## Severe Organophosphate Poisoning with Respiratory Failure ### Clinical Assessment **Key Point:** This patient has **severe organophosphate poisoning with impending respiratory failure** despite initial atropine therapy. The indicators are: - Respiratory rate 32/min (tachypnea) - SpO₂ 85% (hypoxemia) - Persistent bronchospasm (despite 6 mg atropine) - Muscle fasciculations (nicotinic effects) - Bradycardia (42 bpm) — still inadequately controlled ### Why Intubation Is Urgent 1. **Respiratory failure is imminent:** SpO₂ 85% with RR 32 indicates severe hypoxemia and work-of-breathing exhaustion. 2. **Atropine alone cannot reverse nicotinic effects** (muscle weakness, paralysis) — the patient may lose the ability to protect the airway or maintain spontaneous ventilation. 3. **Pralidoxime requires a secured airway** to be safely administered in a patient with severe respiratory compromise; intubation must precede or accompany pralidoxime. ### Management Sequence ```mermaid flowchart TD A[Severe OP poisoning + respiratory distress]:::outcome --> B{SpO₂ adequate?}:::decision B -->|No - SpO₂ <90%| C[Immediate intubation]:::urgent B -->|Yes - SpO₂ >90%| D[Continue atropine titration]:::action C --> E[Mechanical ventilation]:::action E --> F[Pralidoxime 1 g IV over 5-10 min]:::action D --> G{Atropinization achieved?}:::decision G -->|Yes| F G -->|No| H[Repeat atropine q5-10 min]:::action H --> G F --> I[Supportive care + monitoring]:::action ``` ### Atropine Dosing in This Context **High-Yield:** The patient has received 6 mg atropine with **partial response**. This is not "atropine failure" — it reflects: - **Severe poisoning** (high acetylcholinesterase inhibition) - **Need for higher cumulative doses** (organophosphate poisoning often requires 100–200+ mg atropine) - **Concurrent respiratory failure** that cannot be reversed by atropine alone Continuing atropine every 3 minutes while SpO₂ is 85% **delays life-saving intubation** and risks complete respiratory collapse. ### Pralidoxime Timing **Clinical Pearl:** Pralidoxime is given **after the airway is secured** in a patient with respiratory failure. The sequence is: 1. **Intubate** (secure airway, provide mechanical ventilation) 2. **Administer pralidoxime** (reactivate acetylcholinesterase, address nicotinic effects) 3. **Continue atropine titration** (maintain muscarinic blockade) Pralidoxime is **not a substitute for intubation** — it does not improve oxygenation or ventilation directly. ### Why Not Cricothyrotomy? Cricothyrotomy is a **surgical emergency airway** reserved for: - Failed intubation attempts - Anatomical contraindications to oral/nasal intubation - Severe facial/laryngeal trauma In this case, **standard intubation is the appropriate airway technique** — there is no indication for surgical airway. Deferring pralidoxime until after cricothyrotomy is also unnecessary and delays treatment. ### Supportive Care Post-Intubation - **Mechanical ventilation:** Assist-control or synchronized intermittent mandatory ventilation (SIMV) - **Sedation:** Benzodiazepines (e.g., midazolam) ± neuromuscular blockade if needed for synchronization - **Continued atropine:** Titrate to maintain heart rate >60 bpm and control secretions - **Pralidoxime:** 1 g IV q4–6 hours × 24 hours (or longer if severe) - **Monitoring:** Continuous cardiac monitoring, frequent blood gas checks, pupil size, muscle strength 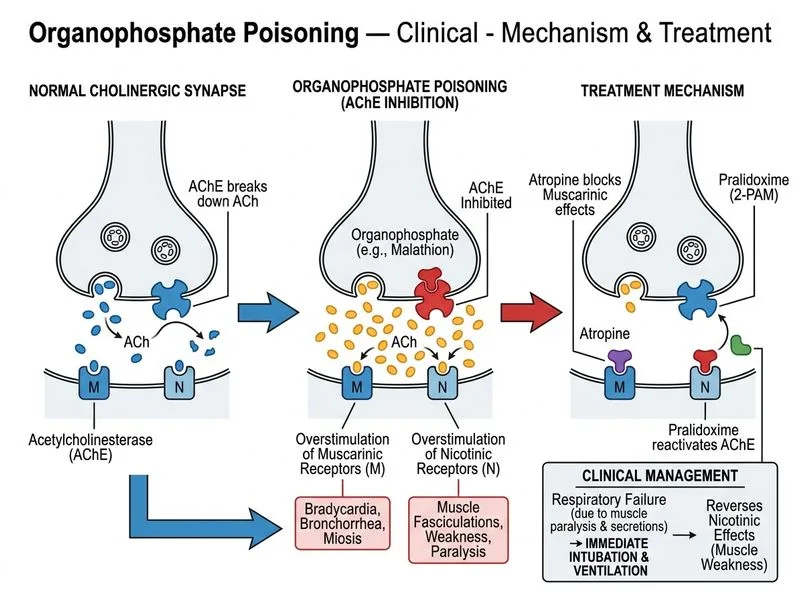
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.