## Meningocele vs. Meningomyelocele: The Critical Distinction ### Clinical Scenario Analysis The patient presents with a lumbosacral lesion that is: - Fluid-filled (suggesting CSF-containing sac) - Skin-covered (intact skin over the defect) - Detected prenatally with elevated AFP This description is consistent with **meningocele**. ### Structural Comparison | Feature | Meningocele | Meningomyelocele | |---------|-------------|------------------| | **Contents of sac** | CSF only; meninges only | Spinal cord and nerve roots | | **Dural integrity** | Dura and arachnoid intact but herniated | Dura is open; neural tissue exposed | | **Skin coverage** | Usually intact | May be intact or open | | **Neurological deficit** | Minimal to none | Significant (paralysis, sphincter loss) | | **Prognosis** | Excellent after repair | Variable; depends on level and extent | ### The Discriminating Feature **Key Point:** The presence of an **intact dura mater and arachnoid membrane** surrounding the sac is the hallmark of meningocele. In meningomyelocele, the dura is open and neural tissue herniates through the defect. **High-Yield:** Meningocele is a closed lesion (skin-covered, dura intact); meningomyelocele is an open lesion (dura defective, neural tissue exposed). This structural difference is the best discriminator. **Mnemonic:** **DURA** = **D**ural integrity distinguishes meningocele (intact) from meningomyelocele (open/defective). ### Clinical Implications **Clinical Pearl:** Meningocele has an excellent prognosis after surgical repair because the neural tissue is not involved. Meningomyelocele carries significant neurological morbidity because the spinal cord and nerve roots are malformed and exposed, leading to paralysis, sensory loss, and bowel/bladder dysfunction. [cite:Robbins 10e Ch 28] 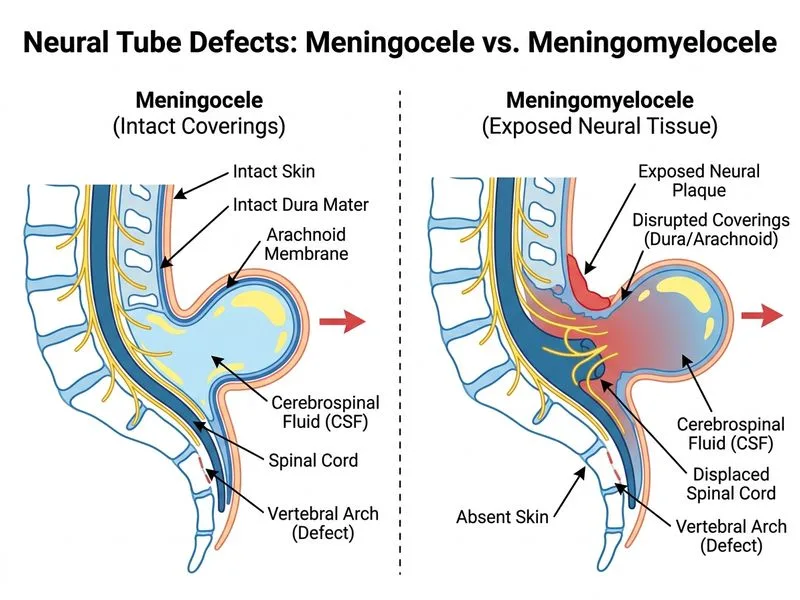
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.