## Diagnosis: Myelomeningocele ### Clinical Presentation The vignette describes a lumbosacral defect with: - Protruding sac containing neural tissue (not just meninges) - Exposed spinal cord elements - Bony vertebral defect - Markedly elevated maternal AFP (>3 MoM is highly suggestive of open neural tube defects) ### Pathophysiology **Key Point:** Myelomeningocele results from incomplete closure of the neural tube during weeks 3–4 of embryogenesis, with herniation of both meninges AND spinal cord tissue through the vertebral defect [cite:Langman's Embryology Ch 17]. ### Differential Features | Feature | Meningocele | Myelomeningocele | Spina Bifida Occulta | Anencephaly | |---------|-------------|------------------|----------------------|-------------| | **Contents of sac** | Meninges + CSF only | Meninges + CSF + neural tissue | None (skin-covered) | Absent brain/skull | | **Neural tissue exposed** | No | Yes | No | N/A | | **Bony defect** | Present | Present | Present | Absent skull vault | | **Neurological deficit** | Minimal | Severe (paralysis, incontinence) | Usually none | Incompatible with life | | **Maternal AFP** | Mildly elevated | Markedly elevated (>3 MoM) | Normal | Markedly elevated | | **Skin coverage** | May be present | Usually absent | Present | | **Prognosis** | Better | Poor (50% mortality, severe morbidity) | Excellent | Lethal | **High-Yield:** The presence of **neural tissue in the herniated sac** is the defining feature that distinguishes myelomeningocele from meningocele. The elevated AFP and exposed spinal cord elements clinch this diagnosis. ### Embryological Basis 1. Neural tube fails to close completely at the lumbosacral region (weeks 3–4) 2. Ectoderm over the defect does not fuse 3. Meninges and spinal cord herniate through the vertebral defect 4. Exposed neural tissue leads to neuronal damage and loss of function below the lesion **Clinical Pearl:** Myelomeningocele is the most common open neural tube defect compatible with life. It is associated with Arnold–Chiari malformation (hindbrain herniation), hydrocephalus, and tethered spinal cord. ### Prevention **Mnemonic:** FOLIC — **F**olate supplementation (400 μg daily, 4 mg if prior NTD), **O**ptimal glycemic control (if diabetic), **L**ow maternal BMI, **I**ncreased folic acid in high-risk populations, **C**ontrol of anticonvulsants (phenytoin, valproate are teratogenic) **Key Point:** Periconceptional folic acid supplementation reduces NTD risk by ~70%. Women with prior NTD should receive 4–5 mg daily. 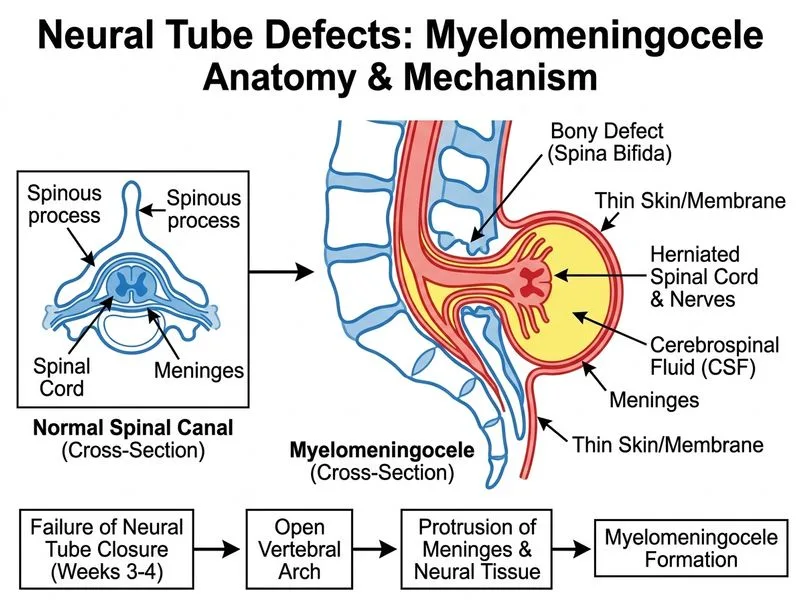
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.