## Clinical Context This elderly woman with untreated atrial fibrillation (AF) presents with acute MCA territory stroke. The irregular pulse and AF history are critical clues to the underlying mechanism. ## Key Point: **Atrial fibrillation is the single most important modifiable risk factor for cardioembolic stroke.** Patients with AF have a 4–5 fold increased risk of ischemic stroke due to blood stasis in the fibrillating atrium, promoting thrombus formation [cite:Harrison 21e Ch 434]. ## Pathophysiology of Cardioembolic Stroke in AF 1. **Loss of atrial contraction** → blood stasis in the left atrial appendage (LAA) 2. **Thrombus formation** in the LAA (risk increases with CHA₂DS₂-VASc score) 3. **Embolization** of thrombus into the cerebral circulation 4. **Occlusion of large cerebral vessels** (commonly MCA), causing territorial infarction ## High-Yield: **AF-related strokes are typically:** - Large territorial infarcts (not lacunar) - Occur in major vessel territories (MCA > ACA > PCA) - Often recurrent if anticoagulation is not initiated - Associated with higher disability and mortality than atherosclerotic strokes ## Mnemonic: CHA₂DS₂-VASc Score **C** — Congestive heart failure (1 point) **H** — Hypertension (1 point) **A₂** — Age ≥75 (2 points) **D** — Diabetes (1 point) **S₂** — Stroke/TIA/thromboembolism (2 points) **V** — Vascular disease (1 point) **A** — Age 65–74 (1 point) **Sc** — Sex category (female, 1 point) Score ≥2 in men or ≥3 in women → anticoagulation indicated. ## Clinical Pearl: **This patient should have been on anticoagulation (warfarin INR 2–3 or DOAC) given her age and AF.** The stroke is a direct consequence of non-adherence to guideline-directed medical therapy. Post-stroke, she requires urgent anticoagulation (after excluding hemorrhage transformation) and long-term stroke prevention. 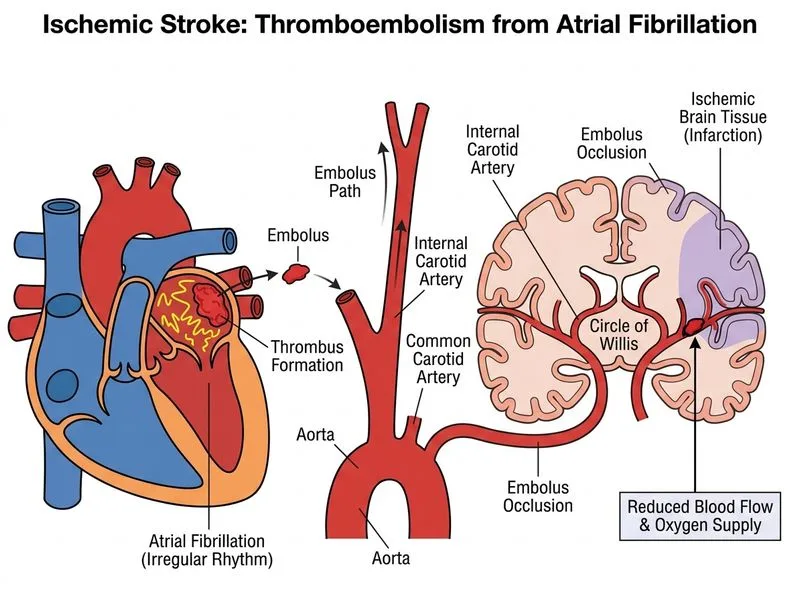
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.