## Clinical Presentation Analysis This patient presents with an **inferior wall MI** (ST elevation in II, III, aVF) complicated by sudden hemodynamic collapse with **bradycardia and hypotension**. ### Key Distinguishing Feature: Bradycardia **Key Point:** The combination of **inferior MI + bradycardia + hypotension** is pathognomonic for **right ventricular (RV) infarction with AV nodal ischemia**, NOT simple cardiogenic shock. ### Why RV Infarction Causes This Pattern 1. **Anatomical basis**: The AV node is supplied by the AV nodal artery, which arises from the RCA in 90% of cases 2. **RV infarction** (part of inferior MI territory) → ischemia of the AV node → **complete heart block or severe bradycardia** 3. **Loss of atrial contraction** ("atrial kick") accounts for 20–30% of RV preload; its loss causes acute RV failure 4. **Hypotension results** from: reduced RV contractility + loss of atrial kick + bradycardia (reduced cardiac output = HR × SV) ### Pathophysiology Timeline ```mermaid flowchart TD A[Inferior Wall MI<br/>RCA occlusion]:::outcome --> B[RV infarction<br/>+ AV node ischemia]:::outcome B --> C{Conduction block<br/>at AV node?}:::decision C -->|Yes| D[Bradycardia<br/>Complete/2nd degree block]:::urgent C -->|No| E[Sinus rhythm preserved] D --> F[Loss of atrial kick]:::outcome F --> G[Acute RV preload failure]:::outcome G --> H[Hypotension + Shock]:::urgent ``` ### Contrast with Other Complications | Complication | Presentation | Heart Rate | Mechanism | |---|---|---|---| | **RV infarction + nodal ischemia** | Inferior MI + bradycardia + hypotension | **↓↓ (40–50)** | AV node ischemia | | VSD rupture | Inferior MI + new holosystolic murmur | ↑ (compensatory) | Acute left-to-right shunt | | Papillary muscle rupture | Acute severe MR + pulmonary edema | ↑ (compensatory) | Acute regurgitation | | Free wall rupture | Sudden electromechanical dissociation | Variable | Pericardial tamponade | **Clinical Pearl:** In **RV infarction, fluid administration (cautious preload) may paradoxically improve BP**, whereas in cardiogenic shock from LV dysfunction, fluids worsen pulmonary edema. This is a key bedside discriminator. ### High-Yield Management Point **High-Yield:** Temporary pacing is often needed in RV infarction with complete heart block. Atropine (0.6 mg IV) may restore AV conduction by reducing vagal tone, but pacing is definitive. [cite:Robbins 10e Ch 12] 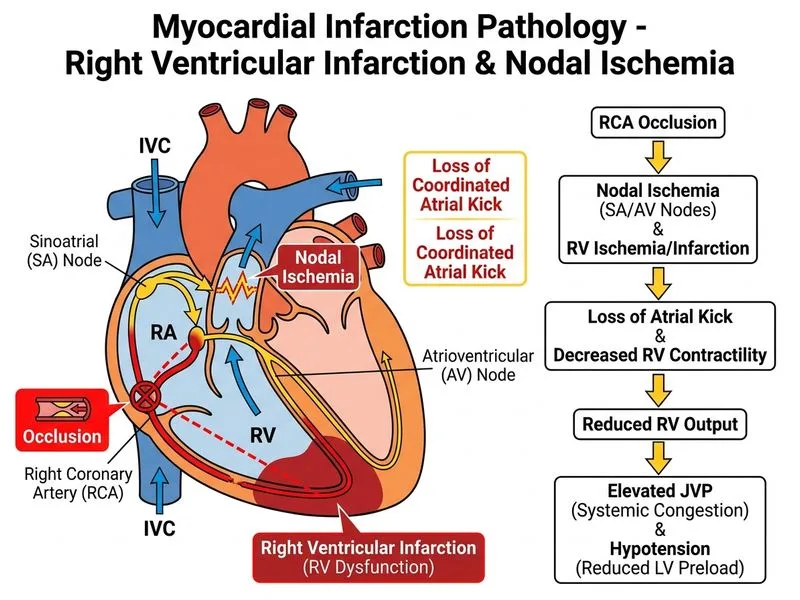
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.