## Diagnostic Uncertainty and Surveillance Strategy **Key Point:** This nodule does NOT meet diagnostic criteria for HCC on current imaging and requires further characterization before treatment initiation. ### AASLD/EASL Diagnostic Criteria for HCC For a nodule 1–2 cm in a cirrhotic liver, HCC diagnosis requires: - **Arterial phase hyperenhancement (APHE)**, AND - **Washout in portal venous or delayed phase** on **at least ONE imaging modality** (CT or MRI) OR - Positive findings on **TWO imaging modalities** **High-Yield:** This patient's nodule shows APHE on CT but **lacks clear washout**. This is insufficient for diagnosis on a single imaging modality. A second imaging study (MRI or repeat CT) is needed to either confirm or exclude HCC. ### Management Algorithm for Nodules 1–2 cm ```mermaid flowchart TD A[Nodule 1-2 cm found on surveillance]:::outcome --> B{APHE on CT/MRI?}:::decision B -->|No| C[Repeat ultrasound in 3-4 months]:::action B -->|Yes| D{Washout on same modality?}:::decision D -->|Yes| E[HCC Diagnosed]:::outcome D -->|No| F[Perform second imaging<br/>modality MRI or repeat CT]:::action E --> G[Stage and treat]:::action F --> H{Washout on 2nd modality?}:::decision H -->|Yes| I[HCC Diagnosed]:::outcome H -->|No| J[Benign nodule or dysplasia<br/>Repeat ultrasound in 3 months]:::action I --> G ``` ### Rationale for Repeat Imaging | Criterion | This Patient | Interpretation | |-----------|---|---| | Nodule size | 1.2 cm | In the 1–2 cm "gray zone" | | APHE on CT | Present | Suspicious but not diagnostic alone | | Washout on CT | Absent or unclear | Does not meet single-modality criteria | | AFP elevation | Mild (45 ng/mL) | Nonspecific; can occur in cirrhosis, hepatitis | | Child-Pugh score | A | Good liver function; can tolerate further imaging | **Clinical Pearl:** Small nodules (1–2 cm) with APHE but no washout often represent dysplastic nodules or early HCC. Repeat imaging in 3 months allows: 1. **Growth assessment** — HCC typically grows; dysplastic nodules grow slowly 2. **Washout development** — early HCC may show washout only on subsequent imaging 3. **Reduced false positives** — avoids unnecessary treatment of benign lesions ### Why MRI is Preferred for Confirmation - **Hepatobiliary contrast agents** (gadoxetate) provide superior characterization of small nodules - **Better tissue characterization** — can detect subtle washout missed on CT - **No additional radiation** — important for repeated surveillance **Mnemonic:** **APHE + Washout = HCC**; **APHE alone (single modality) = Repeat imaging** ## Why Not the Other Options? **Biopsy (Option B)** is not first-line for nodules in the diagnostic gray zone. Biopsy is reserved for: - Nodules that persistently do not meet imaging criteria after repeat imaging - Atypical imaging findings - Immunocompromised patients where infection must be excluded Biopsy carries procedural risk and may miss early HCC due to sampling error. **Sorafenib (Option C)** requires confirmed HCC diagnosis. Initiating systemic therapy on uncertain imaging would expose the patient to unnecessary toxicity (hand-foot skin reaction, diarrhea, hepatotoxicity) if the nodule is benign or dysplastic. **Hepatic resection (Option D)** is not appropriate without confirmed HCC diagnosis. Resection is offered to selected patients with early-stage HCC and preserved liver function, but diagnosis must be certain first. Unnecessary surgery risks morbidity and mortality. [cite:AASLD HCC Guidelines 2023; Harrison 21e Ch 297] 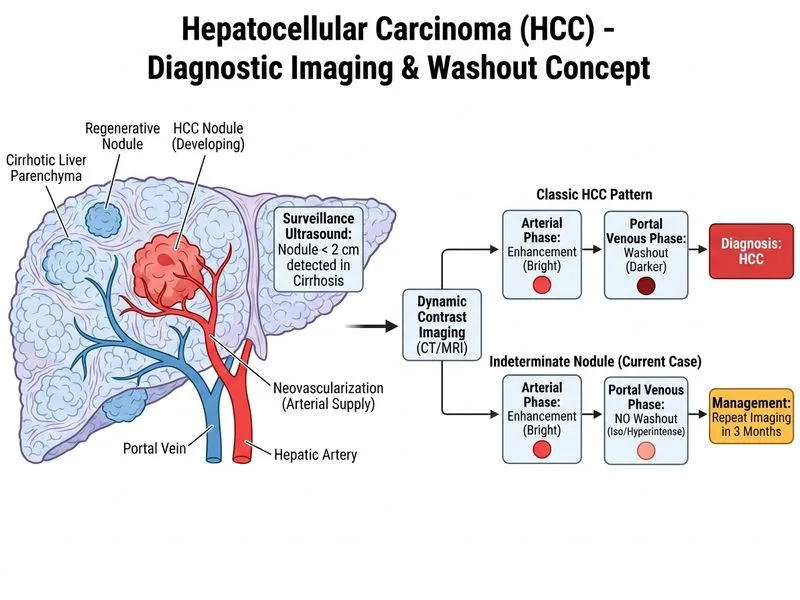
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.