvement | 5–10% | Variable | | **MFS** (Miller Fisher Syndrome) | Ataxia, ophthalmoplegia, areflexia | 5% | Rare | **Clinical Pearl:** In this patient, the **demyelinating pattern on NCS** (conduction blocks, prolonged distal latencies) indicates AIDP, the most common variant in India and worldwide. ### Why This Is GBS and Not Other Diagnoses **Key Point:** The **albuminocytologic dissociation** (high CSF protein with normal cell count) is virtually diagnostic of GBS and distinguishes it from inflammatory myelitis (which would show pleocytosis). --- ## Management Principles 1. **Respiratory monitoring:** Vital capacity, negative inspiratory force — ~25% require mechanical ventilation 2. **Immunotherapy:** Intravenous immunoglobulin (IVIg) or plasma exchange within 2 weeks of symptom onset 3. **Supportive care:** DVT prophylaxis, pain management, nutritional support 4. **Prognosis:** Most patients recover fully over 3–6 months; ~10% have residual weakness **Mnemonic: GABS** — **G**radual ascending **A**reflexia **B**ilateral **S**ymmetric paralysis 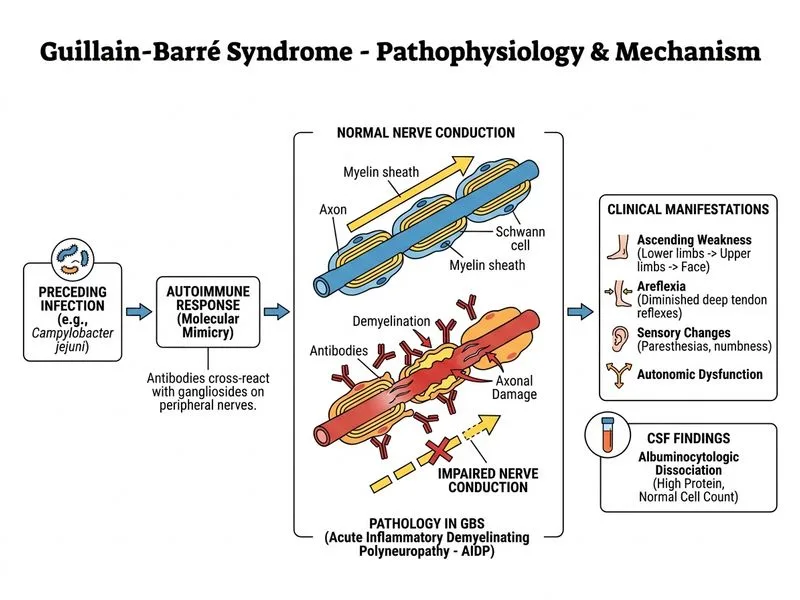
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.