## Imaging Diagnosis of HCC in Cirrhosis **Key Point:** The hallmark imaging criterion for HCC diagnosis in cirrhotic livers is **arterial phase hyperenhancement (APHE) followed by washout** in the portal venous or delayed phase. This pattern reflects the dual blood supply shift in HCC — increased arterial input and loss of portal venous supply. ### Diagnostic Imaging Criteria | Feature | HCC | Benign Nodule | Regenerative Nodule | |---------|-----|---------------|---------------------| | Arterial phase | Hyperenhancement | Isodense/hypoenhance | Isodense | | Portal venous phase | Washout (hypoenhance) | Persistent enhancement | Isodense | | Delayed phase | Washout continues | May persist | Isodense | | Size dependency | Applies to nodules >10 mm | Size-independent | Usually <10 mm | **High-Yield:** The **APHE + washout pattern** is pathognomonic for HCC in a cirrhotic liver and is the basis of non-invasive diagnosis per AASLD and EASL guidelines. A single imaging modality (CT or MRI) showing this pattern in a nodule >10 mm in a cirrhotic patient is diagnostic of HCC — no biopsy needed. **Clinical Pearl:** Benign regenerative nodules in cirrhosis are typically small (<10 mm), isodense to liver on all phases, and do not show arterial enhancement. They represent hepatocyte proliferation in response to liver injury, not neoplastic transformation. **Mnemonic:** **APHE-WO** = Arterial Phase Hyperenhancement with Washout = HCC signature. ### Pathophysiology of the Pattern 1. Early HCC loses normal portal blood supply (portal tracts are destroyed) 2. Tumor develops a rich **hepatic arterial network** (angiogenesis) 3. On arterial phase → tumor "lights up" (hyperenhances) 4. On portal/delayed phases → tumor washes out (lacks portal supply, no sustained enhancement) 5. Benign nodules retain normal dual blood supply → sustained enhancement [cite:Robbins 10e Ch 20] 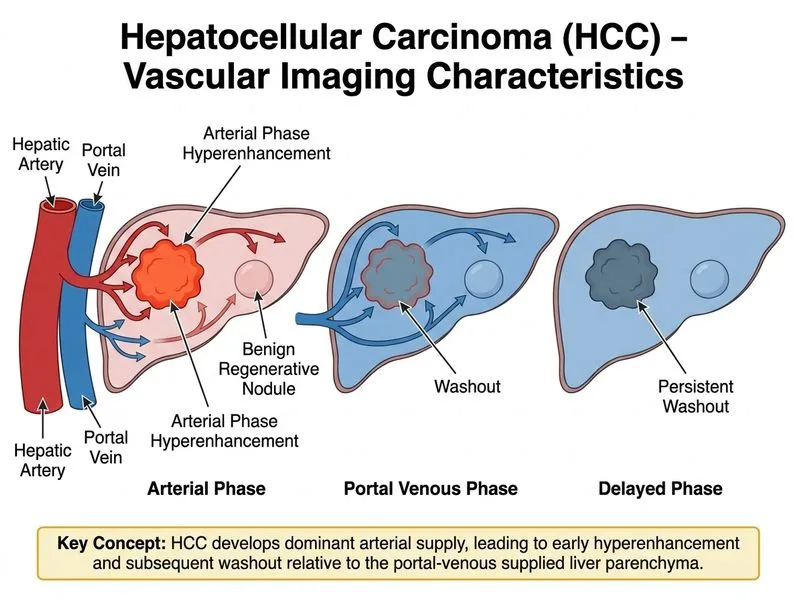
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.