## Temporal Pathology of Acute Myocardial Infarction **Key Point:** The pathological changes in MI evolve in a predictable temporal sequence. At 3 hours post-infarction, the myocardium is in the **early acute phase** characterized by coagulation necrosis with early neutrophilic infiltration. ### Timeline of MI Pathology | Time After Onset | Dominant Pathological Feature | Microscopic Finding | |---|---|---| | 0–4 hours | Coagulation necrosis (early) | Minimal inflammation; wavy fibers at border | | 4–12 hours | Coagulation necrosis (established) | Early neutrophilic infiltration begins | | 12–24 hours | Coagulation necrosis + neutrophils | Dense neutrophilic infiltrate | | 1–3 weeks | Granulation tissue formation | Macrophages, fibroblasts, neovascularization | | >3 weeks | Fibrosis/scarring | Collagen deposition, mature scar | **High-Yield:** At **3 hours**, the infarct zone shows: - Coagulation necrosis (ischemic necrosis) — the hallmark of MI - Wavy myofibers at the border (due to stretching by contracting adjacent muscle) - Early neutrophilic infiltration just beginning - Loss of striations and nuclei, but architecture preserved **Clinical Pearl:** Troponin elevation at 3 hours confirms myocardial necrosis has begun. The ECG changes (ST elevation) reflect acute transmural injury, but the histology at this timepoint is still predominantly coagulation necrosis. ### Why NOT the Other Patterns? - **Contraction band necrosis** (Option B): Occurs in reperfusion injury (after thrombolysis or PCI) or in catecholamine excess. Not the primary pattern in acute, ongoing ischemia. - **Hyaline necrosis** (Option C): Not a characteristic pattern in MI; seen in some infections or toxic injuries. - **Liquefactive necrosis** (Option D): Occurs weeks later (1–3 weeks) when macrophages digest the dead tissue, or in brain infarcts. At 3 hours, there is minimal macrophage infiltration. [cite:Robbins 10e Ch 12] 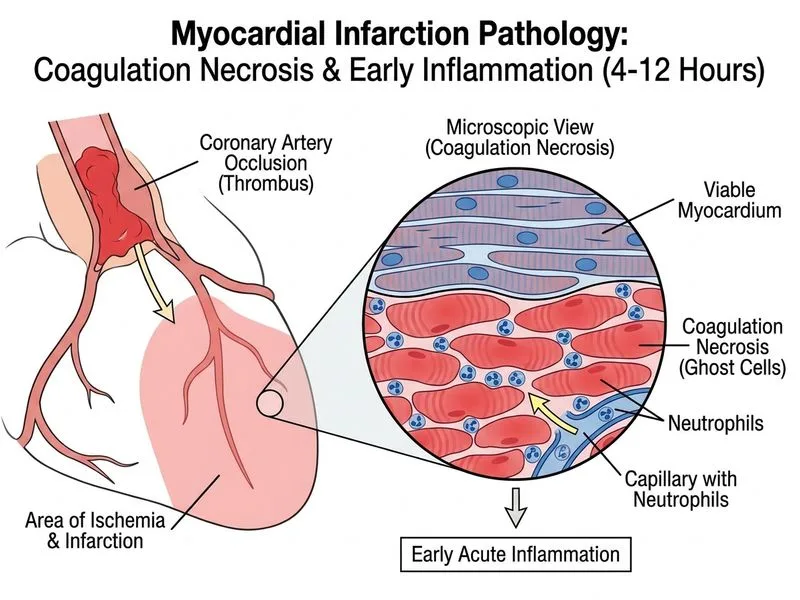
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.