## Diagnosis: MEN 1 Syndrome ### Clinical Triad Identification **Key Point:** MEN 1 is defined by the "3 P's": **Pituitary adenoma** (prolactinoma most common), **Parathyroid hyperplasia** (primary hyperparathyroidism), and **Pancreatic neuroendocrine tumours** (gastrinoma causing peptic ulcer disease). This patient and her family exhibit all three components: - **Patient:** Prolactin-secreting pituitary adenoma + borderline elevated PTH + adrenal nodule - **Brother:** Refractory peptic ulcer disease (gastrinoma → Zollinger-Ellison syndrome) - **Son:** Parathyroid adenoma (early-onset hyperparathyroidism) ### MEN 1 vs MEN 2A: Critical Distinction | Feature | MEN 1 | MEN 2A | |---------|-------|--------| | **Pituitary adenoma** | ~40% (prolactinoma most common) | Absent | | **Parathyroid hyperplasia/adenoma** | ~95% (earliest manifestation) | ~20–30% | | **Pancreatic NET** | ~70% (gastrinoma, insulinoma) | Absent | | **Medullary thyroid carcinoma** | Absent | ~95% | | **Phaeochromocytoma** | Absent | ~50% | | **Genetic basis** | MEN1 gene (chromosome 12q13) — tumour suppressor | RET proto-oncogene (chromosome 10q11.2) — gain-of-function | | **Inheritance** | Autosomal dominant (90% penetrance by age 40) | Autosomal dominant | | **Age of onset** | Typically 20–40 years | Earlier (MTC by age 5–10) | **High-Yield:** The **absence of medullary thyroid carcinoma** and **presence of gastrinoma** (peptic ulcer disease refractory to PPI) are diagnostic for MEN 1, not MEN 2A. ### Pathophysiology: MEN1 Gene Mutation **Key Point:** MEN 1 is caused by loss-of-function mutations in the **MEN1 gene** (chromosome 12q13), which encodes the **menin protein**. Menin is a tumour suppressor that: 1. Regulates histone acetylation and chromatin remodelling 2. Inhibits cell proliferation and promotes apoptosis 3. Acts as a scaffold protein for multiple signalling pathways Loss of menin function leads to: - **Parathyroid hyperplasia** → primary hyperparathyroidism (earliest, ~95%) - **Anterior pituitary adenomas** → prolactinoma (most common, ~40%), growth hormone-secreting adenoma, ACTH-secreting adenoma - **Pancreatic/gastroenteric neuroendocrine tumours** → gastrinoma (Zollinger-Ellison syndrome), insulinoma, VIPoma, non-functional NETs - **Adrenocortical tumours** → benign adenomas (common, usually non-functional) - **Carcinoid tumours** → thymic, bronchial, gastric ### Clinical Pearls for MEN 1 **Clinical Pearl:** Gastrinoma in MEN 1 (Zollinger-Ellison syndrome) presents with: - Severe, refractory peptic ulcer disease - Chronic diarrhoea - Elevated fasting serum gastrin (>1000 pg/mL is diagnostic) - Low gastric pH (<2) The brother's "peptic ulcer disease refractory to PPIs" is a red flag for gastrinoma, not simple GERD. **Clinical Pearl:** Parathyroid involvement in MEN 1 is typically **multiglandular hyperplasia** (not a single adenoma), which explains why the 8-year-old son has early-onset hyperparathyroidism — a hallmark of MEN 1 in children. ### Screening and Management 1. **Genetic testing:** MEN1 mutation analysis (diagnostic; ~90% of MEN 1 patients carry detectable mutations) 2. **Biochemical screening:** - Serum calcium, PTH, phosphate (parathyroid) - Fasting gastrin, gastric pH (gastrinoma) - Fasting insulin, C-peptide, glucose (insulinoma) - Prolactin, growth hormone, ACTH (pituitary) 3. **Imaging:** - MRI pituitary (prolactinoma surveillance) - Endoscopic ultrasound or CT/MRI abdomen (pancreatic NETs) - Adrenal imaging (usually benign, but monitor) 4. **Treatment:** - Dopamine agonists or surgery for prolactinoma - Parathyroidectomy (subtotal or total with autotransplantation) - Somatostatin analogues or surgery for gastrinoma **Mnemonic: MEN 1 = "3 P's + menin"** (Pituitary, Parathyroid, Pancreatic NETs + MEN1 gene mutation) [cite:Robbins 10e Ch 24; Harrison 21e Ch 439] 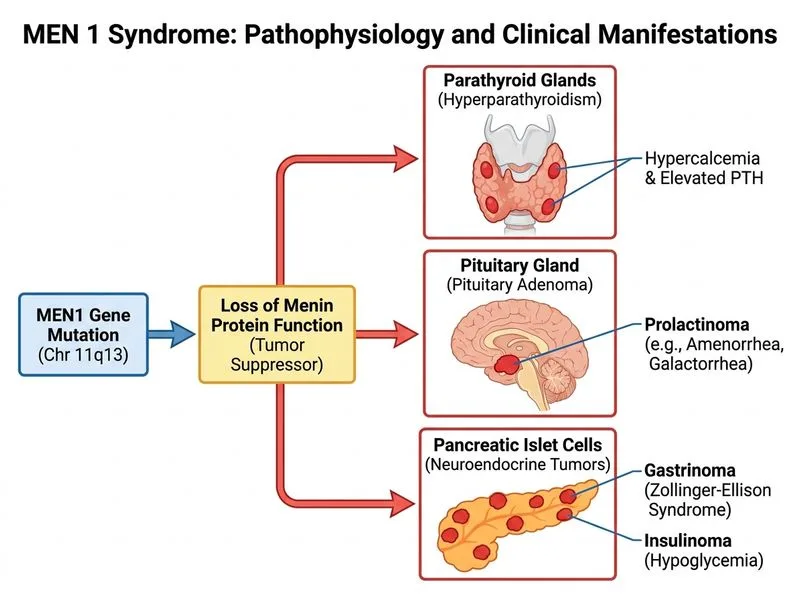
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.