## Diagnosis: Anencephaly – Embryological Timing ### Clinical Presentation The vignette describes: - Absence of cerebral hemispheres, brainstem, and skull vault - Exposed neural tissue covered by thin membrane ('area cerebrovasculosa') - Markedly elevated maternal AFP (>6 MoM is typical for anencephaly) - Risk factors: poorly controlled diabetes, phenytoin exposure ### Embryological Basis of Anencephaly **Key Point:** Anencephaly results from failure of the **cranial neuropore** to close during weeks 3–4 of embryogenesis. The cranial neuropore is the rostral (anterior) end of the neural tube and normally closes by day 24–25 [cite:Langman's Embryology Ch 17]. ### Timeline of Neural Tube Closure | Week | Event | Neuropore | Defect if Failed | |------|-------|-----------|------------------| | **Week 3 (days 17–21)** | Notochord and primitive streak form; neural plate appears | — | — | | **Week 3–4 (days 21–24)** | **Cranial neuropore closes** (rostral end) | Cranial | **Anencephaly** | | **Week 4–6 (days 24–28)** | **Caudal neuropore closes** (caudal end) | Caudal | Spina bifida, myelomeningocele | | **Week 7–8** | Secondary neurulation (filum terminale, sacrococcygeal region) | — | Sacral agenesis | **High-Yield:** The cranial neuropore closes BEFORE the caudal neuropore. Anencephaly is a defect of early closure (weeks 3–4), whereas spina bifida is a defect of later closure (weeks 4–6). ### Pathophysiology of Anencephaly 1. Failure of cranial neuropore closure → neural tissue remains exposed 2. Exposed neural tissue degenerates due to amniotic fluid exposure and trauma 3. Cerebral hemispheres, brainstem, and most of the skull fail to form 4. Only brainstem and midbrain remnants may persist 5. Thin vascular membrane ('area cerebrovasculosa') covers the defect ### Distinguishing from Other NTDs | Defect | Embryological Timing | Location | Contents | Prognosis | |--------|----------------------|----------|----------|----------| | **Anencephaly** | Weeks 3–4 (cranial neuropore) | Cranial vault | Absent brain/skull | Lethal (stillbirth or neonatal death) | | **Spina bifida / Myelomeningocele** | Weeks 4–6 (caudal neuropore) | Lumbosacral spine | Meninges ± spinal cord | Variable (compatible with life) | | **Encephalocele** | Weeks 3–4 (cranial) | Occipital or frontal | Meninges + brain tissue | Variable (depends on size/location) | **Clinical Pearl:** Anencephaly is incompatible with life. Most fetuses are stillborn; those born alive die within hours to days due to absent brainstem and respiratory centers. ### Risk Factors for NTDs **Mnemonic:** DEFECTS — **D**iabetes (uncontrolled, HbA1c >8%), **E**pilepsy drugs (phenytoin, valproate, carbamazepine), **F**olate deficiency, **E**thnicity (higher in Celtic populations), **C**ontrol of maternal temperature (fever in first trimester), **T**eratogenic drugs (retinoids, methotrexate), **S**pina bifida/NTD family history This patient has TWO major risk factors: 1. **Poorly controlled diabetes** (HbA1c 10.2%) — increases NTD risk ~2–10-fold 2. **Phenytoin exposure** — anticonvulsant teratogen (fetal hydantoin syndrome includes NTDs) ### Prevention **Key Point:** Periconceptional folic acid (400 μg daily, or 4–5 mg if prior NTD) reduces anencephaly risk by ~70%. Women with diabetes should achieve HbA1c <6.5% before conception. Anticonvulsant selection should favor levetiracetam or lamotrigine (lower NTD risk) over phenytoin. 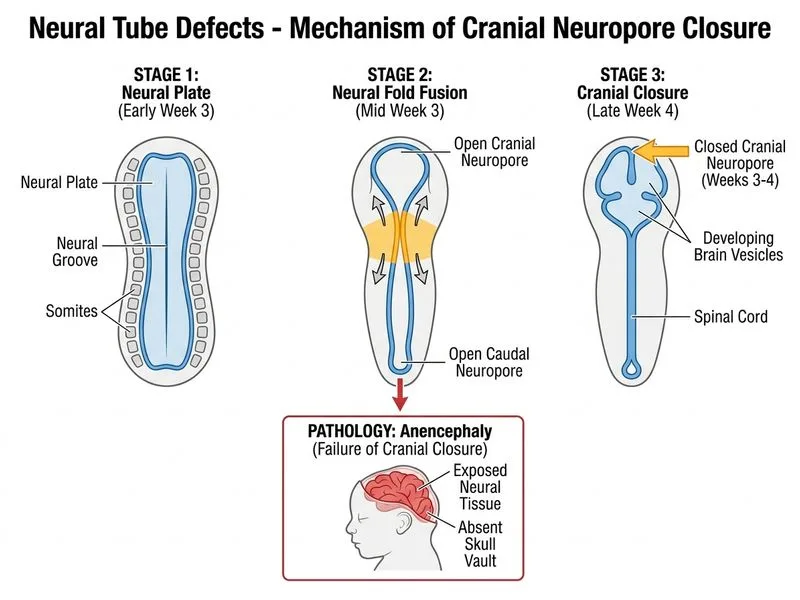
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.