## Microbiology of Orbital Cellulitis from Sinusitis ### Most Common Organisms **Key Point:** Orbital cellulitis secondary to paranasal sinusitis is typically polymicrobial, involving aerobic and anaerobic bacteria. The source (ethmoid/maxillary sinusitis) guides organism prediction. | Organism | Frequency | Source | Notes | |---|---|---|---| | *Streptococcus pneumoniae* | Most common (30–40%) | Sinusitis, hematogenous | Gram-positive coccus; penicillin-resistant strains common in India | | *Staphylococcus aureus* | Common (20–30%) | Sinusitis, skin flora | MRSA prevalence increasing | | Anaerobes (*Peptostreptococcus*, *Prevotella*, *Bacteroides*) | 20–40% | Sinusitis, dental sources | Polymicrobial infections | | *Haemophilus influenzae* | Less common (5–10%) | Sinusitis | Declining due to Hib vaccination | | *Pseudomonas aeruginosa* | Rare (< 5%) | Immunocompromised, trauma, surgery | Not typical in immunocompetent patients | ### Why *Streptococcus pneumoniae* Is Most Likely - **High-Yield:** In sinusitis-related orbital cellulitis, *S. pneumoniae* is the single most common pathogen in immunocompetent adults. - The patient has chronic rhinosinusitis (predisposing factor) with acute orbital spread. - Gram-positive cocci are the predominant isolates in this setting. ## Empiric Antibiotic Regimen ### Recommended First-Line Therapy **Ceftriaxone 2 g IV 6-hourly + Vancomycin 15–20 mg/kg IV 8-hourly + Metronidazole 500 mg IV 8-hourly** ### Rationale for Each Agent | Agent | Coverage | Rationale | |---|---|---| | **Ceftriaxone** | *S. pneumoniae*, *H. influenzae*, Gram-negatives | Third-generation cephalosporin; good CNS/orbital penetration | | **Vancomycin** | MRSA, penicillin-resistant *S. pneumoniae* | Essential for resistant Gram-positive cocci; high prevalence in India | | **Metronidazole** | Anaerobes (*Peptostreptococcus*, *Prevotella*, *Bacteroides*) | Covers polymicrobial anaerobic component; good orbital penetration | **Clinical Pearl:** This triple-agent regimen covers the full spectrum of sinusitis-derived orbital cellulitis (aerobes + anaerobes) while awaiting culture results. ### Duration - IV antibiotics: **10–14 days minimum** (longer if abscess present). - Transition to oral (e.g., amoxicillin-clavulanate + metronidazole) only after clinical improvement. - Total course: 3–4 weeks. ## Why Other Options Are Incorrect **Warning:** Monotherapy or dual therapy is inadequate for polymicrobial orbital cellulitis from sinusitis. ### Inadequate Regimens - **Piperacillin-tazobactam + ciprofloxacin:** Overkill for *Pseudomonas* coverage (rare in immunocompetent patients); misses anaerobes; fluoroquinolones have poor anaerobic coverage. - **Clindamycin monotherapy:** Covers anaerobes and some Gram-positives, but insufficient coverage of *S. pneumoniae* (especially resistant strains) and Gram-negatives. - **Amoxicillin-clavulanate monotherapy:** Inadequate for resistant *S. pneumoniae*, no vancomycin coverage, and insufficient anaerobic coverage in polymicrobial infections. 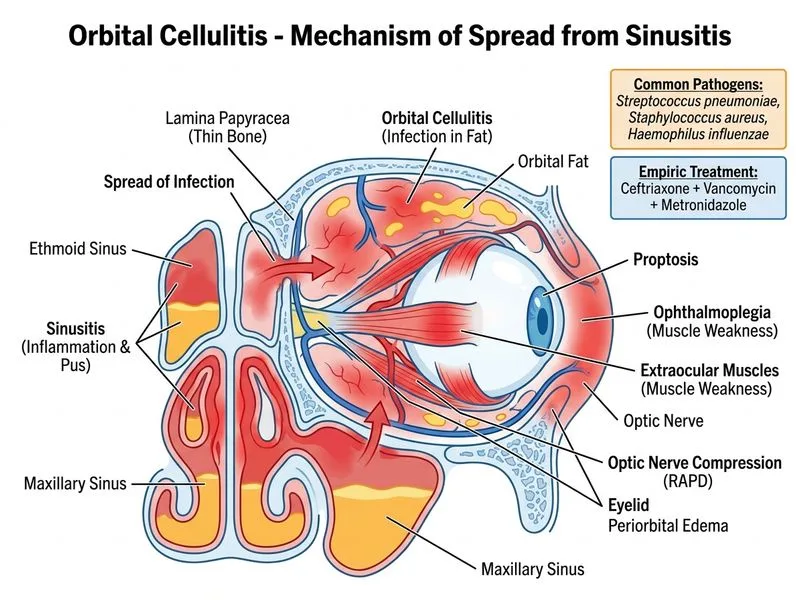
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.