## Organophosphate Poisoning: Acute Management Protocol **Key Point:** Organophosphate compounds irreversibly inhibit acetylcholinesterase, causing accumulation of acetylcholine at cholinergic synapses (muscarinic and nicotinic effects). ### Clinical Presentation (SLUDGE Syndrome) - **S**alivation, **L**acrimation, **U**rination, **D**efecation, **G**astrointestinal upset, **E**mesis - Miosis (pinpoint pupils) - Muscle fasciculations and weakness (nicotinic) - Bradycardia and bronchospasm (muscarinic) - Altered consciousness in severe cases ### Treatment Algorithm ```mermaid flowchart TD A[Organophosphate Exposure]:::outcome --> B[Decontamination + Remove clothing]:::action B --> C[Establish airway, O₂, IV access]:::action C --> D[Atropine 2–5 mg IV bolus]:::action D --> E{Signs of atropinization?}:::decision E -->|No| F[Repeat Atropine q5–10 min]:::action E -->|Yes| G[Start Pralidoxime 1 g IV]:::action G --> H[Pralidoxime 500 mg–1 g IV q4–6h]:::action H --> I[Monitor cholinesterase recovery]:::outcome ``` ### Drug Roles | Drug | Mechanism | Timing | Notes | | --- | --- | --- | --- | | **Atropine** | Muscarinic antagonist | First-line, immediate | Relieves salivation, bronchospasm, bradycardia; does NOT affect nicotinic effects (fasciculations, weakness) | | **Pralidoxime (2-PAM)** | Nucleophilic oxime; reactivates acetylcholinesterase by removing phosphoryl group | Within 24–48 hrs (ideally <6 hrs) | Effective only if enzyme-phosphate bond not yet "aged"; addresses both muscarinic AND nicotinic effects | **High-Yield:** Atropine is ESSENTIAL and MUST be given first. Pralidoxime is adjunctive and works best when given early, before "aging" of the enzyme-inhibitor complex (which varies by agent: minutes to hours). **Clinical Pearl:** The presence of muscle fasciculations and weakness (nicotinic signs) indicates severe poisoning and reinforces the need for early pralidoxime, as atropine alone cannot reverse nicotinic blockade. **Warning:** Pralidoxime alone is insufficient — atropine is required to manage life-threatening muscarinic effects (bronchospasm, bradycardia, hypersalivation). Neostigmine is contraindicated as it would worsen cholinergic excess. [cite:Harrison 21e Ch 481] 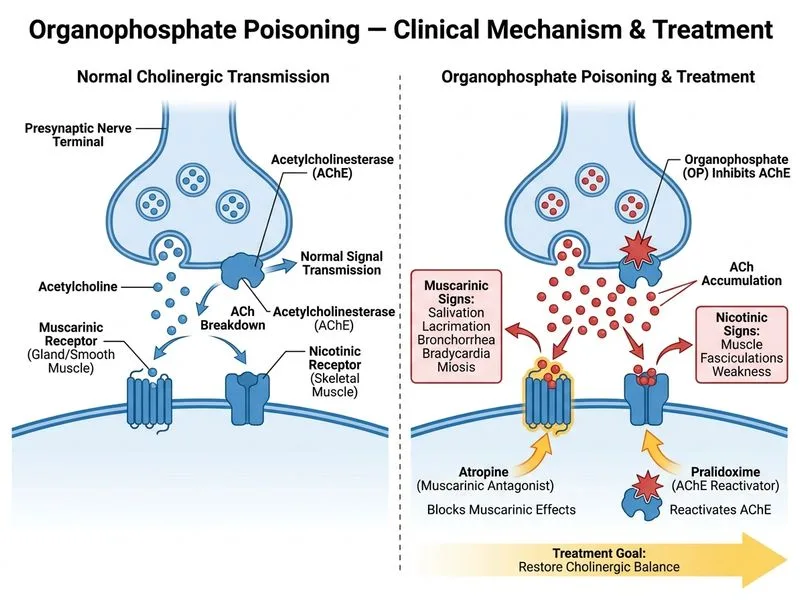
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.