## Orbital Cellulitis: Source Identification ### Clinical Clue Recognition **Key Point:** The combination of recent URTI, ethmoid sinus opacification on imaging, and medial rectus involvement (cranial nerve III territory) strongly suggests **ethmoid sinusitis with direct orbital extension**. ### Anatomical Basis for Ethmoid Sinusitis as Primary Source ```mermaid flowchart TD A[Ethmoid sinusitis]:::outcome --> B[Thin lamina papyracea separates ethmoid from orbit]:::outcome B --> C[Direct spread through bone erosion or via valveless ophthalmic veins]:::outcome C --> D[Orbital cellulitis]:::urgent D --> E[Medial rectus muscle inflammation/edema]:::action E --> F[Ophthalmoplegia: medial rectus palsy]:::outcome A --> G[Upper respiratory tract infection]:::outcome G --> H[Ethmoid sinusitis: most common source in children and adults]:::action ``` ### Sources of Orbital Cellulitis: Frequency & Anatomy | Source | Frequency | Mechanism | Imaging Clue | |--------|-----------|-----------|---------------| | **Ethmoid sinusitis** | 70–80% | Thin lamina papyracea; direct extension | Sinus opacification, air-fluid level | | Maxillary sinusitis | 10–15% | Inferior orbital wall erosion | Inferior sinus involvement | | Frontal sinusitis | 5–10% | Anterior orbital wall erosion | Superior sinus involvement | | Sphenoid sinusitis | <5% | Posterior extension; rare | Posterior sinus involvement | | Dacryocystitis | <5% | Lacrimal sac rupture; medial canthal source | Medial canthal swelling, lacrimal sac enlargement | | Hematogenous seeding | <5% | Bacteremia from distant source | No sinus involvement | | Preseptal cellulitis | Rare | Requires orbital septum breach | Septum intact on imaging | **High-Yield:** Ethmoid sinusitis is the **single most common source** of orbital cellulitis in both children and adults. The lamina papyracea is thin and easily eroded by infection. ### Why Ethmoid Sinusitis in This Case? 1. **Recent URTI:** Viral URTI → secondary bacterial sinusitis (ethmoid most common) 2. **CT findings:** Opacification of ethmoid sinuses with air-fluid level is pathognomonic 3. **Medial rectus involvement:** The medial rectus is adjacent to the medial orbital wall, which is the lamina papyracea (boundary between ethmoid sinus and orbit) 4. **Pattern of ophthalmoplegia:** Medial and lateral rectus involvement suggests mass effect from medial orbital inflammation (consistent with medial orbital wall source) **Clinical Pearl:** Medial rectus and lateral rectus palsies together suggest a **medial orbital mass or inflammation**, which is typical of ethmoid sinusitis spreading through the lamina papyracea. ### Microbiology of Ethmoid Sinusitis | Organism | Frequency | |----------|----------| | *Streptococcus pneumoniae* | 30–40% | | *Staphylococcus aureus* | 20–30% | | *Haemophilus influenzae* | 10–15% | | Anaerobes | 10–20% | | *Streptococcus pyogenes* | 5–10% | ### Management of Ethmoid Sinusitis–Derived Orbital Cellulitis 1. **IV antibiotics:** Ceftriaxone + Vancomycin ± Metronidazole (as above) 2. **Imaging:** CT/MRI to assess for: - Loculated abscess (requires drainage) - Lamina papyracea erosion - Posterior extension toward cavernous sinus 3. **ENT consultation:** For possible functional endoscopic sinus surgery (FESS) to drain infected ethmoid air cells and prevent recurrence 4. **Duration:** 2–3 weeks IV antibiotics, then oral for 2–4 weeks total **Warning:** Do NOT confuse ethmoid sinusitis (70% of orbital cellulitis) with cavernous sinus thrombosis (a *complication* of orbital cellulitis, not a primary source). Cavernous sinus thrombosis presents with **bilateral** orbital signs, altered mental status, and high mortality. [cite:Yanoff & Duker Ophthalmology 6e Ch 12; Park 26e Ch 16] 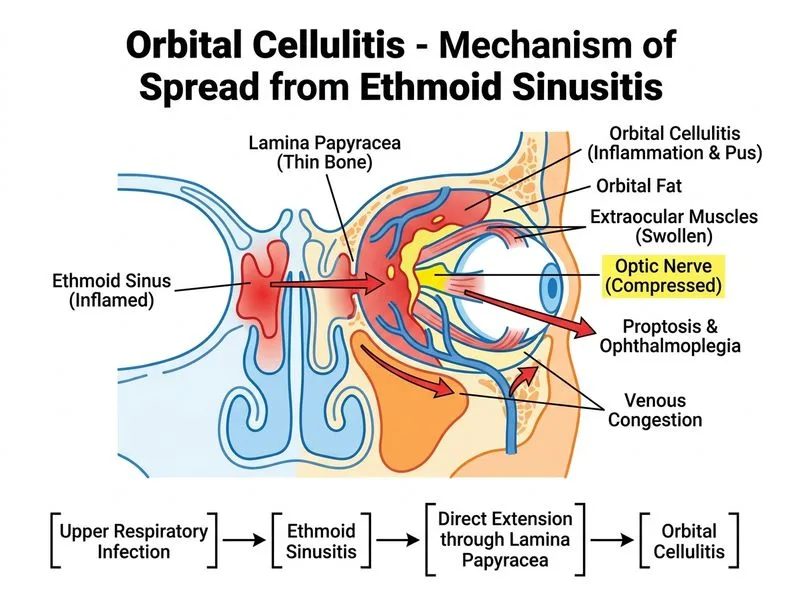
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.