## Clinical Context: Treatment Failure in Orbital Cellulitis **Key Point:** Failure to improve after 48–72 hours of appropriate IV antibiotics in orbital cellulitis warrants urgent reassessment. Imaging-guided aspiration is the next step to identify abscess formation, obtain culture for organism identification and sensitivities, and guide targeted therapy. ## Why This Patient Is Not Improving Possible reasons for treatment failure: 1. **Localized abscess formation** — requires drainage for cure 2. **Resistant organism** — MRSA, fungal, or atypical pathogen not covered by empiric regimen 3. **Inadequate antibiotic penetration** — abscess wall limits drug diffusion 4. **Underlying source not addressed** — untreated sinusitis (this patient has chronic rhinosinusitis) 5. **Immunocompromised state** — not evident here, but must be considered **High-Yield:** Imaging-guided aspiration serves dual purposes: (1) diagnostic—culture and sensitivities, (2) therapeutic—drainage of loculated pus. ## Management Algorithm for Treatment Failure ```mermaid flowchart TD A[Orbital cellulitis on IV antibiotics]:::outcome --> B{Clinical improvement<br/>at 48-72 hours?}:::decision B -->|Yes| C[Continue IV antibiotics<br/>2-3 weeks total]:::action B -->|No| D[Repeat imaging<br/>CT ± MRI]:::action D --> E{Abscess or<br/>loculation?}:::decision E -->|Yes| F[Imaging-guided aspiration<br/>or surgical drainage]:::action E -->|No| G[Review antibiotic coverage<br/>Consider resistant organism]:::action F --> H[Culture & sensitivities<br/>Adjust antibiotics]:::action G --> I[Change antibiotics based<br/>on clinical suspicion]:::action H --> J[Reassess at 48 hours]:::decision I --> J J -->|Improvement| K[Continue therapy<br/>4-6 weeks total]:::action J -->|No improvement| L[Surgical drainage]:::action ``` ## Imaging-Guided Aspiration: Technique & Yield | Aspect | Detail | |--------|--------| | **Imaging modality** | CT or ultrasound guidance (CT preferred for deeper lesions) | | **Needle size** | 18–22 gauge | | **Diagnostic yield** | 70–80% for culture-positive cases | | **Therapeutic benefit** | Immediate decompression; reduces intraorbital pressure | | **Complications** | Rare; hemorrhage, infection spread (< 1%) | **Clinical Pearl:** In this patient, chronic rhinosinusitis is a predisposing factor. Imaging-guided aspiration not only drains pus but also allows identification of the causative organism, which may be unusual (e.g., *Mucor*, *Aspergillus*, anaerobes). ## Why Other Options Are Incorrect - **Continuing same antibiotics:** Violates the "no improvement in 72 hours" rule. Abscess requires drainage; antibiotics alone cannot penetrate loculated pus adequately. - **Switching to oral antibiotics:** Premature de-escalation in a patient with treatment failure. Oral drugs achieve lower orbital tissue levels than IV. - **Enucleation:** Unnecessary and mutilating. Orbital cellulitis does not require eye removal; abscess drainage and targeted antibiotics are curative. **Warning:** Do not confuse orbital cellulitis with orbital abscess. Both present similarly, but abscess requires drainage in addition to antibiotics. [cite:Orbit & Neuro-ophthalmology, AIIMS protocols; Khurana Comprehensive Ophthalmology] 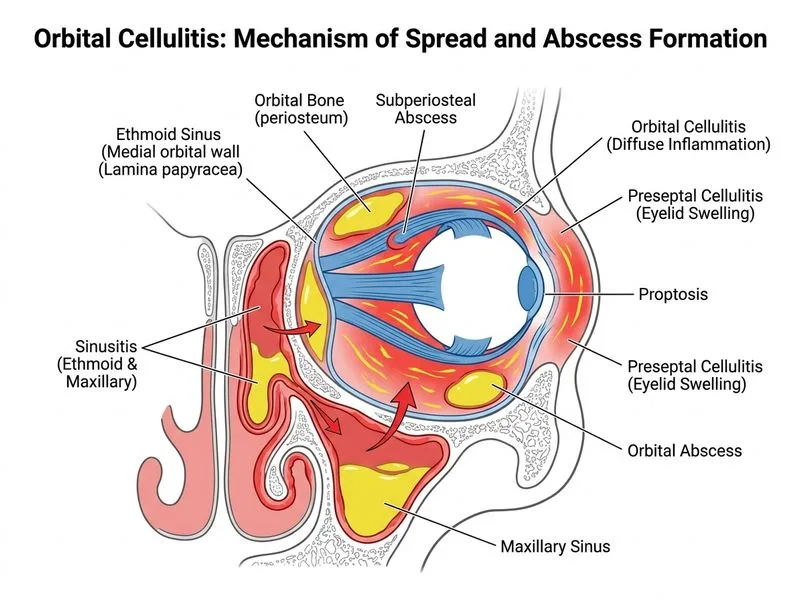
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.