## Diagnosis of ANCA-Associated Vasculitis (AAV) with Pulmonary-Renal Involvement ### Clinical Presentation Analysis The patient presents with: - **Pulmonary findings:** bilateral alveolar infiltrates (pulmonary haemorrhage) - **Renal findings:** acute nephritic syndrome with RBC casts, dysmorphic RBCs, proteinuria, and acute kidney injury - **Systemic features:** fever, respiratory symptoms This constellation is classic for **pulmonary-renal syndrome**, most commonly due to ANCA-associated vasculitis (granulomatosis with polyangiitis [GPA] or microscopic polyangiitis [MPA]). ### Role of ANCA Testing **Key Point:** c-ANCA with anti-PR3 and p-ANCA with anti-MPO antibodies are the most specific and sensitive investigations to diagnose ANCA-associated vasculitis. | Feature | c-ANCA + anti-PR3 | p-ANCA + anti-MPO | |---------|-------------------|-------------------| | **Associated disease** | GPA (Wegener granulomatosis) | MPA, EGPA | | **Sensitivity in systemic disease** | 90–95% | 50–70% | | **Pulmonary involvement** | Common (nodules, cavitation) | Alveolar haemorrhage | | **Renal pattern** | RPGN (necrotizing, pauci-immune) | RPGN (necrotizing, pauci-immune) | **High-Yield:** In pulmonary-renal syndrome: - **c-ANCA/anti-PR3** → suspect GPA - **p-ANCA/anti-MPO** → suspect MPA - **Negative ANCA** → consider anti-GBM disease (linear IgG on kidney biopsy) ### Why Not Kidney Biopsy Alone? While kidney biopsy with immunofluorescence (showing **pauci-immune necrotizing RPGN**) is confirmatory, it is **not the first-line investigation**. ANCA serology is non-invasive, rapid, and highly specific. Biopsy is performed **after** ANCA testing to confirm the pattern and exclude other diagnoses (e.g., anti-GBM disease, immune complex GN). ### Why Not ANA/Anti-dsDNA? These are markers of lupus nephritis, not ANCA-associated vasculitis. Lupus can cause pulmonary-renal syndrome, but the clinical context (acute presentation, bilateral infiltrates, RPGN pattern) and absence of other lupus features make AAV more likely. ANA would be negative in AAV. ### Why Not HRCT + BAL? These investigations characterize the pulmonary component (alveolar haemorrhage, infection, malignancy) but do **not diagnose vasculitis**. BAL with haemosiderin-laden macrophages confirms pulmonary haemorrhage but is non-specific. ANCA serology is more specific for the underlying diagnosis. **Clinical Pearl:** In suspected pulmonary-renal syndrome, the diagnostic sequence is: 1. **ANCA serology** (c-ANCA/anti-PR3 or p-ANCA/anti-MPO) — rapid, non-invasive, highly specific 2. **Kidney biopsy** (if ANCA positive or clinical suspicion high) — confirms pauci-immune RPGN pattern 3. **Chest imaging** (HRCT ± BAL) — characterizes pulmonary involvement and excludes infection/malignancy [cite:Harrison 21e Ch 319; Robbins 10e Ch 20] 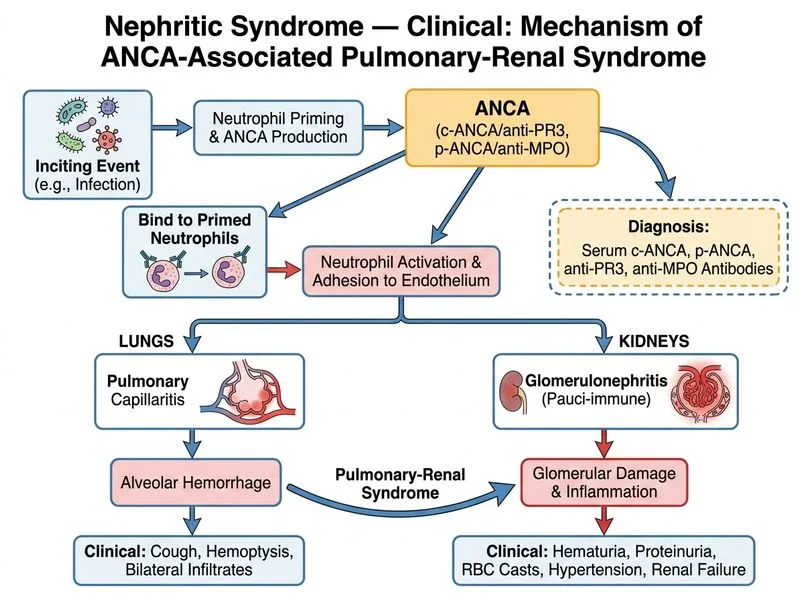
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.