## Critical IUGR: AEDF with Abnormal Cerebral Doppler **Key Point:** This patient has **severe IUGR with absent end-diastolic flow (AEDF) in the umbilical artery AND abnormal MCA Doppler (low PI indicating cerebral vasodilatation)**. This combination represents **advanced placental insufficiency with fetal compensation failing** — a critical state requiring delivery within days, not weeks. ### Doppler Severity Stratification | Doppler Finding | Severity | Management | |-----------------|----------|------------| | Elevated UA PI/RI, normal CPR | Mild-moderate | Twice-weekly monitoring, deliver if deteriorates | | Elevated UA PI/RI, low CPR | Moderate-severe | Admit, twice-weekly Doppler, deliver if REDF develops | | REDF (reversed end-diastolic flow) | Severe | Daily monitoring, deliver within 48 hrs if stable | | AEDF (absent end-diastolic flow) | Very severe | **Daily monitoring, deliver at 30 weeks or if deterioration** | | AEDF + abnormal MCA/DV | Critical | **Deliver within 24–48 hrs** | **High-Yield:** **AEDF + low MCA PI = fetal decompensation.** The low MCA PI indicates the fetus is attempting maximal cerebral vasodilatation (brain-sparing) but is failing to maintain adequate cerebral perfusion. This is a **pre-terminal state**. ### Pathophysiology of Deterioration ```mermaid flowchart TD A[Placental insufficiency]:::outcome --> B[Elevated UA resistance]:::outcome B --> C[Reduced umbilical blood flow]:::outcome C --> D[Fetal hypoxemia]:::outcome D --> E[Cerebral vasodilatation<br/>MCA PI decreases]:::action E --> F{Compensation adequate?}:::decision F -->|Yes| G[Stable, continue monitoring]:::action F -->|No| H[Fetal acidosis, bradycardia<br/>Ductus venosus abnormality]:::urgent H --> I[Deliver urgently]:::urgent ``` ### Why Not Immediate Delivery? **Clinical Pearl:** Although AEDF is severe, the fetus currently has **normal baseline heart rate and variability** — signs of compensation. Delivery at 28 weeks carries **>90% survival but 40–50% neurodevelopmental morbidity**. The standard approach is: 1. **Administer antenatal corticosteroids immediately** (betamethasone 12 mg IM × 2 doses, 24 hrs apart) to reduce neonatal respiratory distress and intraventricular hemorrhage. 2. **Admit for daily monitoring** (CTG + Doppler) to detect acute decompensation (loss of variability, bradycardia, reversed flow in ductus venosus, oligohydramnios). 3. **Deliver if deterioration occurs OR at 32 weeks** (balancing IUGR mortality against prematurity morbidity). **Warning:** Do NOT discharge home — AEDF can progress to ductus venosus reversal or fetal bradycardia within hours. Do NOT perform fetal blood sampling (cordocentesis) — it is invasive, time-consuming, and not indicated when Doppler findings already mandate delivery within days. ### Distinction from Mild IUGR **Mnemonic: "AEDF = Admit, Evaluate, Deliver Frequently"** — these fetuses need daily assessment and delivery within 3–5 days unless they reach a safer gestational age (32+ weeks) without deterioration. [cite:RCOG Green-top Guideline 31; ACOG Practice Bulletin #204 on Fetal Growth Restriction] 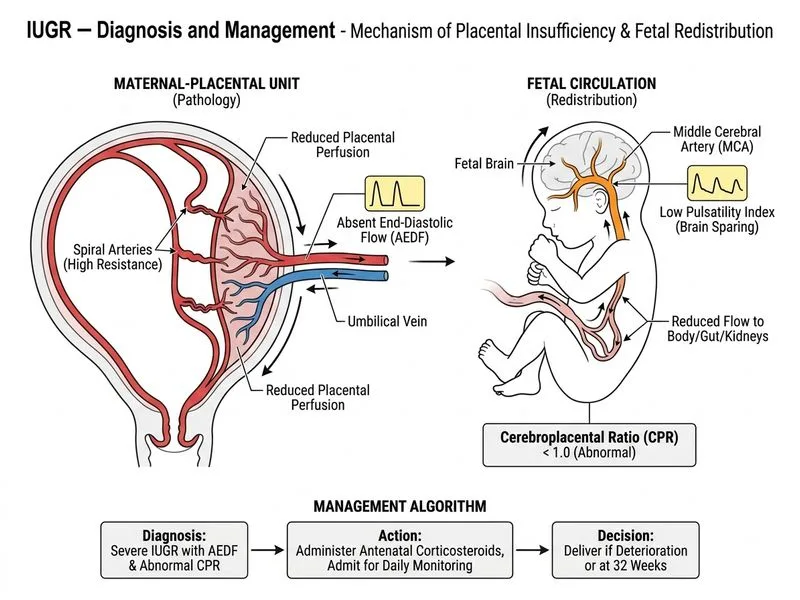
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.