## Clinical Diagnosis: Mucormycosis **Key Point:** The clinical triad of **uncontrolled diabetes + black necrotic palatal eschar + acute orbital cellulitis with ophthalmoplegia** is pathognomonic for **rhinocerebral mucormycosis** caused by *Rhizopus* species. ## Pathognomonic Features | Feature | Significance | | --- | --- | | Black necrotic eschar on palate | Pathognomonic for mucormycosis; indicates tissue necrosis from angioinvasion | | Uncontrolled diabetes (HbA1c 11.2%) | Primary risk factor; hyperglycemia impairs neutrophil function | | Complete ophthalmoplegia | Indicates cavernous sinus involvement or orbital apex syndrome | | Fixed, dilated pupil | CN III palsy from cavernous sinus thrombosis | | Acute presentation (hours to days) | Mucormycosis progresses rapidly; delays are fatal | **High-Yield:** *Rhizopus* is the most common cause of mucormycosis (60–70% of cases). It is angioinvasive, causing vascular thrombosis and tissue necrosis. ## Why Amphotericin B is Essential **Mnemonic:** **RAPID** management of mucormycosis — **R**hizopus identification, **A**mphotericin B IV, **P**ancreatic/endocrine control (glucose), **I**mmediate debridement, **D**aily monitoring for progression. 1. **Liposomal amphotericin B** is the gold standard for invasive mucormycosis 2. Dosing: 5–10 mg/kg/day IV 3. High-dose therapy is critical; mortality is >50% even with treatment 4. Voriconazole and posaconazole are NOT effective against *Rhizopus* ## Why Orbital Debridement is Urgent **Clinical Pearl:** Mucormycosis is one of the few orbital emergencies where debridement must occur **within hours** of diagnosis. Angioinvasion causes rapid tissue death; delaying surgery by even 24 hours significantly worsens prognosis. - Debridement removes necrotic tissue and improves drug penetration - Repeat debridements may be needed - Aggressive glycemic control (insulin infusions) is also critical ## Why Other Organisms Are Wrong | Organism | Why It's Wrong | | --- | --- | | *Pseudomonas aeruginosa* | Does not cause palatal necrosis or angioinvasion; ceftazidime would be used for bacterial cellulitis, not fungal | | *Staphylococcus aureus* | Causes bacterial cellulitis, not tissue necrosis with eschar; no palatal involvement | | *Aspergillus fumigatus* | Causes chronic invasive aspergillosis in immunocompromised patients, not acute angioinvasive disease with palatal eschar; voriconazole is the drug of choice for aspergillosis, not mucormycosis | [cite:Kanski's Clinical Ophthalmology 9e Ch 16; Harrison 21e Ch 207] 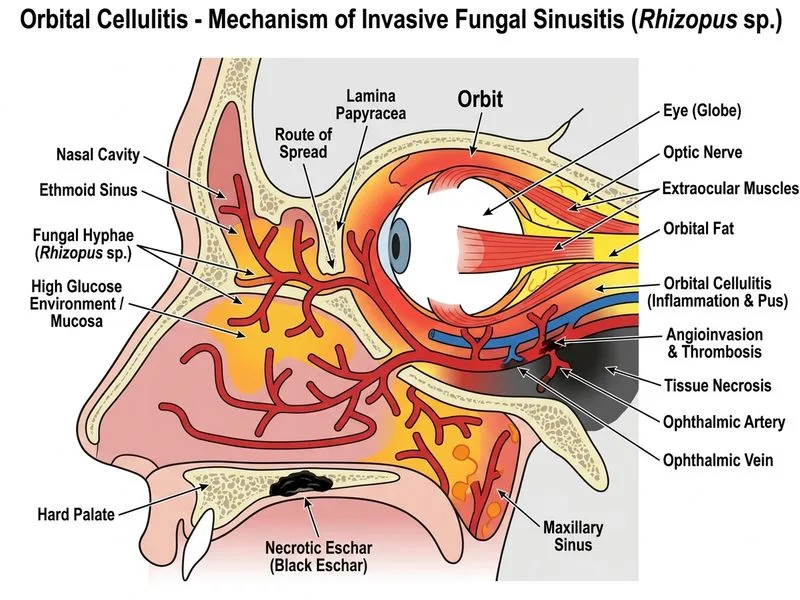
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.