## Clinical Presentation Analysis ### Key Clinical Findings **High-Yield:** The patient presents with: - **Hyponatremia** (Na 118 mEq/L) with low serum osmolality (245 mOsm/kg) - **Inappropriately concentrated urine** (osmolality 580 mOsm/kg despite hypo-osmolar serum) - **Neuropsychiatric symptoms:** weakness, altered mental status (implied by diplopia/ptosis confusion) - **Limited-stage SCLC** (left perihilar, ipsilateral hilar nodes only — no contralateral or distant metastases) **Key Point:** This constellation of findings is pathognomonic for **Syndrome of Inappropriate Antidiuretic Hormone (SIADH)** secretion. ## Diagnostic Criteria for SIADH | Criterion | Patient's Finding | Normal Range | |-----------|-------------------|---------------| | Serum sodium | 118 mEq/L | 135–145 mEq/L | | Serum osmolality | 245 mOsm/kg | 280–295 mOsm/kg | | Urine osmolality | 580 mOsm/kg | <100 mOsm/kg (if serum hypo-osmolar) | | Urine sodium | (Presumed elevated) | >40 mEq/L in SIADH | | TSH, cortisol | (Presumed normal) | Normal | | Volume status | Euvolemic | Clinically euvolemic | **Clinical Pearl:** SIADH is the most common paraneoplastic endocrine syndrome in SCLC, occurring in 10–15% of cases. It results from **ectopic ADH (vasopressin) production** by neuroendocrine tumor cells. ## Mechanism of Ectopic ADH Production ```mermaid flowchart TD A[SCLC cells]:::outcome --> B[Neuroendocrine differentiation]:::outcome B --> C[Ectopic ADH synthesis and release]:::action C --> D[Increased water reabsorption in collecting duct]:::action D --> E[Hyponatremia + hypo-osmolality]:::outcome E --> F[Inappropriately concentrated urine]:::outcome F --> G[Neuropsychiatric symptoms<br/>Seizures, confusion, coma]:::urgent ``` **Key Point:** SCLC is a **neuroendocrine malignancy** with high propensity for ectopic hormone production. The tumor cells synthesize and secrete ADH (vasopressin) autonomously, leading to: 1. Increased aquaporin-2 expression in renal collecting duct 2. Enhanced water reabsorption 3. Dilutional hyponatremia and hypo-osmolality 4. Paradoxically concentrated urine (osmolality >serum osmolality) ## Paraneoplastic Syndromes in SCLC | Syndrome | Mechanism | Frequency | Clinical Features | |----------|-----------|-----------|-------------------| | **SIADH** | Ectopic ADH | 10–15% | Hyponatremia, hypo-osmolality, concentrated urine | | **Cushing syndrome** | Ectopic ACTH | 2–5% | Hypokalemia, metabolic alkalosis, hypertension, hyperglycemia | | **Eaton-Lambert** | Anti-VGCC antibodies | 3–5% | Proximal muscle weakness, autonomic dysfunction, areflexia | | **Myasthenia gravis** | Anti-AChR antibodies | <1% | Ocular/bulbar/generalized weakness, fatigability | **Mnemonic:** **ACES** — paraneoplastic syndromes in SCLC: - **A**DIADH (most common) - **C**ushing syndrome - **E**aton-Lambert myasthenic syndrome - **S**ubacute sensory neuropathy ## Why Other Options Are Incorrect **Option 1 (Eaton-Lambert):** While Eaton-Lambert is a paraneoplastic syndrome in SCLC (3–5% incidence), it presents with **proximal muscle weakness, diminished reflexes, and autonomic dysfunction** — NOT hyponatremia. The mechanism involves **anti-VGCC (voltage-gated calcium channel) antibodies** affecting presynaptic neuromuscular transmission. The patient's hyponatremia and SIADH are not explained by this diagnosis. **Option 2 (Cushing syndrome):** Ectopic ACTH production by SCLC causes Cushing syndrome in 2–5% of cases, presenting with **hypokalemia, metabolic alkalosis, hypertension, and hyperglycemia** — NOT hyponatremia. The patient's electrolyte abnormality (hyponatremia with low osmolality) is inconsistent with ACTH-secreting tumors. **Option 3 (Myasthenia gravis):** MG is caused by **anti-acetylcholine receptor (anti-AChR) antibodies** and presents with **ocular weakness (ptosis, diplopia), bulbar symptoms, and fatigability** — features that can overlap with the patient's presentation. However, MG does NOT cause hyponatremia or SIADH. The diplopia and ptosis in this patient are secondary to **hyponatremia-induced neuropsychiatric symptoms** (confusion, weakness), not primary neuromuscular junction dysfunction. **Warning:** Do NOT confuse the neuropsychiatric symptoms of severe hyponatremia (confusion, weakness, seizures) with primary neurological paraneoplastic syndromes. The hyponatremia and SIADH are the primary diagnosis here. ## Clinical Management Implications **High-Yield:** Treatment of SIADH in SCLC includes: 1. **Fluid restriction** (500–1000 mL/day) — first-line for asymptomatic hyponatremia 2. **Hypertonic saline** (3%) — for symptomatic or severe hyponatremia (<120 mEq/L with seizures) 3. **Chemotherapy** — addresses the underlying malignancy and often resolves SIADH 4. **Vaptans** (vasopressin antagonists) — if refractory to fluid restriction [cite:Robbins 10e Ch 15; Harrison 21e Ch 105] 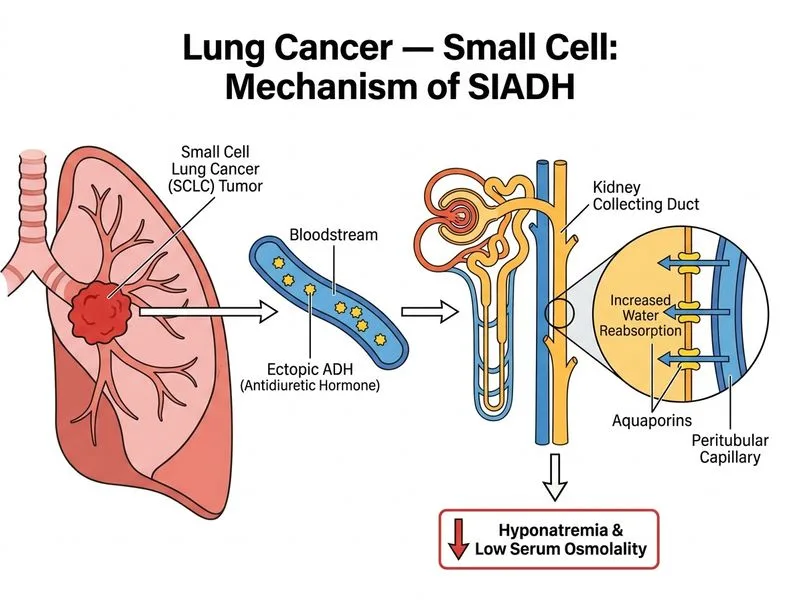
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.