## Pathophysiology of Acute MSUD Encephalopathy ### Mechanism of Neurological Injury **Key Point:** In maple syrup urine disease (MSUD), the defect lies in the branched-chain α-ketoacid dehydrogenase complex (BCKDC), which catalyzes the irreversible oxidative decarboxylation of branched-chain α-ketoacids (BCKAs) derived from leucine, isoleucine, and valine. This blockade causes accumulation of both BCAAs and their corresponding α-ketoacids (α-ketoisocaproate, α-keto-β-methylvalerate, α-ketoisovalerate). ### Why Option C (Correct Answer) is Right The accumulated branched-chain α-ketoacids — particularly **α-ketoisocaproate (from leucine)** — are potent inhibitors of key mitochondrial enzyme complexes: 1. **α-Ketoglutarate dehydrogenase inhibition**: BCKAs structurally resemble α-ketoglutarate and competitively inhibit this critical TCA cycle enzyme, reducing NADH generation and oxidative phosphorylation. 2. **Pyruvate dehydrogenase inhibition**: Further impairs the glycolysis–TCA cycle link, compounding the energy deficit. 3. **Cerebral energy crisis**: The brain is almost entirely dependent on oxidative metabolism. Inhibition of these enzymes causes acute ATP depletion, manifesting as encephalopathy, ataxia, and seizures. This mechanism is supported by the clinical observation that acute MSUD crises respond to aggressive BCAA restriction combined with high-dose glucose and lipid infusion — interventions that restore cerebral energy metabolism by providing alternative substrates and suppressing BCAA catabolism. **High-Yield:** The acute pathophysiology is **metabolic energy failure** driven by BCKA-mediated inhibition of the TCA cycle, not neurotransmitter imbalance or acute demyelination. ### Why Each Distractor is Wrong #### Option A: LNAA competition at LAT1 transporter (INCORRECT — contributes to chronic, not acute, injury) Elevated BCAAs do compete with large neutral amino acids (tryptophan, tyrosine, phenylalanine) for the LAT1 transporter at the blood-brain barrier, reducing monoamine neurotransmitter synthesis. However, this is a **chronic, secondary mechanism** contributing to long-term neurodevelopmental impairment, not the primary driver of **acute** encephalopathy in a metabolic crisis. Acute crises are characterized by rapid energy failure, not gradual neurotransmitter depletion. #### Option B: Alloisoleucine as a false neurotransmitter (INCORRECT — alloisoleucine is a diagnostic marker, not a pathogenic agent) Alloisoleucine is the allo-isomer of isoleucine that accumulates in MSUD and is pathognomonic when plasma levels exceed 100 µmol/L. However, there is **no evidence** in the literature that alloisoleucine acts as a false neurotransmitter or competitively antagonizes GABA receptors. It is a biochemical marker of the disease, not a causative agent of acute neurological deterioration. #### Option D: Demyelination via myelin basic protein inhibition (INCORRECT — mechanism of chronic, not acute, MSUD) Chronic MSUD can cause demyelination and white matter disease due to prolonged exposure to elevated BCKAs, which impair myelin synthesis and maintenance. However, demyelination is a **long-term consequence** developing over weeks to months of repeated metabolic crises. The acute encephalopathy described in this vignette (hours to days) is due to acute energy depletion, not demyelination. --- ## Clinical Correlations **Clinical Pearl:** Acute MSUD encephalopathy is a medical emergency requiring: - Immediate cessation of BCAA intake (protein restriction or BCAA-free formula) - High-dose glucose and lipid infusion to provide alternative cerebral fuel and suppress BCAA catabolism - Dialysis (hemodialysis or CRRT) to rapidly remove accumulated BCAAs and α-ketoacids - Correction of cerebral edema (mannitol, hypertonic saline) **Mnemonic:** **MSUD = Metabolic Toxicity** (energy failure). The acute crisis is an **energy crisis** caused by BCKA inhibition of the TCA cycle. --- ## Biochemical Basis The branched-chain α-ketoacid dehydrogenase complex is a multi-enzyme complex analogous to pyruvate dehydrogenase, requiring cofactors including thiamine pyrophosphate (TPP), lipoic acid, FAD, and NAD⁺. Deficiency of any subunit (E1α, E1β, E2, E3, or E3-binding protein) causes MSUD. The accumulated BCKAs are potent inhibitors of: - **α-Ketoglutarate dehydrogenase** (TCA cycle — primary acute mechanism) - **Pyruvate dehydrogenase** (glycolysis–TCA link) - Branched-chain aminotransferase (feedback inhibition) This creates a **metabolic bottleneck** that severely impairs cerebral energy production and causes acute neurological deterioration. [cite:Robbins 10e Ch 5; Harper's Illustrated Biochemistry 31e Ch 29] 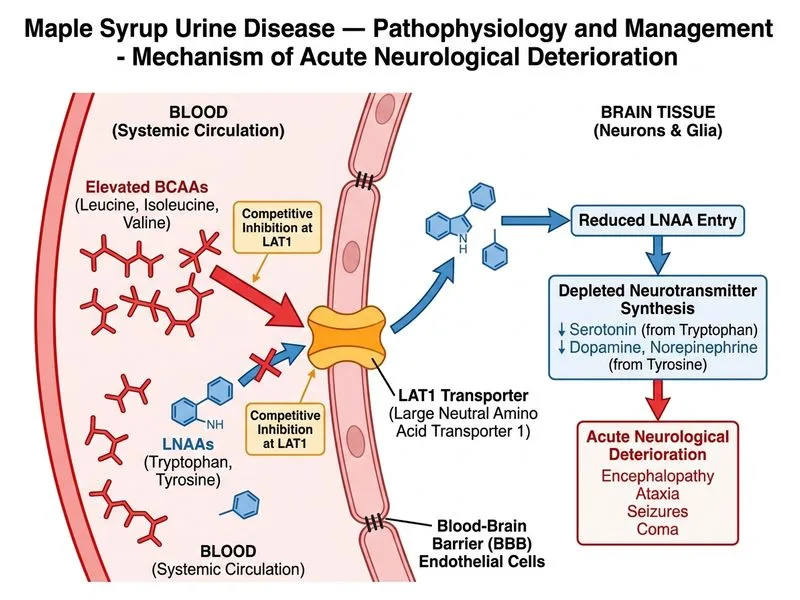
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.