## Paraneoplastic Syndromes in SCLC **Key Point:** Small cell lung cancer is the **most common malignancy associated with paraneoplastic syndromes**, occurring in 10–15% of patients. SCLC frequently secretes ectopic hormones (ACTH, ADH, calcitonin) and produces autoantibodies against neuronal and muscle antigens. ### Clinical Analysis of This Case | Finding | Interpretation | Mechanism | |---|---|---| | **Hyponatremia (Na 118)** | SIADH | Ectopic ADH secretion by tumor cells | | **Hypercalcemia (Ca 12.8)** | PTHrP secretion or osteolytic metastases | Ectopic parathyroid hormone-related peptide (PTHrP) | | **Hypokalemia (K 2.8)** | Hypokalemic metabolic alkalosis | Ectopic ACTH → cortisol excess → urinary K^+^ wasting | | **Proximal muscle weakness** | Steroid myopathy + hypokalemia | Cortisol excess + K^+^ depletion | | **Polyuria, polydipsia** | Hyperglycemia from cortisol excess | Ectopic ACTH → Cushing syndrome | | **Nausea** | Hypercalcemia + hyponatremia | Both cause GI symptoms | ### Ectopic Hormone Production in SCLC ```mermaid flowchart TD A[SCLC Diagnosis]:::outcome --> B[Neuroendocrine Differentiation]:::action B --> C[Ectopic Hormone Secretion]:::action C --> D1[ACTH]:::action C --> D2[ADH]:::action C --> D3[Calcitonin]:::action D1 --> E1[Cushing Syndrome]:::outcome D2 --> E2[SIADH]:::outcome D3 --> E3[Hypercalcemia]:::outcome E1 --> F1[Hypokalemia, Hyperglycemia, Hypertension]:::outcome E2 --> F2[Hyponatremia, Seizures, Confusion]:::outcome E3 --> F3[Polyuria, Polydipsia, Altered Mental Status]:::outcome ``` **High-Yield:** **SCLC is the most common cause of ectopic ACTH syndrome** (Cushing syndrome of malignancy), accounting for ~50% of all ectopic ACTH cases. The combination of **SIADH + Cushing syndrome** in a SCLC patient is pathognomonic. ### Why This Patient Has Both SIADH and Cushing Syndrome 1. **Ectopic ACTH:** SCLC cells express proopiomelanocortin (POMC), which is cleaved to ACTH. This drives cortisol overproduction → hypokalemia, hyperglycemia, muscle weakness, and hypertension. 2. **Ectopic ADH:** The same neuroendocrine tumor cells also secrete ADH, causing water retention and hyponatremia. 3. **PTHrP secretion:** Some SCLC tumors produce PTHrP, contributing to hypercalcemia. **Clinical Pearl:** The **hypokalemia in this case is severe (2.8 mEq/L) and multifactorial**: - Ectopic ACTH → cortisol excess → renal K^+^ wasting - Hyponatremia → osmotic shifts - Possible concurrent hypomagnesemia (common in Cushing syndrome) This combination explains the proximal muscle weakness and hyporeflexia (steroid myopathy + electrolyte derangement). ### Diagnostic Confirmation | Test | Expected Finding in This Case | |---|---| | **24-hour urinary cortisol** | Markedly elevated (>300 μg/24 h) | | **Plasma ACTH** | Elevated (>200 pg/mL) — ectopic source | | **Low-dose dexamethasone suppression test** | NO suppression (distinguishes ectopic ACTH from pituitary Cushing) | | **Serum osmolality** | Low (<280 mOsm/kg) | | **Urine osmolality** | Inappropriately high (>100 mOsm/kg) despite hyponatremia | ### Treatment Approach 1. **Urgent:** Correct hypokalemia (K^+^ repletion) and hyponatremia (fluid restriction for SIADH). 2. **Cortisol control:** Mitotane or ketoconazole to inhibit 11β-hydroxylase and reduce ACTH-driven cortisol synthesis. 3. **Definitive:** Initiate SCLC-directed chemotherapy (cisplatin + etoposide); tumor response often resolves paraneoplastic syndromes. **Warning:** Do NOT give dexamethasone to suppress ACTH in ectopic ACTH syndrome — it will NOT work (unlike pituitary Cushing). Use steroid synthesis inhibitors instead. 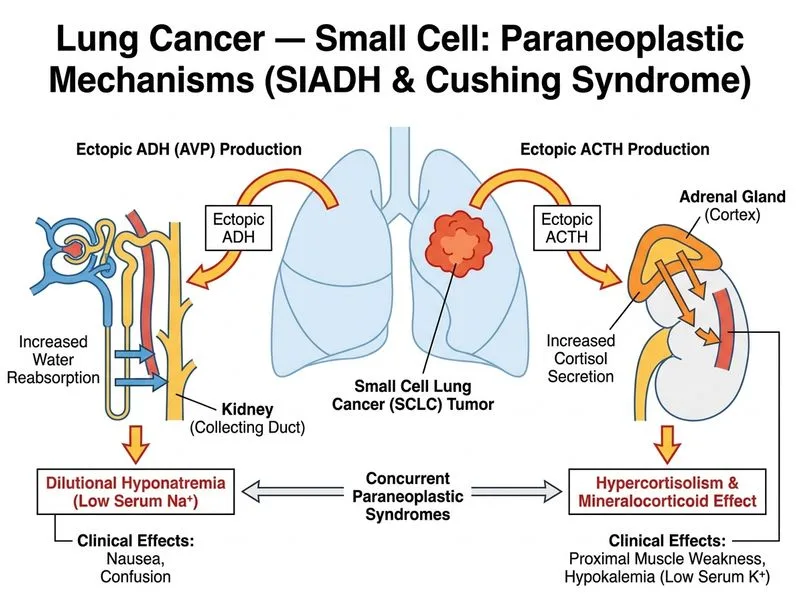
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.