## Critical IUGR with Severe Placental Insufficiency This patient has **severe early-onset IUGR** (weight <10th percentile at 28 weeks) complicated by **preeclampsia** (hypertension + proteinuria) and **absent end-diastolic flow (AEDF)** on umbilical artery Doppler—a marker of severe placental insufficiency with high risk of intrauterine fetal death and neonatal compromise. ### Doppler Classification and Management Thresholds | Doppler Finding | Umbilical Artery Pattern | Risk Level | Gestational Age <34 weeks | Gestational Age ≥34 weeks | |---|---|---|---|---| | Normal | Positive diastolic flow | Low | Routine care | Routine care | | Elevated PI | Positive but reduced diastolic | Intermediate | Twice-weekly surveillance | Consider delivery | | AEDF | Absent diastolic flow | **High** | **Steroids + deliver 24–48 hrs** | **Deliver immediately** | | Reversed diastolic flow | Negative diastolic flow | **Critical** | **Steroids + deliver 24–48 hrs** | **Deliver immediately** | **Key Point:** AEDF at <34 weeks is an indication for **corticosteroid administration followed by delivery within 24–48 hours**, not expectant management. The risk of intrauterine fetal death exceeds the benefit of prolonging pregnancy for further fetal maturation. ### Management Algorithm for AEDF at 28 Weeks ```mermaid flowchart TD A[IUGR + AEDF at 28 weeks]:::outcome --> B{Maternal condition?}:::decision B -->|Preeclampsia or maternal instability| C[Admit immediately]:::action B -->|Stable| C C --> D[Administer IV MgSO₄ for neuroprotection]:::action C --> E[Give betamethasone 12 mg IM × 2 doses, 24 hrs apart]:::action E --> F[Deliver within 24–48 hours after 1st steroid dose]:::action F --> G[Prepare NICU; plan cesarean if non-reassuring FHR]:::action ``` **Clinical Pearl:** The **GRIT trial** (Growth Restriction Intervention Trial) showed that in early-onset IUGR with abnormal Doppler, **immediate delivery** (without steroids) was associated with higher perinatal mortality than **delayed delivery after corticosteroid administration**. However, the delay should not exceed 48 hours; prolonged expectant management with AEDF leads to intrauterine fetal death. **High-Yield:** Management of AEDF at <34 weeks: 1. **Admit immediately** for continuous fetal monitoring 2. **Magnesium sulfate** 4 g IV bolus, then 1 g/hr infusion (neuroprotection for preterm neonate) 3. **Betamethasone** 12 mg IM, repeat in 24 hours (accelerates fetal lung maturity) 4. **Deliver within 24–48 hours** after first steroid dose (optimal window for neonatal benefit) 5. **Cesarean delivery** is preferred if FHR is non-reassuring or labor does not progress **Mnemonic:** **AEDF = Admit, Evaluate, Deliver, Fetal neuroprotection** - **A**dmit for continuous monitoring - **E**valuate maternal condition (preeclampsia, abruption) - **D**eliver within 24–48 hours - **F**etal neuroprotection (MgSO₄) + fetal lung maturation (steroids) **Warning:** Do not attempt expectant management (option D) with AEDF—this is a high-risk scenario with significant risk of intrauterine fetal death. The presence of preeclampsia further increases maternal and fetal risk. 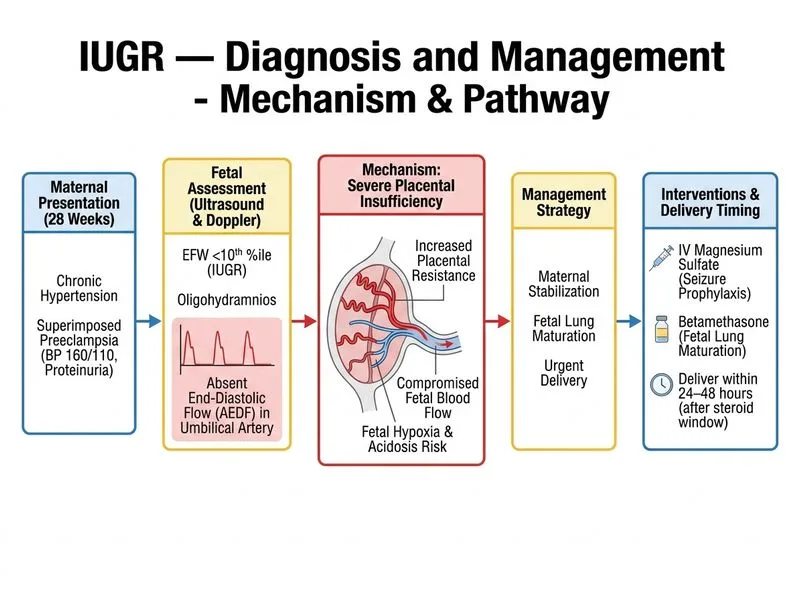
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.