## Diagnosis: MEN 2A Syndrome ### Clinical Features Pointing to MEN 2A **Key Point:** MEN 2A is characterised by the triad of medullary thyroid carcinoma (MTC), phaeochromocytoma, and primary hyperparathyroidism (pHPT). The presence of MTC in a first-degree relative (son) is the sentinel finding. ### Differential Analysis | Feature | MEN 2A | MEN 1 | Familial HCH | |---------|--------|-------|---------------| | **Medullary thyroid cancer** | ~95% (earliest manifestation) | Rare | Absent | | **Phaeochromocytoma** | ~50% | Rare | Absent | | **Primary hyperparathyroidism** | ~20–30% | ~95% | Absent | | **Pancreatic neuroendocrine tumours** | Absent | ~70% | Absent | | **Pituitary adenoma** | Absent | ~40% | Absent | | **Genetic basis** | RET proto-oncogene (gain-of-function) | MEN1 gene (tumour suppressor) | CASR gene (loss-of-function) | | **PTH level in hypercalcaemia** | Elevated | Elevated | Suppressed | **High-Yield:** In this patient: - **Son with MTC** → MEN 2A or MEN 2B (not MEN 1) - **Sister with pHPT** → Autosomal dominant inheritance pattern - **Elevated PTH with hypercalcaemia** → Rules out familial hypocalciuric hypercalcaemia (where PTH is suppressed) - **Abdominal mass** → Likely phaeochromocytoma (present in ~50% of MEN 2A) ### Why MEN 2A and Not MEN 2B? MEN 2B includes MTC, phaeochromocytoma, and mucosal neuromas / marfanoid habitus. The patient has no mention of oral neuromas or skeletal features, making MEN 2A more likely. ### Pathophysiology **Key Point:** MEN 2A is caused by activating mutations in the **RET proto-oncogene** (chromosome 10q11.2). This leads to constitutive activation of the RET receptor tyrosine kinase, causing: 1. C-cell hyperplasia → medullary thyroid carcinoma (earliest, ~100% penetrance by age 70) 2. Chromaffin cell proliferation → phaeochromocytoma 3. Parathyroid hyperplasia → primary hyperparathyroidism **Clinical Pearl:** MTC is the most common and earliest manifestation of MEN 2A. Calcitonin and carcinoembryonic antigen (CEA) screening are essential in all RET mutation carriers. Prophylactic thyroidectomy is recommended in childhood (by age 5–10) for RET-positive family members. ### Management Implications 1. **Genetic testing:** RET mutation analysis in the patient and all first-degree relatives 2. **Screening protocol:** - Annual serum calcitonin and CEA - Plasma free metanephrines (phaeochromocytoma screening) - Serum calcium and PTH (parathyroid surveillance) - Thyroid ultrasound 3. **Prophylactic thyroidectomy** in RET-positive family members (especially children) 4. **Adrenalectomy** if phaeochromocytoma confirmed 5. **Parathyroidectomy** if symptomatic pHPT **Mnemonic: MEN 2A = "MTC + Pheo + PTH"** (Medullary Thyroid Cancer, Phaeochromocytoma, Primary hyperparathyroidism) [cite:Robbins 10e Ch 24] 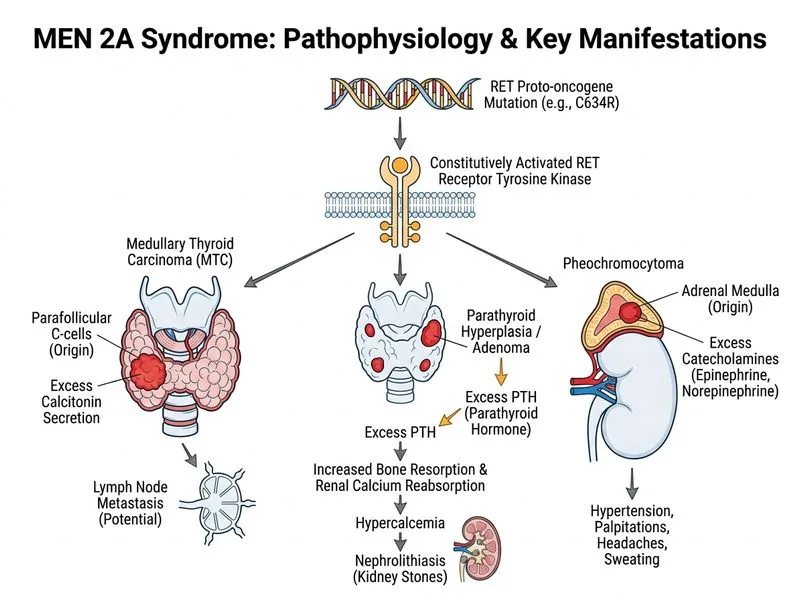
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.