## Management of Crohn Disease with Intra-abdominal Abscess ### Clinical Scenario Analysis **Key Point:** An intra-abdominal abscess in Crohn disease is a surgical emergency if it ruptures, but a contained abscess >3 cm should be drained percutaneously first, reserving surgery for failed medical management or perforation. This patient has: - Transmural Crohn disease (cobblestoning, stricture) - A **contained intra-abdominal collection** (4 × 5 cm) - Signs of sepsis (fever, elevated WCC, elevated CRP) - No evidence of free perforation or peritonitis ### Management Algorithm for Crohn-Related Abscess ```mermaid flowchart TD A[Crohn disease + intra-abdominal collection]:::outcome --> B{Size & containment?}:::decision B -->|Small <3 cm, contained| C[Conservative: antibiotics + medical therapy]:::action B -->|Large ≥3 cm, symptomatic| D[Percutaneous drainage + antibiotics]:::action B -->|Free perforation, peritonitis| E[Emergency surgery]:::urgent D --> F[Reassess after 4-6 weeks]:::decision F -->|Resolved, medically controlled| G[Continue medical therapy, avoid surgery]:::action F -->|Persistent/recurrent| H[Elective surgical resection]:::action C --> G ``` ### Why Percutaneous Drainage Is First-Line | Approach | Indication | Outcome | |----------|-----------|----------| | **Percutaneous drainage** | Abscess ≥3 cm, contained, no free perforation | Allows source control + medical therapy; avoids emergency surgery | | **Surgery (emergency)** | Free perforation, uncontained sepsis, failed drainage | High morbidity; reserved for failed conservative management | | **Surgery (elective)** | Recurrent abscess after drainage, stricture with obstruction | Planned resection after inflammation resolves | **High-Yield:** Percutaneous drainage converts an emergency surgical case into a controlled, medically manageable scenario. This is the **standard of care** for contained abscesses >3 cm in Crohn disease [cite:Harrison 21e Ch 297]. ### Why Each Alternative Is Suboptimal 1. **Immediate surgical resection** — Surgery in the acute inflammatory phase carries high morbidity and mortality. Percutaneous drainage allows inflammation to settle before elective surgery if needed. 2. **High-dose steroids + antibiotics alone** — Without drainage, a 4–5 cm collection will not resolve; continued sepsis risks rupture and peritonitis. Antibiotics alone are insufficient for large abscesses. 3. **Infliximab monotherapy** — Biologic therapy is contraindicated in active sepsis and uncontrolled abscess. Drainage must precede immunosuppression. **Clinical Pearl:** The "step-up" approach in Crohn disease is: (1) percutaneous drainage for source control, (2) antibiotics + medical therapy, (3) elective surgery only if abscess recurs or stricture causes obstruction. This reduces emergency surgery rates from ~50% to <10% [cite:Robbins 10e Ch 17]. ### Post-Drainage Management - **Broad-spectrum antibiotics** (e.g., ciprofloxacin + metronidazole) for 4–6 weeks - **Repeat imaging** at 4–6 weeks to confirm resolution - **Medical therapy escalation** — 5-ASA, corticosteroids, then biologics (infliximab/adalimumab) if not already on them - **Elective resection** only if abscess recurs or stricture persists [cite:Harrison 21e Ch 297] 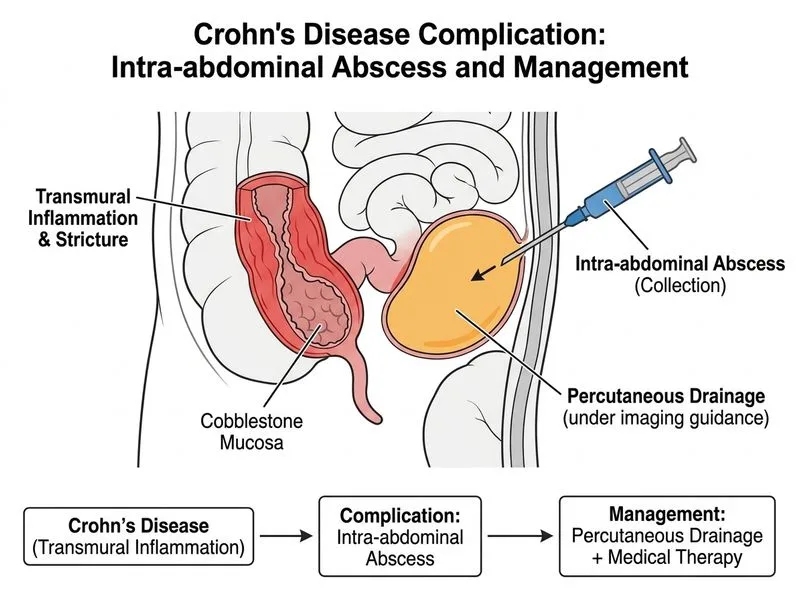
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.