## Diagnosis: Ulcerative Colitis ### Key Distinguishing Features **Key Point:** The clinical and histopathological presentation is pathognomonic for ulcerative colitis (UC): - **Continuous mucosal inflammation** limited to the colon - **Crypt distortion** and increased chronic inflammatory infiltrate in the lamina propria - **Bloody diarrhoea** as the predominant symptom - **Normal albumin** (suggesting preserved nutritional status despite symptoms) ### Pathological Hallmarks of UC | Feature | Ulcerative Colitis | Crohn Disease | |---------|-------------------|---------------| | **Distribution** | Continuous, colon only | Skip lesions, any part of GI tract | | **Depth of inflammation** | Mucosa and submucosa | Transmural | | **Crypt changes** | Crypt distortion, branching | Crypt branching, fissuring | | **Granulomas** | Absent | Present in 30–50% | | **Complications** | Toxic megacolon, perforation | Fistulas, strictures, abscesses | ### Why This Is UC and Not Crohn Disease **High-Yield:** The **continuous pattern of inflammation confined to the colon** is the single most important distinguishing feature. Crohn disease would show: - Skip lesions (areas of normal mucosa between inflamed segments) - Transmural inflammation (not just mucosal) - Granulomas on biopsy (present in ~40% of cases) - Potential involvement of small bowel or upper GI tract ### Clinical Pearl **Clinical Pearl:** UC typically presents with bloody diarrhoea as the cardinal symptom, whereas Crohn disease often presents with abdominal pain and diarrhoea (not necessarily bloody). The absence of systemic fever and preserved albumin favour UC over fulminant disease. ### Diagnostic Criteria for UC 1. Continuous mucosal inflammation starting from rectum 2. Inflammation limited to colon 3. Crypt distortion and chronic inflammatory infiltrate 4. Absence of granulomas 5. Absence of transmural involvement [cite:Robbins 10e Ch 17] 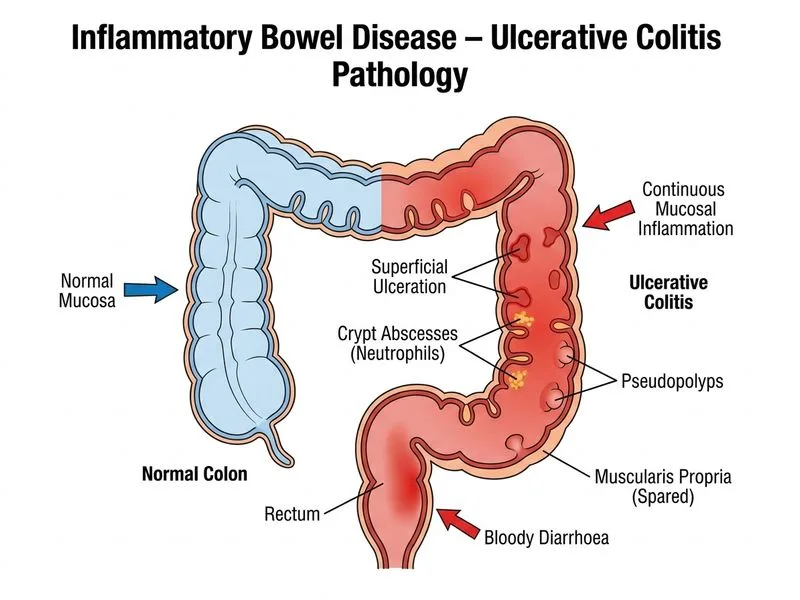
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.