## Management of a Growing Liver Nodule with Atypical Imaging in Cirrhosis ### Clinical Scenario Analysis **Key Point:** This 2.5 cm nodule (growing to 3.2 cm) shows **APHE without washout** — an **atypical/discordant** imaging pattern. While AASLD 2018 guidelines state that APHE alone in a nodule >20 mm in a cirrhotic liver is sufficient for HCC diagnosis, the **absence of washout** is an atypical feature that raises the possibility of a non-HCC lesion (e.g., intrahepatic cholangiocarcinoma, combined HCC-CCA, or high-grade dysplastic nodule). In this setting, **liver biopsy is the most appropriate next step** to confirm histological diagnosis before committing to definitive therapy. ### Diagnostic Criteria Review (AASLD 2018 / LI-RADS) | Criterion | Status | Significance | |-----------|--------|-------------| | **Nodule size** | 2.5 cm → 3.2 cm | >20 mm threshold met | | **APHE** | Present | ✓ Positive | | **Washout** | **Absent** | ✗ Atypical — raises non-HCC differential | | **AFP** | 45 ng/mL | Mildly elevated; non-diagnostic | | **Growth** | +0.7 cm in 3 months | Supports malignancy but not HCC-specific | | **Risk liver** | HCV cirrhosis | ✓ At-risk liver | ### Why Biopsy is the Correct Next Step **High-Yield:** Per AASLD 2018 and EASL guidelines, when imaging features are **discordant** (APHE present but washout absent) in a nodule >20 mm, the pattern is classified as **LI-RADS 4 (probably HCC)** rather than LI-RADS 5 (definitely HCC). In this scenario: 1. **Intrahepatic cholangiocarcinoma (iCCA)** can mimic HCC with arterial enhancement but typically lacks washout — biopsy is essential to distinguish these entities, as management differs fundamentally. 2. **Combined HCC-CCA** also shows atypical enhancement patterns. 3. **Sorafenib or resection** without histological confirmation risks treating the wrong disease. 4. **Nodule growth** (2.5 → 3.2 cm in 3 months) increases urgency — further surveillance delay is inappropriate. **Clinical Pearl (Harrison's Principles, 21st ed.):** Biopsy is indicated when imaging findings are atypical or discordant, particularly when the distinction between HCC and iCCA has direct therapeutic implications. The risk of needle-tract seeding (~2.7%) is acceptable when the diagnosis is uncertain and will change management. ### Why NOT the Other Options? - **A (Hepatic resection):** Requires confirmed HCC diagnosis; premature without histology given atypical imaging. - **B (Sorafenib):** First-line systemic therapy for advanced/unresectable HCC — requires confirmed diagnosis first; inappropriate here. - **D (Repeat CT/MRI in 3–4 months):** Inappropriate given the nodule has already grown significantly over 3 months. Further surveillance delay risks disease progression. This approach would be reasonable only if the nodule were stable and <20 mm. ### Summary Algorithm **APHE + Washout in >20 mm nodule → LI-RADS 5 → Diagnose HCC → Treat** **APHE alone (no washout) in >20 mm nodule → LI-RADS 4 → Atypical → Biopsy for histological confirmation** **Mnemonic: ATYPICAL = Always Take Your Pathology In Cases of Atypical Liver lesions** 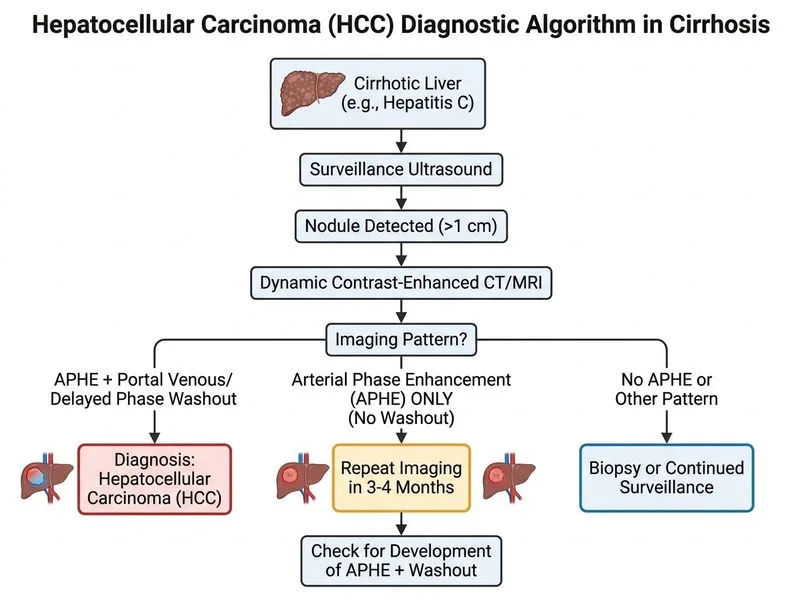
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.