## Clinical Diagnosis This patient has **Crohn's disease with an intra-abdominal abscess** (ileocaecal region): - Fever, localised abdominal pain, palpable mass - CT findings: 6 cm complex mass with internal fluid collection (abscess) - Elevated inflammatory markers - Known Crohn's disease with ileocaecal involvement ## Abscess in Crohn's Disease: Epidemiology & Pathophysiology **Key Point:** Intra-abdominal abscesses occur in 10–30% of Crohn's disease patients, typically from: - Transmural inflammation with fistulization - Perforation of diseased bowel - Mesenteric lymphadenitis with localized suppuration ## Management Algorithm for CD with Abscess ```mermaid flowchart TD A[Crohn's disease + abscess]:::outcome --> B{Abscess >3 cm or symptomatic?}:::decision B -->|Yes| C[Percutaneous drainage]:::action B -->|No| D[Medical management alone]:::action C --> E[Continue/optimize immunosuppression]:::action D --> E E --> F{Clinical improvement?}:::decision F -->|Yes| G[Maintain remission therapy]:::action F -->|No| H[Consider escalation or surgery]:::action ``` ## Why Percutaneous Drainage + Medical Therapy? **High-Yield:** The modern paradigm for **CD-related abscesses >3 cm** is: 1. **Percutaneous drainage** (CT or ultrasound-guided): - Success rate: >90% for abscesses >3 cm - Avoids emergency surgery - Allows time for medical optimization - Can be done under local anaesthesia with minimal morbidity 2. **Continue/optimize immunosuppression:** - Azathioprine continuation is safe post-drainage - Consider adding anti-TNF (infliximab/adalimumab) if not already on it - Allows healing of underlying disease and fistula closure 3. **Timing of surgery:** - Elective resection after drainage and medical optimization (4–12 weeks) - Avoids emergency surgery with higher morbidity - Allows inflammation to settle before resection **Clinical Pearl:** In the era of biologics, percutaneous drainage + medical therapy has reduced emergency surgery rates in CD-related abscesses from ~70% to <20%. ## Comparative Management Strategies | Strategy | Indication | Outcome | |----------|-----------|----------| | **Percutaneous drainage + medical Rx** | Abscess >3 cm, stable patient | Healing in 80–90%; elective surgery later if needed | | **Medical therapy alone** | Abscess <3 cm, minimal symptoms | Success in ~50%; risk of rupture | | **Immediate surgery** | Perforation, septic shock, failed drainage | High morbidity; reserved for emergencies | | **Increase immunosuppression without drainage** | Dangerous | Risk of abscess rupture, peritonitis, sepsis | ## Why Not the Other Options? **Option 0 (Increase azathioprine + add infliximab):** - Escalating immunosuppression without draining a 6 cm abscess risks rupture and peritonitis - Drainage must precede or accompany medical escalation - This is a **trap answer** — it sounds "aggressive" but is actually dangerous **Option 2 (Immediate surgical resection):** - Reserved for: - Perforation or peritonitis - Failed percutaneous drainage - Septic shock - Uncontrolled sepsis despite drainage - Elective surgery after drainage has lower morbidity and mortality - This patient is stable and suitable for drainage **Option 3 (Discontinue azathioprine + high-dose corticosteroids):** - Stopping azathioprine removes disease-modifying therapy - Corticosteroids alone are insufficient for abscess management - No role in acute abscess management ## Post-Drainage Management **Key Point:** After successful drainage: 1. Continue azathioprine (safe; does not increase infection risk post-drainage) 2. Consider adding anti-TNF if not already on it (improves fistula closure) 3. Reassess at 4–8 weeks 4. Plan elective resection if abscess recurs or underlying disease not controlled [cite:Harrison 21e Ch 319; Robbins 10e Ch 17] 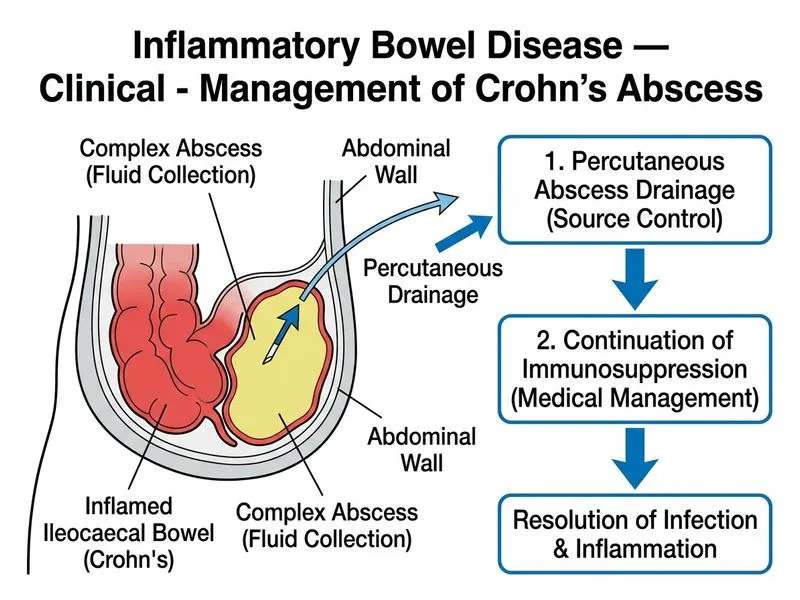
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.