## Management of Perforated Crohn's Disease ### Clinical Diagnosis: Bowel Perforation **Key Point:** Free air under the diaphragm on plain X-ray is pathognomonic for bowel perforation and constitutes a surgical emergency. This patient has: - **Acute peritonitis**: Rigid abdomen, rebound tenderness, absent bowel sounds - **Systemic toxicity**: Fever, tachycardia - **Imaging confirmation**: Free air on plain film - **Underlying IBD**: Crohn's disease with poor disease control (non-compliant with azathioprine) **High-Yield:** Perforation in Crohn's disease is a **surgical emergency** requiring immediate laparotomy — medical management alone is contraindicated. ### Why Emergency Laparotomy Is Correct **Clinical Pearl:** Free air on imaging combined with peritoneal signs mandates immediate surgical intervention. Delay increases morbidity and mortality from sepsis and multi-organ failure. Surgical options in perforated Crohn's disease: 1. **Resection of affected segment** (most common) 2. **Primary anastomosis** (if no significant contamination) 3. **Exteriorization/ileostomy** (if extensive disease or high contamination) 4. **Drainage of localized abscess** (if perforation is contained) ### Why Other Options Are Wrong | Option | Why Incorrect | |--------|---------------| | **High-dose IV steroids + antibiotics alone** | Medical management cannot seal a perforation; delay increases sepsis risk and mortality. Steroids may worsen perforation outcomes. | | **Anti-TNF therapy (infliximab)** | Contraindicated in acute peritonitis and perforation; increases infection risk. Requires surgical control first. | | **CT abdomen with contrast** | Delays definitive treatment in a surgical emergency. Free air on plain film is sufficient for diagnosis; imaging should not postpone surgery. | **Warning:** Corticosteroids in the setting of perforation can mask symptoms and worsen outcomes — they are contraindicated until after surgical repair. ### Pre-operative Resuscitation (Parallel to Surgery) While preparing for theatre: 1. **IV fluid resuscitation**: Aggressive crystalloid bolus 2. **Broad-spectrum antibiotics**: Cover gram-negative, gram-positive, and anaerobes (e.g., piperacillin-tazobactam or cefotaxime + metronidazole) 3. **NPO status**: Nil per mouth 4. **Urinary catheter**: Monitor urine output 5. **Central line**: Consider for hemodynamic monitoring in septic shock **Mnemonic:** SURGICAL = **S**epsis control, **U**rgent resection, **R**esuscitation fluids, **G**ram-negative coverage, **I**V antibiotics, **C**entral access, **A**cute peritonitis, **L**aparotomy, **E**mergency = Perforated IBD management ### Post-operative Management - **Restart IBD therapy** after recovery (5-ASA, azathioprine, or anti-TNF) - **Ensure compliance** to prevent recurrence - **Monitor for anastomotic leak** (fever, tachycardia, elevated WBC in post-op period) [cite:Harrison 21e Ch 295] 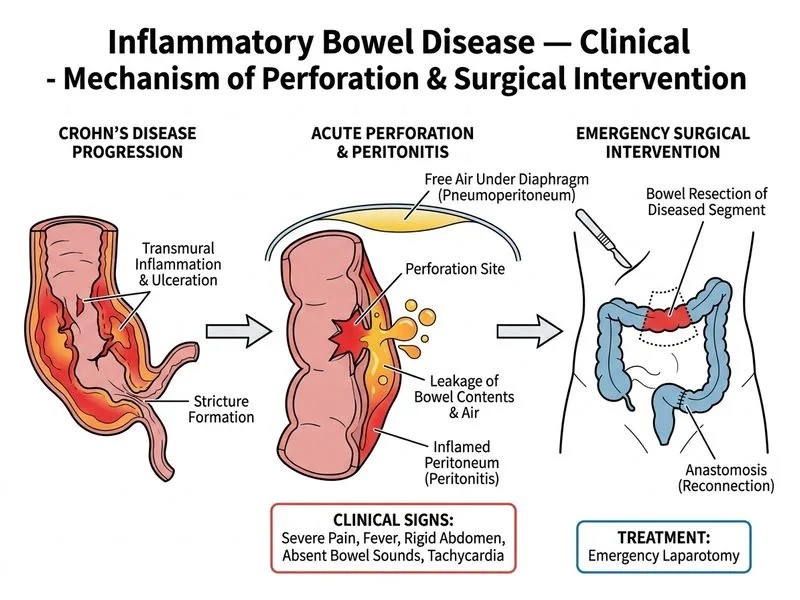
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.